Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Mark Duffill, Hamilton, New Zealand, 2008.
Introduction - panniculitis
Introduction - cytophagic histiocytic panniculitis
Clinical features
Causes
Diagnosis
Treatment
Panniculitis is a term usually referring to a disorder of the subcutaneous fat.
Cytophagic histiocytic panniculitis is an inflammatory condition of the subcutaneous fat. It is diagnosed after a biopsy has detected abnormal histiocytes which are engulfing other cells (such as red and white blood cells).
Cytophagic histiocytic panniculitis also affects other organs and is a life-threatening condition.
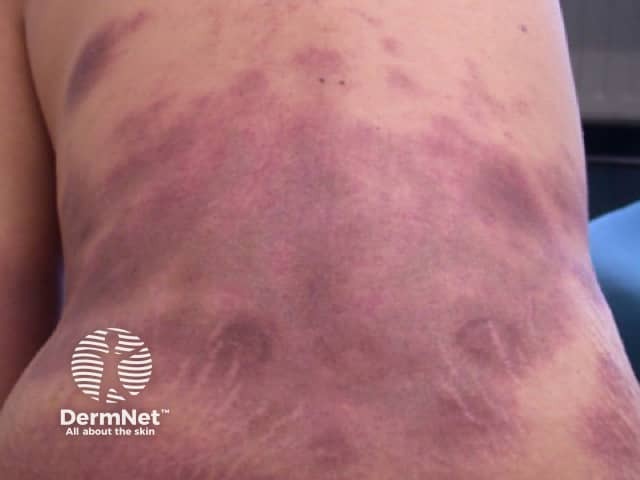
Cytophagic histiocytic panniculitis
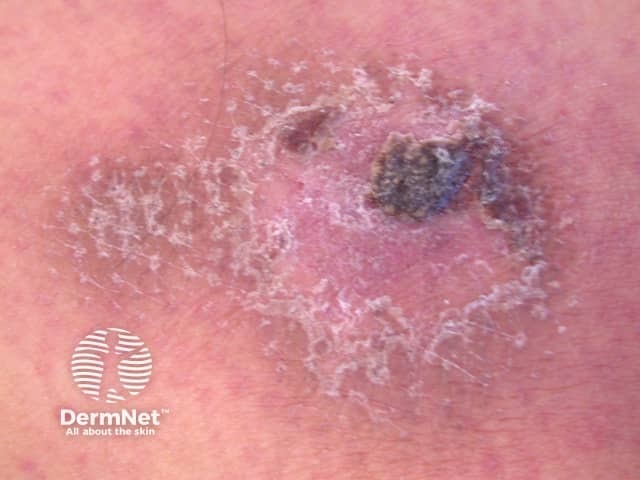
Cytophagic histiocytic panniculitis
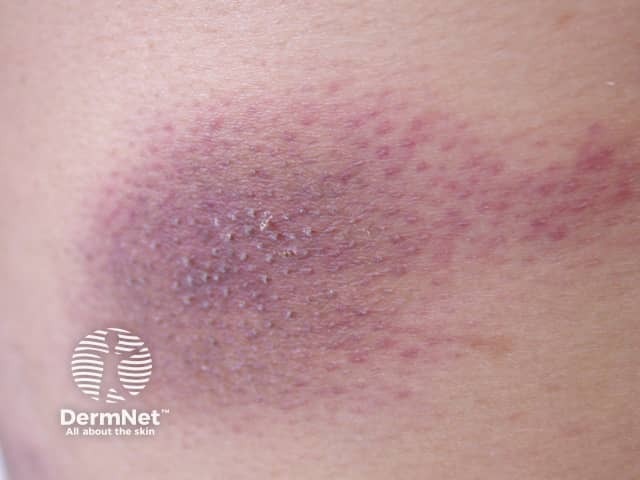
Cytophagic histiocytic panniculitis presents with painful subcutaneous nodules at multiple sites and systemic symptoms.
Death, when it occurs, is associated with bleeding from the gastrointestinal, urinary and respiratory tracts and into the skin.
Cytophagic histiocytic panniculitis is triggered by an infection in about 50% of cases. This is usually one of the herpes viruses. The disease occurs in patients with altered immune function due to immunodeficiency, an autoimmune disease, or haematological disease.
Subcutaneous T-cell lymphoma can also present with cytophagic histiocytic panniculitis.
Biopsy of a subcutaneous nodule shows cytophagic histiocytes and inflammatory cells associated with breakdown and haemorrhage in subcutaneous fat. Abnormal lymphocytes may lead to a diagnosis of T-cell lymphoma.
Further investigations may show damage to other organs and a bleeding tendency. There may be evidence of a preceding infection, such as a herpesvirus, and of altered immune function. If T-cell lymphoma is diagnosed, staging may find evidence of lymphoma in the lymph nodes and elsewhere.
Cytophagic histiocytic panniculitis is usually lethal if untreated.
Symptomatic treatment consists of transfusion and corticosteroid therapy. Etoposide and ciclosporin have been reported to be helpful in some cases. Some authors recommend that cytophagic histiocytic panniculitis should be treated with CHOP-like polychemotherapy. Good results have been obtained with high dose intravenous immunoglobulin.