Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2007. Reviewed by Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, 23 February 2014.
Compulsive skin picking is a disorder characterised by the repetitive picking of one's own skin to the point of causing open sores that may bleed and leave scarring. This condition is also known as dermatillomania, pathological skin picking and neurotic excoriation.
People suffering from compulsive skin picking may pick at normal skin variations such as freckles and moles, at pre-existing skin defects such as scabs, sores or acne blemishes, or in some cases imagined skin defects that are not actually visible by others. Individuals with compulsive skin picking not only use their fingernails to pick and scratch but may also use their teeth and/or other instruments such as tweezers, blades and pins. The compulsion to scratch, pick or peel pimples is called acne excorié and could be considered a subtype of compulsive skin picking. Although any part of the body may be attacked, often the face is the targeted area.
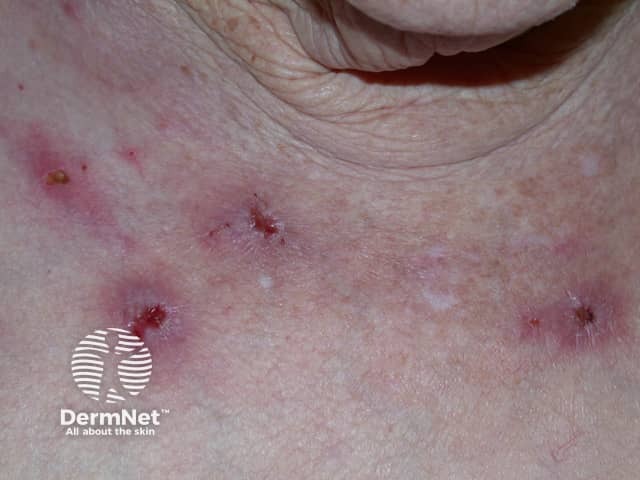
Compulsive skin picking
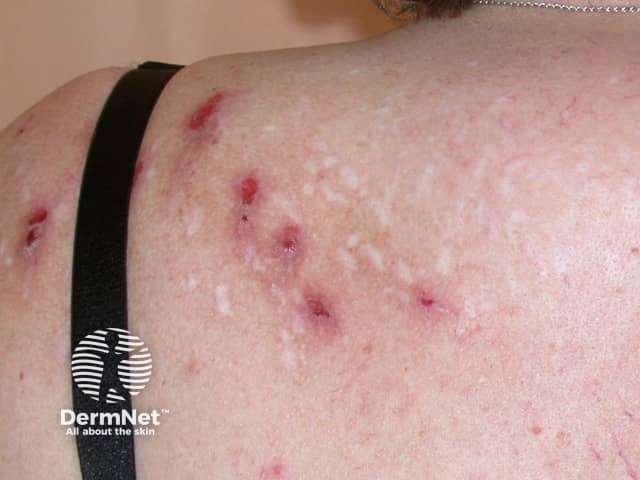
Compulsive skin picking
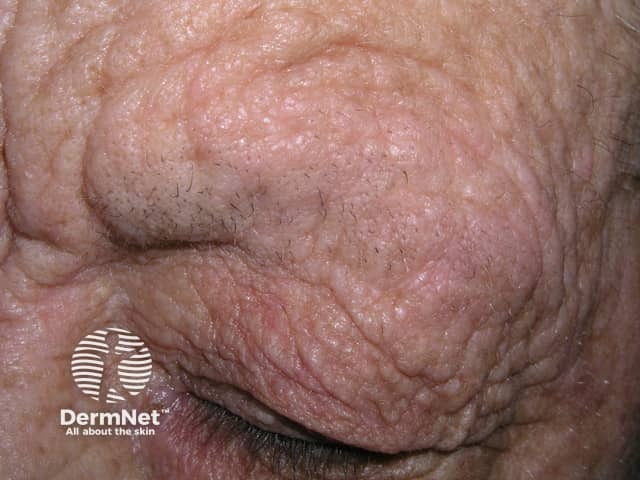
Compulsive skin picking
See more images of compulsive skin picking.
Individuals with compulsive skin picking often have a co-existing psychiatric disorder. The most common co-existing psychiatric conditions are major depression and anxiety disorders, especially obsessive-compulsive disorder (OCD). In one study, 52% of patients with compulsive skin picking were also diagnosed with OCD. An organic disease such as anaemia, uraemia or liver disease may also cause compulsive skin picking. It is essential for the doctor to consider all possible causes.
In many sufferers of compulsive skin picking, skin picking is preceded or accompanied by a high level of tension, anxiety or stress and a strong urge to itch or scratch. Often certain events or situations trigger skin-picking episodes. For some, the act of skin picking provides a feeling of relief or pleasure. Skin-picking episodes can be a conscious response to anxiety or may be done as an unconscious habit.
Compulsive skin picking appears to be more common in women than in men, and often starts in adolescence.
It may also be associated with methamphetamine or cocaine abuse.
Skin damage caused from compulsive skin picking can range from mild to extreme. Bleeding, bruising and secondary infections are not uncommon. In severe cases, patients may create wounds so large that they require hospitalised care. Compulsive skin picking often leads to permanent disfigurement, shame and social impairment. Sufferers will often try to hide the damaged caused to their skin by wearing make-up and/or clothes to cover the marks and scars. In extreme cases, they will avoid social situations to hide their condition from those around them.
Treatment for compulsive skin picking depends on the cause and the level of awareness the patient has regarding the problem. Compulsive skin picking stemming from a psychological disorder is best treated with psychotherapy. When compulsive skin picking is generally an unconscious habit the treatment of choice is a form of cognitive behaviour therapy called Habit Reversal Training (HRT).
Habit Reversal Training – this is a form of psychotherapy that helps patients to become more consciously aware of situations and events that trigger skin-picking episodes. Patients are then taught alternative behaviours in response to these situations and events.
Exposure and Response Prevention (ERP) – this is commonly used in the treatment of obsessive-compulsive disorders and is useful in cases of compulsive skin picking where the patient is already aware of the situations and events that cause skin-picking episodes. Most patients using this technique have already made significant recovery using HRT.
Medications used for the treatment of OCDs are also frequently used in compulsive skin picking. They are often used in conjunction with cognitive behaviour therapy. The drugs of choice are the selective serotonin reuptake inhibitors (SSRIs) such as fluoxetine, paroxetine, sertraline and fluvoxamine. N-acetylcysteine has also been reported to be effective.