Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Vanessa Ngan, Staff Writer, 1998. Updated: Dr Nisal Punchihewa, Junior Medical Officer, Monash Medical Centre, Melbourne, Victoria, Australia; Dr Martin Keefe, Dermatologist and Assistant Editor. Copy edited by Gus Mitchell. February 2022
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Pityriasis lichenoides (PL) is an uncommon cutaneous rash of uncertain aetiology. The acute form, pityriasis lichenoides et varioliformis acuta (PLEVA), and the chronic form, pityriasis lichenoides chronica (PLC), sit at either end of a disease spectrum with many patients showing overlapping features.
The eponym Mucha–Habermann disease is sometimes applied to the entire spectrum of PL but is often reserved for the particularly severe ulcero-necrotic variant of PLEVA.
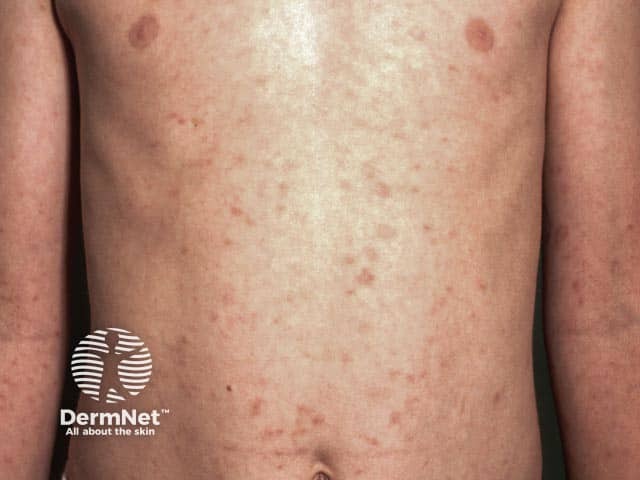
Pityriasis lichenoides chronica on the chest
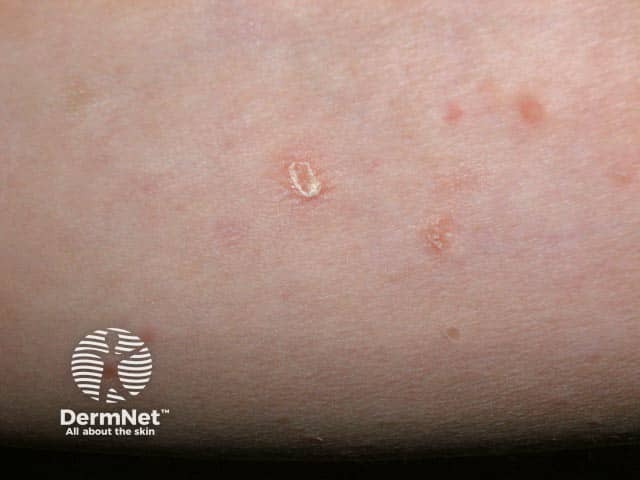
The mica-like scale in pityriasis lichenoides chronica
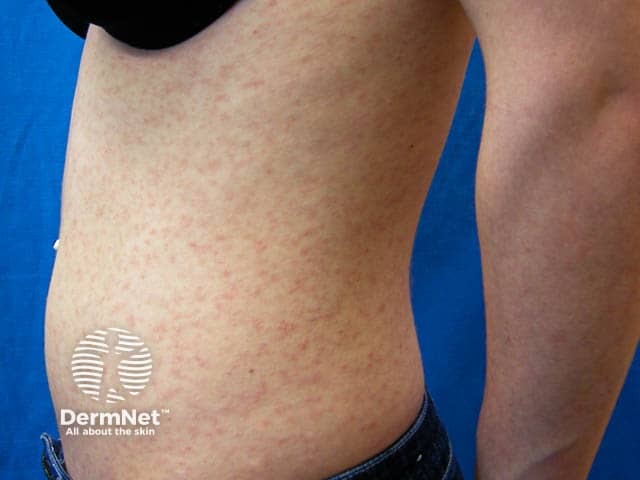
Widespread truncal pityriasis lichenoides chronica
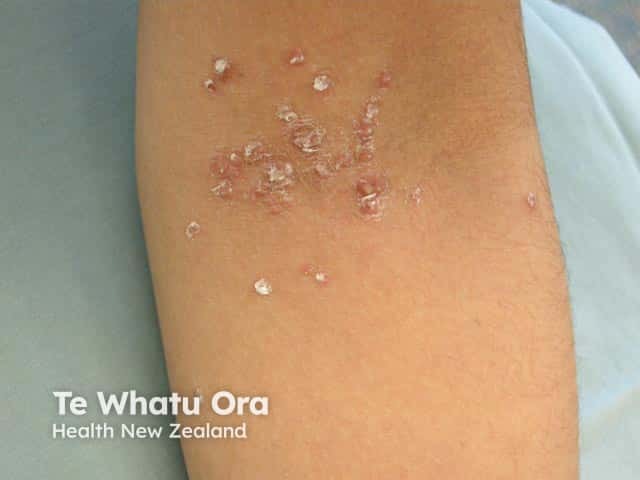
Mica-like scale in pityriasis lichenoides chronica
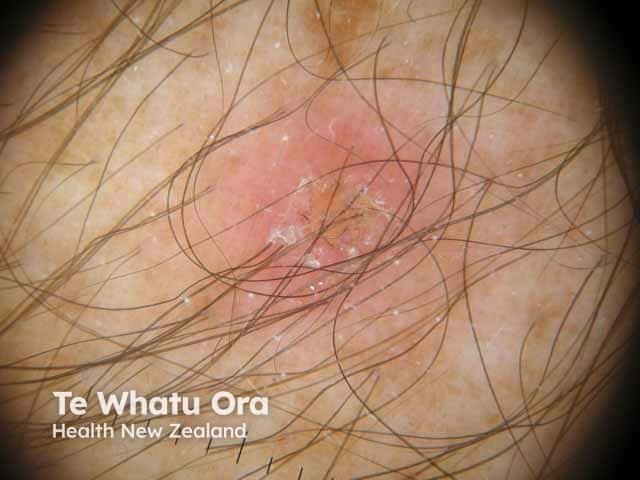
Pityriasis lichenoides acuta on dermoscopy
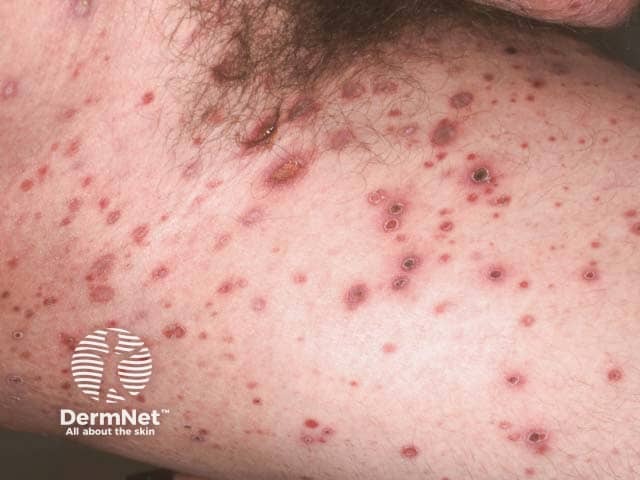
Ulcerated pityriasis lichenoides acuta
Click for more images of pityriasis lichenoides
The incidence of PL is unknown, but the disease is rare. It is most common in children and young adults under age 30 but can present at any age. There is a slight male predominance. All races are affected.
The cause of PL is unknown. The main hypotheses are that it may be:
PLEVA presents abruptly with a rapidly progressive rash:
PLC presents more slowly over several days with:
Patients often show features of both PLEVA and PLC, and PLEVA may evolve into PLC. Mucosal lesions have been reported.

Ulcerated pityriasis lichenoides acuta
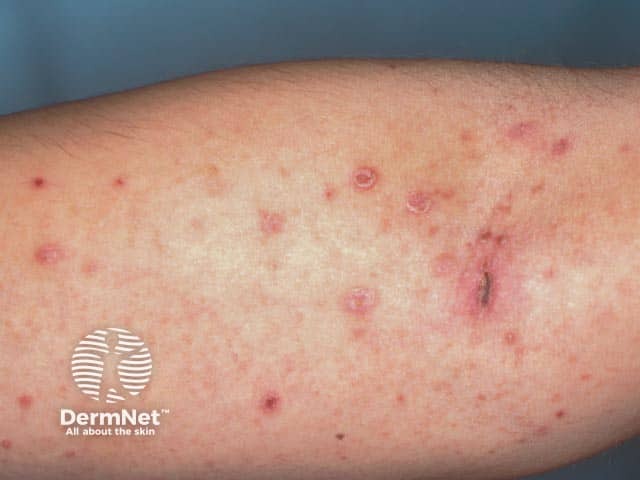
Pityriasis lichenoides acuta on the arm
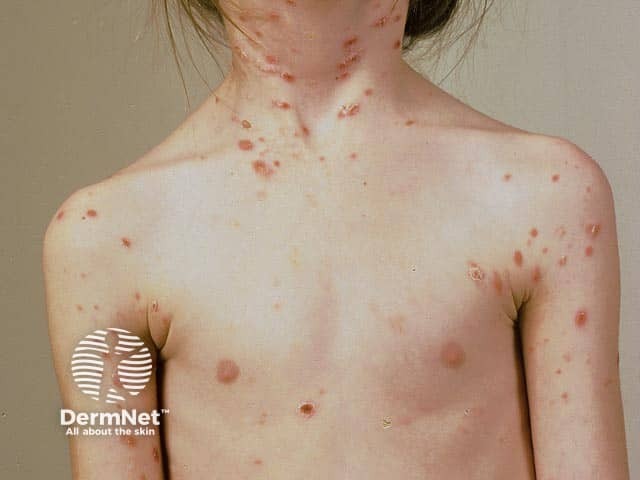
Pityriasis lichenoides acuta in a child
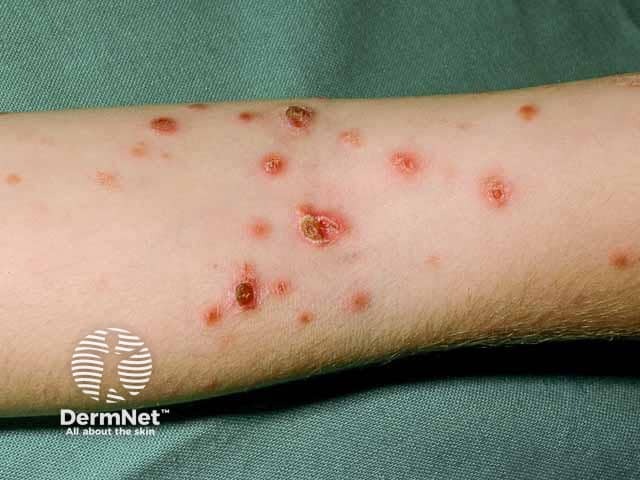
Ulcerated pityriasis lichenoides acuta on the arm
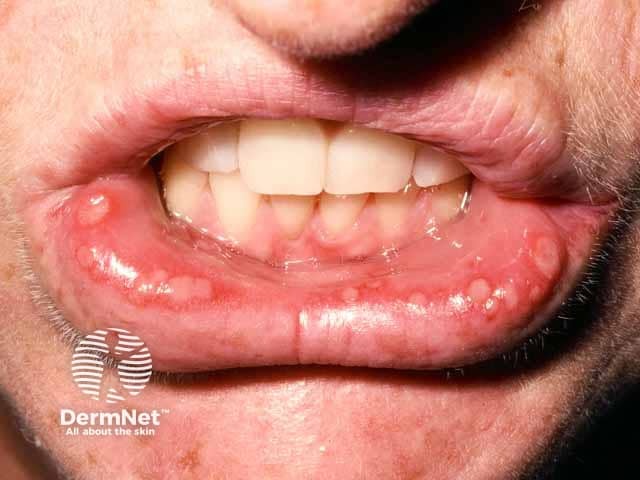
Mucosal ulcers in pityriasis lichenoides acuta
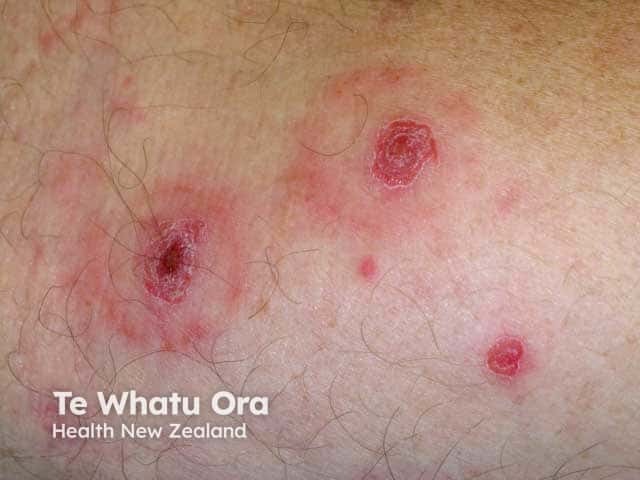
Eroded lesions in pityriasis lichenoides acuta
Dark-skinned patients, particularly children, may present with widespread hypopigmentation and prominent facial involvement. The definitive signs of pityriasis lichenoides may be very subtle.
The diagnosis can often be made on clinical grounds but is usually confirmed with a skin biopsy, which helps to exclude other important differential diagnoses.
Histological features of PLEVA include:
In PLC there is usually:
Dermoscopy may be useful, particularly to distinguish PLC from guttate psoriasis or pityriasis rosea.
Other tests, such as screening for viral, bacterial, and toxoplasma infection may be considered, depending on the severity of the presentation.
It is important to recognise that there have been no randomised controlled trials regarding treatment, and the natural history of pityriasis lichenoides makes interpretation of anecdotal reports difficult.
Pityriasis lichenoides et varioliformis acuta typically resolves within a few weeks. However, this can be variable and PLEVA may evolve into PLC or a scar. Pityriasis lichenoides chronica typically lasts several months, but some cases can wax and wane for several years.