What is dermatomyositis?
Dermatomyositis is an autoimmune connective tissue disorder involving the skin and the skeletal muscles. Rarely, dermatomyositis may be caused by medications.
Drug-induced dermatomyositis is also known as drug-induced dermopathy, pseudodermatomyositis, and dermatomyositis-like eruption.
Dermatomyositis
Who gets drug-induced dermatomyositis?
Drug-induced dermatomyositis can affect individuals of any race, age, or sex. Drug-induced dermatomyositis is equally common in males and females. There are very few case reports of drug-induced juvenile dermatomyositis.
What causes drug-induced dermatomyositis?
The most common cause of drug-induced dermatomyositis is hydroxyurea, associated with 50% of cases reported in the medical literature, and affecting up to 4% of patients taking hydroxyurea. Hydroxyurea has been typically been prescribed for 4-5 years for chronic myeloproliferative disorders.
Many other drugs have been reported to trigger drug-induced dermatomyositis. The list includes the following among many others:
- Penicillamine
- Lipid-lowering agents including statins and HMF-CoA reductase inhibitors
- Cyclophosphamide
- Non-steroidal anti-inflammatory drugs
- Anticonvulsants
- Bacillus Calmette-Guérin (BCG) administration and other immunisations.
What are the clinical features of drug-induced dermatomyositis?
Drug-induced dermatomyositis can present with:
- Classic dermatomyositis
- Amyopathic dermatomyositis (the cutaneous features without muscle damage)
- Myalgia without cutaneous findings
- Elevated creatine kinase without cutaneous findings or obvious muscle disease.
The classic cutaneous findings of dermatomyositis include:
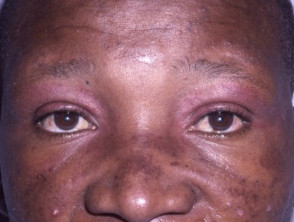
- Heliotrope rash — purple or violaceous eyelids
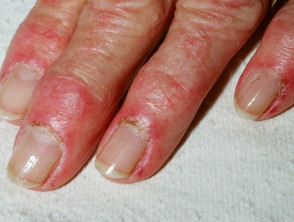
- Gottron papules — purple or violaceous papules or plaques on knuckles or other regions of bony prominence
- Nailfold telangiectasia
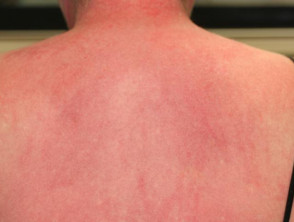
- Photosensitivity and macular violaceous erythema — red or bluish-purple patches on sun-exposed areas.
The majority of cases of drug-induced dermatomyositis present with the pathognomonic heliotrope rash and/or Gottron papules of dermatomyositis, with the remainder having skin changes consistent with dermatomyositis, such as nailfold telangiectasia or photosensitive poikiloderma.
Hydroxyurea-induced dermatomyositis typically presents after longterm treatment (2-10 years) with hydroxyurea with skin changes over the backs of the fingers, hands, and periorbital areas of the face. Often other skin side effects of hydroxyurea are also present. Myositis rarely, if ever, occurs.
In contrast, where drug-induced dermatomyositis is not associated with hydroxyurea symptoms and signs develop soon after starting the offending drug (< 2months), and the majority have myositis as well as skin signs.
What are the complications of drug-induced dermatomyositis?
Complications of dermatomyositis include calcinosis and Raynaud phenomenon, but have not been reported in drug-induced cases.
Dermatomyositis can be associated with adenocarcinoma, a finding not seen in drug-induced dermatomyositis. The majority of malignancies found in patients with drug-induced dermatomyositis are pre-existing haematological disorders, and for most are the reason for the use of the implicated drug.
How is drug-induced dermatomyositis diagnosed?
It may be difficult to distinguish classic dermatomyositis and dermatomyositis induced by drugs. A history of longterm hydroxyurea use or the recent commencement of a new drug should raise the possibility of a drug cause. Confirmation is obtained when the clinical symptoms and signs improve following cessation of the implicated drug.
Serology is usually negative for ANA, anti-Ro, and anti-Jo-1 antibodies. Muscle and skin biopsies shows the same changes as seen in dermatomyositis so cannot be used as distinguishing features.
Skin biopsy shows an interface dermatitis with vacuolar basal cell change, dyskeratotic keratinocytes, and hyper- or hypo-granuloasis.
What is the differential diagnosis for drug-induced dermatomyositis?
The differential diagnosis for drug-induced dermatomyositis includes:
- Statin myopathy — muscle toxicity caused by statins
- Fluoroquinolone-induced tendinopathy — inflammation of weight-bearing tendons caused by fluoroquinolones
- Inclusion body myositis — an idiopathic inflammatory muscular disorder, characterised by progressive muscle weakness, inflammation, and atrophy
- Necrotising myopathy — an idiopathic inflammatory muscle disorder in which there is death of muscle cells.
These differential diagnoses present with symptoms suggestive of myositis but lack the cutaneous findings of dermatomyositis-like eruption.
What is the treatment for drug-induced dermatomyositis?
Cessation of the implicated drug is usually required, although it may be continued if symptoms and signs are mild. In most cases symptoms will improve following discontinuation of the drug. If dermatomyositis remains active for more than one month after the drug ceased, topical or systemic corticosteroids and/or anti-rheumatic drugs may be added if required.
Physical therapy and activity to maintain muscle and joint mobility are also important.
What is the outcome for drug-induced dermatomyositis?
After stopping the drug, patients with drug-induced dermatomyositis generally experience improvement. Complete resolution of the skin signs has been documented in half the patients, usually within the first two months after drug cessation. By 12 months, the majority had cleared. Numbers and time course were similar for resolution or improvement of the myositis.
Clinical features of hydroxyurea-induced dermatomyositis may resolve quickly within days, or can take years to settle after ceasing the drug. Skin atrophy may persist.