Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2006. DermNet Update May 2021. Further minor update June 2023. Minor amendment by Ian Coulson, Dermatologist. July 2024.
Introduction
Demographics
Causes
Classification
In children
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Cutaneous T-cell lymphoma (CTCL) is the most common type of primary cutaneous lymphoma. It is a form of non-Hodgkin lymphoma in which malignant T-cells are initially localised to the skin with no evidence of extracutaneous disease at the time of diagnosis.
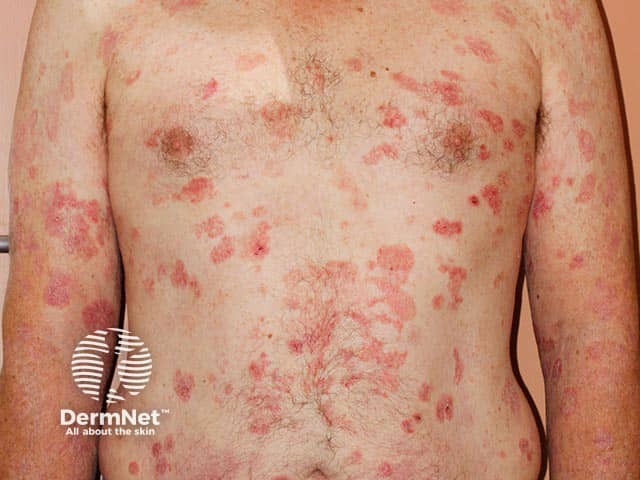
Cutaneous T-cell lymphoma
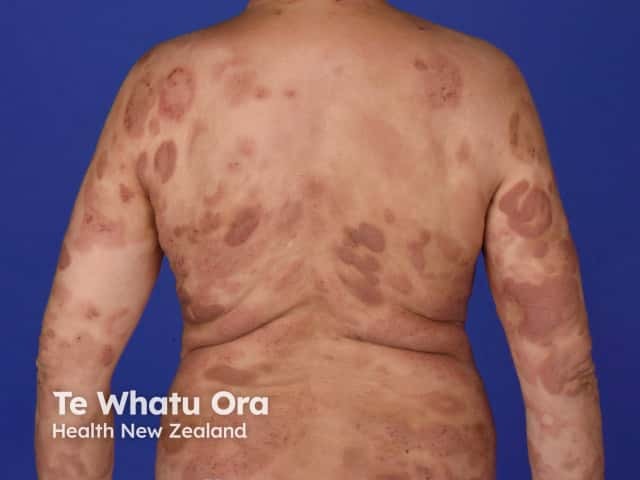
Mycosis fungoides
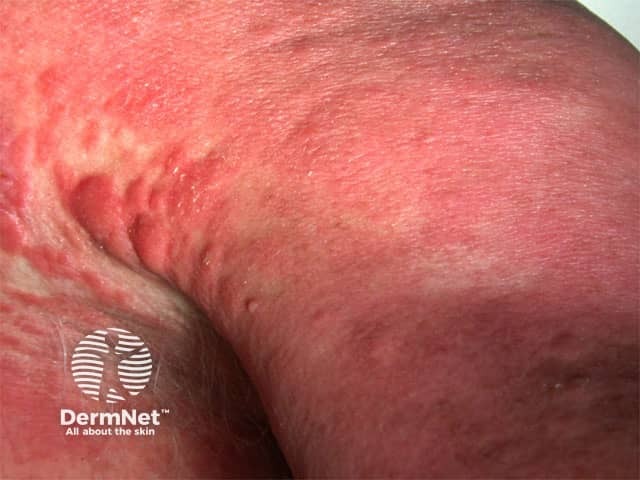
Sézary syndrome
Cutaneous T-cell lymphoma comprises 4% of all non-Hodgkin lymphomas and 75-80% of all primary cutaneous lymphomas. It shows a male predominance of 2:1. The incidence of CTCL increases with age, with an average age at diagnosis of 50–60 years.
The aetiopathogenesis of cutaneous T-cell lymphoma is unknown. Theories include a viral infection (eg, Epstein Barr virus, HTLV-1) causing a chronically heightened immune state, genetic changes (eg, HLA type), or chemical exposure (eg, medications).
Epigenetics regulates gene expression without altering the DNA sequence. Epigenetic studies of CTCL have identified changes in DNA methylation, histone modification, microRNAs and chromatin remodellers. One example is miR-155 which is overexpressed in malignant CTCL cells, especially in advanced stage disease, and treatments inhibiting this are in early clinical trials for tumour-stage mycosis fungoides, Sézary syndrome, and primary cutaneous anaplastic large-cell lymphoma.
An association between JAK inhibitors and malignancy (eg, T-cell lymphomas) is currently under investigation and is not fully understood. There have been rare cases of T-cell lymphomas reported in patients treated with JAK inhibitors, but the overall incidence appears to be low and causality has not been established.
An association between dupilumab and CTCL is also currently under investigation; causality has not been established.
The 2018 WHO-EORTC classification of cutaneous T-cell lymphomas is summarised in the following tables with links to specific DermNet webpages.
Indolent forms of CTCL |
Frequency (%) |
Prognosis: 5 year survival (%) |
39 |
88 |
|
Mycosis fungoides variants |
||
Folliculotropic MF |
5 |
75 |
Pagetoid reticulosis |
1 |
100 |
Granulomatous slack skin |
1 |
100 |
Primary cutaneous CD30+ LPD |
||
pcALCL |
8 |
95 |
[Lymphomatoid papulosis](/topics/lymphomatoid-papulosis |
12 |
99 |
Primary cutaneous CD4+ small/medium T-cell lymphoproliferative disorder* |
6 |
100 |
1 |
87 |
Aggressive forms of CTCL |
Frequency (%) |
Prognosis: 5 year survival (%) |
2 |
36 |
|
Adult T-cell leukaemia/lymphoma |
1 |
NDA |
1 |
16 |
|
Chronic active EBV infection in childhood |
1 |
NDA |
Primary cutaneous |
1 |
11 |
1 |
15 |
|
Primary cutaneous aggressive CD8+ cytotoxic T-cell lymphoma |
1 |
31 |
Primary cutaneous peripheral T-cell lymphoma NOS |
2 |
15 |
Primary cutaneous small-medium pleomorphic T-cell lymphoma is an example of a ‘Primary cutaneous peripheral T-cell lymphoma NOS’ with an excellent prognosis.
Cutaneous T cell lymphoma is rare in childhood, with lymphomatoid papulosis and mycosis fungoides variants being the most frequency.
Cutaneous T-cell lymphomas typically present as patches, papules, nodules, plaques, and/or tumours. Itch is reported by 80% of patients.
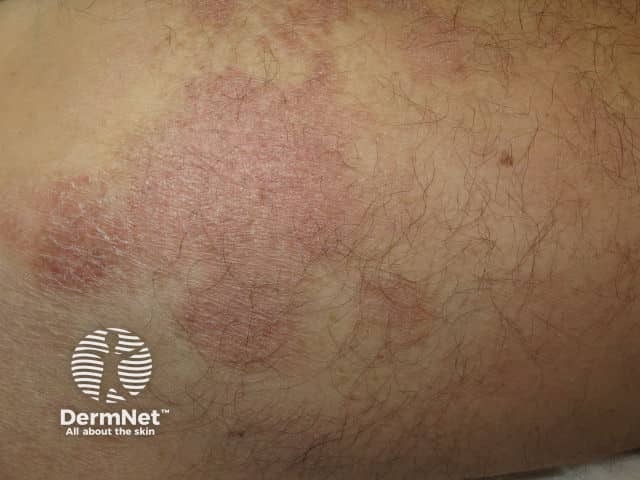
Patch stage mycosis fungoides
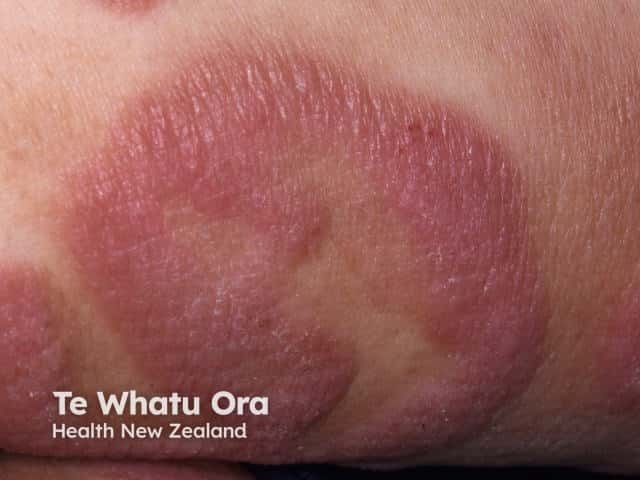
Plaque stage mycosis fungoides
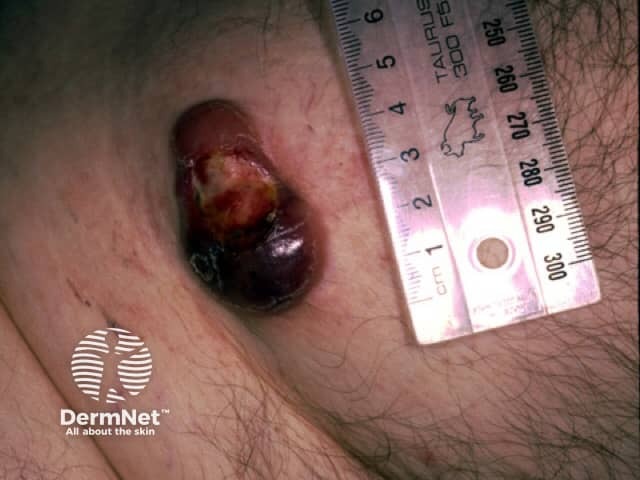
Tumour stage of CTCL
The diagnosis of cutaneous T-cell lymphoma is often delayed by months or years due to the indolent course, clinical similarity to inflammatory dermatoses, and subtle changes on histopathology.
Cutaneous T-cell lymphoma papules, nodules, and tumours may ulcerate and become necrotic, healing with varioliform scarring.
Extracutaneous spread affects 10%.
Quality of life can be significantly impacted due the economic burden of a chronic disease, or to symptoms such as itch and pain, psychological effects including anxiety and depression, and visible skin changes including hair loss.
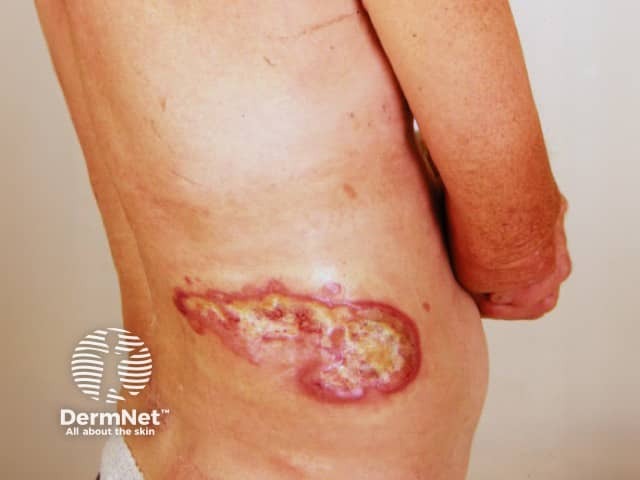
Ulcerated mycosis fungoides, tumour stage
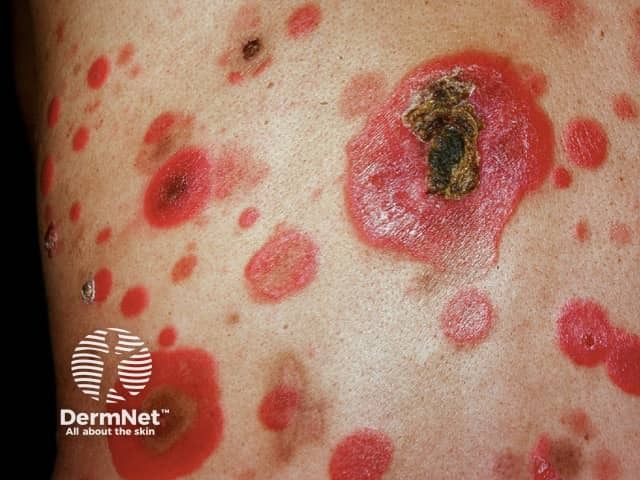
Ulcerated mycosis fungoides, plaque stage
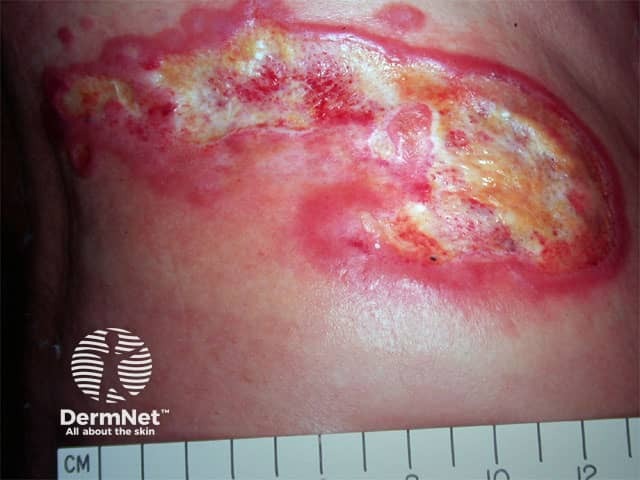
Ulcerated mycosis fungoides, tumour stage
Diagnosis of cutaneous T-cell lymphoma involves careful clinicopathological correlation. Multiple skin biopsies are often required to detect the characteristic histopathology changes, especially in the early patch stages. Further investigations may be performed on skin biopsy specimens including immunohistochemistry.
EBV, T-cell receptor (TCR) gene rearrangements, ALK, DUSP22-IRF4, and TP63 gene studies may be performed to confirm the diagnosis and predict the clinical course.
Enlarged lymph nodes may also be biopsied. Cutaneous T-cell lymphoma can cause harmless swelling, known as reactive or dermopathic lymphadenopathy, or malignant growth in the lymph nodes.
The blood count is normal in most patients with CTCL. An elevated white cell count is characteristic of Sézary syndrome and confirmed on flow cytometry. Some patients may require bone marrow biopsy.
Patients with advanced cutaneous T-cell lymphoma may undergo CT or MRI scans to determine whether the disease has affected internal organs.
Formal TNMB staging is recommended in some forms of CTCL.
Cutaneous T-cell lymphoma is regarded as treatable, not curable. Treatments considered will depend on the individual patient, specific type of CTCL, stage of disease, local expertise, and available drugs and equipment. There are no global consensus guidelines for treating CTCL.
Skin-directed topical treatments are the mainstay of early disease.
Cutaneous T-cell lymphoma typically follows a long slow course remaining confined to the skin, progressing over many years, and not usually life-threatening.
Some forms of CTCL progress more rapidly with a minority developing advanced disease including tumour formation, extracutaneous spread (10%), and progression to systemic lymphoma.