Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Vidette Wong, Core Medical Trainee, Department of Dermatology, Antrim Area Hospital, Belfast, Northern Ireland, United Kingdom. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. September 2019.
Introduction Demographics Causes Clinical features Diagnosis Treatment Outcome
Patients with compulsive hand washing perform excessive and repetitive washing of their hands in an attempt to relieve severe distress associated with obsessive and irrational fears of contamination.
Repeated hand washing often causes marked skin changes of the hands or exacerbates pre-existing skin conditions. Compulsive hand-washing is often a debilitating psychodermatological condition that interferes with the patient’s activities of daily living and quality of life.

Contact dermatitis due to hand washing
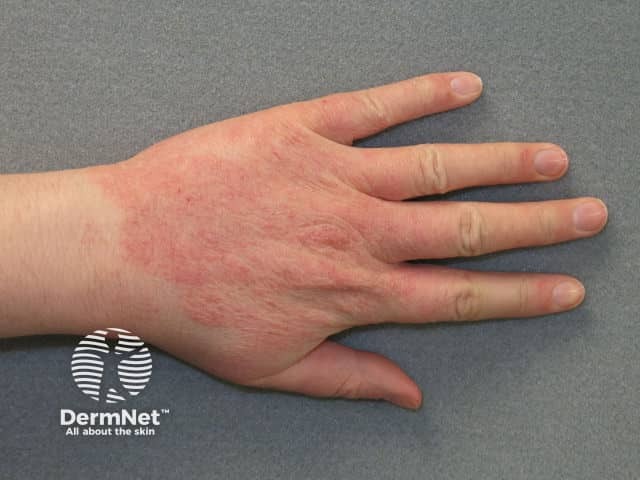
Contact dermatitis due to washing
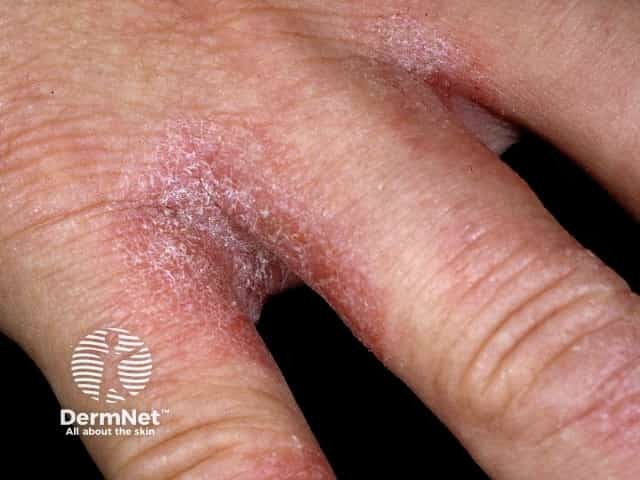
Hand dermatitis due to excessive exposure to water
Compulsive hand washing occurs in patients with obsessive–compulsive disorder (OCD).
OCD is characterised by obsessive and repetitive thoughts, images, or urges with compulsions consisting of repetitive rituals and behaviours; these are performed to excess to reduce anxiety and distress related to the person's obsessions.
OCD is a common disorder that has an estimated worldwide lifetime prevalence of 2% in the general population [1]. Approximately 16% of all patients with OCD suffer from some form of washing compulsion, which is manifested by frequent long and ritualised compulsive hand washings up to 50–100 times daily [2].
The cause of OCD and compulsive hand washing remains uncertain and involves biological and psychosocial factors.
It is thought the neurotransmitter serotonin plays a role in the development of the OCD as multiple trials have shown selective serotonin reuptake inhibitors (SSRIs) to be effective for managing the symptoms of OCD [3,4].
Cognitive behavioural therapy has been applied to OCD, on the basis that compulsive behaviours are learned and conditioned according to several psychological models [3,4].
Compulsive hand washing can result in inflammatory, degenerative, and infective changes to the dorsal and palmar sides of the hands, usually manifesting as hand dermatitis. It can also exacerbate pre-existing skin conditions such as atopic dermatitis or allergic contact dermatitis.
Soaps, detergents, and other cleansers for recurrent hand washing can also result in irritant contact dermatitis.
Compulsive hand–washing may result in the clinical features of both acute and chronic hand dermatitis.
A careful history will reveal that the patient suffers from obsessive thoughts of contamination, fear of germs, or similar beliefs. They need to complete repeated cycles and rituals of handwashing to relieve anxiety from these obsessions.
Individuals are often aware that their compulsive behaviours are excessive, irrational, and time-consuming, but often do not seek help until late in their disease, at which point signs and symptoms have become chronic [3].
Compulsive hand washing is diagnosed and identified after taking a careful and thorough history and clinical examination. Patients should be approached tactfully and supportively.
The clinical manifestations of compulsive hand washing may appear similar to the following dermatological conditions (or these may be coexisting) including:
The main distinguishing feature of compulsive hand washing is the psychological component of obsessive thoughts and fears, with compulsive behaviours of repetitive hand washing that affect the individual’s daily life and quality of living.
The management of compulsive hand washing and OCD consists of a multi-faceted approach.
First-line treatment is selective SSRIs such as fluoxetine, sertraline, and paroxetine for at least a period of 3 months [3,4].
Psychological therapies are based on cognitive behavioural therapy, with exposure and response prevention. The individual works with the therapist to acknowledge their condition and face their fears and obsessive thoughts or feelings, without neutralising them with their compulsive behaviours. This is often guided in a step-by-step and personalised manner and using methods such as distraction techniques [3,4].
Counselling and OCD support groups may be helpful.
Hypnosis and other complementary therapies are also gaining recognition as part of the management of OCD [5].
The aim is to protect and manage the damaged skin, using:
Any coexisting skin condition should also be treated.
A close collaboration between the dermatologist, psychologist, and psychiatrist can achieve a favourable outcome for a patient suffering from compulsive hand washing.
Long-term longitudinal studies have reported varied symptomatic remission rates of OCD ranging from 32% to 70% [6].