Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Updated by Dr Karen Koch, Consultant Dermatologist, Donald Gordon Medical Clinic, University of the Witwatersrand, Johannesburg, South Africa. March 2018. Minor update by Ian Coulson, Dermatologist. Copy edited by Gus Mitchell. July 2024.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Prevention
Outlook
Hand dermatitis is a common acute or chronic eczematous disorder that affects the dorsal and palmar aspects of the hands due to a variety of causes.
Hand dermatitis is also known as hand eczema.
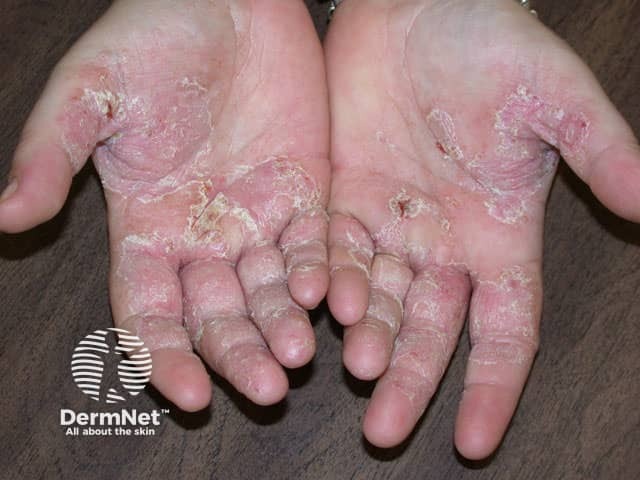
Palmar dermatitis
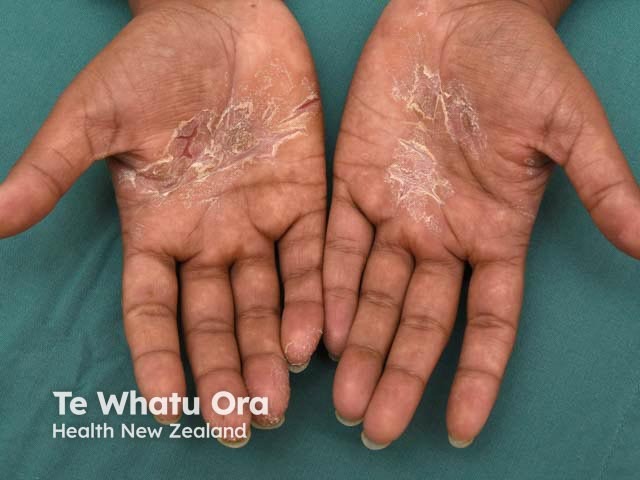
Hyperkeratotic palmar eczema
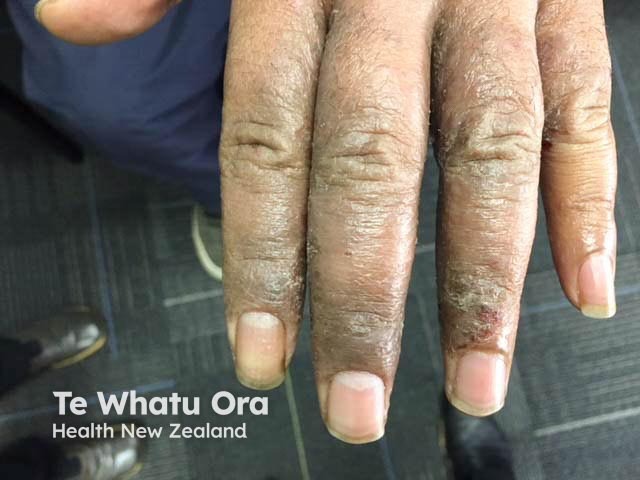
Thickening, dryness, and scale on the dorsal fingers
See more images of hand dermatitis.
Hand dermatitis is common, especially in young adult females, and accounts for 20–35% of all forms of dermatitis. It may occur at any age, including during childhood. It is particularly prevalent in people with a history of atopic dermatitis. [see also Atopic hand dermatitis]
Chronic hand dermatitis is estimated to affect 10–15% of the population and is a common cause of time lost from work.
Hand dermatitis is particularly common in industries involving wet work or exposure to chemicals such as cleaning, catering, metalwork, hairdressing, healthcare, housework, construction, painting and mechanical work. This is mainly due to contact with irritants, but specific contact allergies can contribute [2].
Hand dermatitis often results from a combination of causes, including:
Hand dermatitis is frequently caused or aggravated by work when it is known as occupational dermatitis.
Irritants include water, detergents, solvents, acids, alkalis, cold, heat, friction, and desiccating dusts. These can damage the outer stratum corneum, removing lipids and disturbing the skin’s barrier function. Water loss and inflammation lead to further impairment of barrier function.
In atopic dermatitis, a deficiency in or defective function of the filaggrin protein in the stratum corneum leads to barrier dysfunction resulting in water loss and easy penetration by irritants and allergens [3].
Contact allergy is a delayed hypersensitivity reaction with elicitation and memory phases involving T lymphocytes and release of cytokines [2].
Hand dermatitis may affect the backs of the hands, the palms, or both. It can be very itchy, often with a burning sensation, and is sometimes painful. It has acute, relapsing, and chronic phases.
Acute hand dermatitis presents with:
Features of chronic hand dermatitis include:
There are various causes and clinical presentations of hand dermatitis.
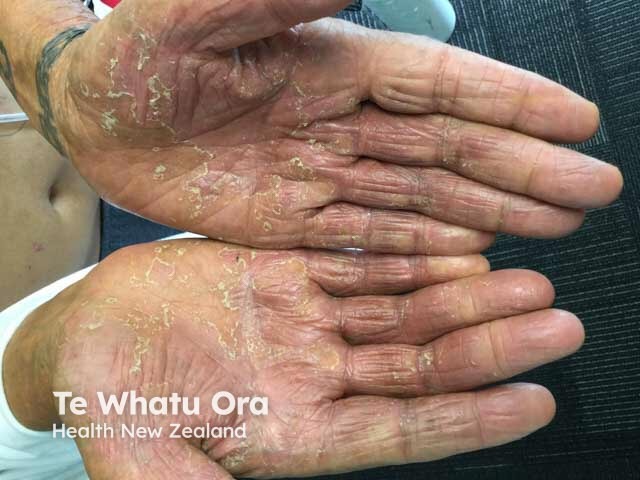
Diffuse scale and redness on the palms due to eczema
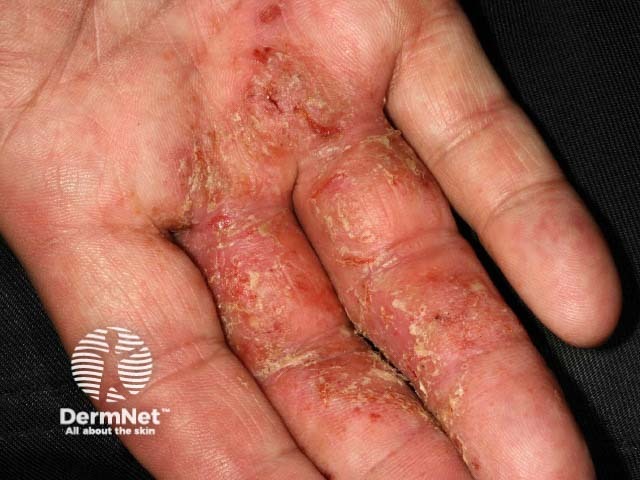
Infected hand dermatitis
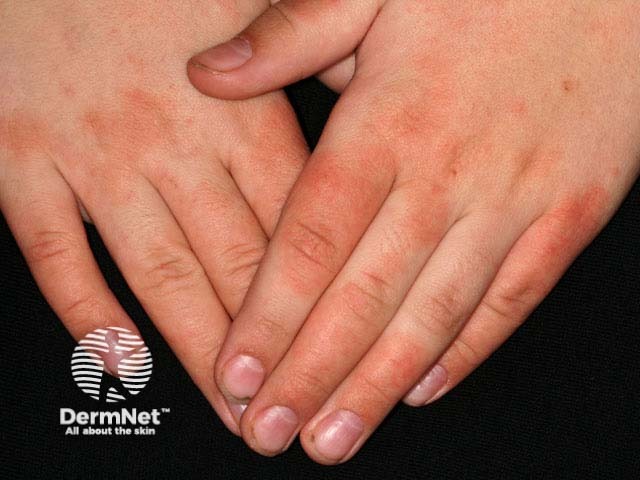
Hand dermatitis on the dorsal fingers in an atopic boy
Atopic hand dermatitis is due to impaired skin barrier function and is triggered by contact with irritants. It usually involves the backs of the hands and around the wrists. It may manifest as a discoid or vesicular pattern of eczema. Patients will typically have signs of atopic dermatitis elsewhere such as in the flexures.
Discoid eczema (nummular dermatitis) tends to affect the dorsal surfaces of the hands and fingers as circumscribed plaques. Other sites of the body may or may not be affected.
Vesicular hand dermatitis is also known as pompholyx. Intensely itchy crops of skin-coloured blisters arise on the palms and the sides of the hands and fingers. Similar symptoms often affect the feet. It is likely this form of dermatitis is exacerbated by excessive sweating (hyperhidrosis) such as in hot and/or humid weather and with emotional stress.
Chronic relapsing vesiculosquamous dermatitis is a common pattern of palmar and finger dermatitis, in which episodes of acute vesicular dermatitis are followed by chronic scaling and fissuring.
Hyperkeratotic hand dermatitis is a chronic, dry, non-inflammatory palmar dermatitis. It can appear similar to palmar psoriasis but is less red and less well circumscribed.
Fingertip dermatitis can be isolated to one or several fingers.
The hands are the most common site for irritant contact dermatitis and are often due to wet work and repeated exposure to low-grade irritants. The finger-webs are the first place to be affected, but inflammation can extend to fingers, the backs of the hands and the wrists. Irritant contact dermatitis often spares the palms.
Allergic contact dermatitis may be difficult to distinguish from constitutional forms of hand dermatitis and irritant contact dermatitis. There are about 30 common allergens and innumerable uncommon or rare ones that may affect the hands. Common allergens include nickel, fragrances, rubber accelerators and chromate (in gloves), and p-phenylenediamine (permanent hair-dye). Clues to contact allergy depend on the allergen, but may include:
Hand dermatitis is usually straightforward to diagnose and classify by history and examination, considering:
However determining the cause of a hand dermatitis can be complicated as it may be multifactorial.
Patients with chronic hand dermatitis may require patch tests to detect contact allergens.
A punch biopsy and skin scrapings (mycology) may be necessary to exclude other causes of inflammation of the hands.

Applying patch tests to the back
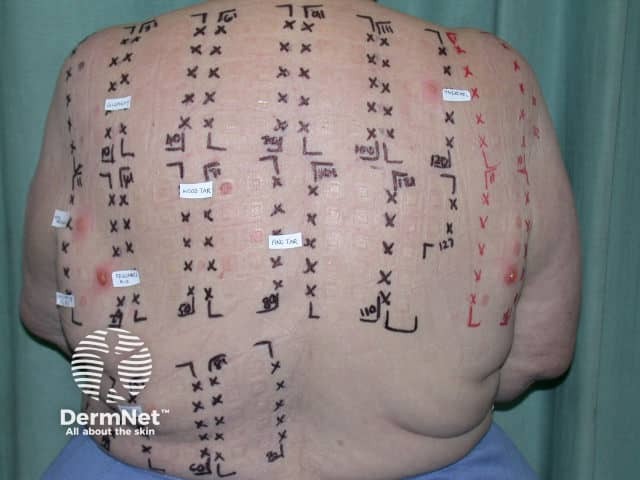
Reading the patch tests - there are several positives

Positive patch test reaction
Patients with all forms of hand dermatitis should be most particular to:
Vinyl gloves are less likely than rubber gloves to cause allergic reactions.
Topical steroids reduce inflammation.
Calcineurin inhibitors (tacrolimus and pimecrolimus) have some evidence to show efficacy in hand eczema and can be used as a steroid-sparing agent [4].
Oral alitretinoin and topical delgocitinib (pan-JAK inhibitor) have been approved for recalcitrant hand dermatitis in some countries. A trial comparing the two showed that topical delgocitinib was more effective and had fewer side effects.
Secondary bacterial infection may require an oral antibiotic, usually flucloxacillin.
Severe acute flares of hand dermatitis are treated with short course oral prednisone (systemic steroids) for 2–4 weeks.
Chronic intractable hand dermatitis may be treated with second-line agents such as azathioprine, methotrexate, ciclosporin, alitretinoin or phototherapy.
Contact irritant hand dermatitis can be prevented by careful protective measures and active treatment. It is very important that people with atopic dermatitis are aware of the risk of hand dermatitis, particularly when considering an occupation.
With careful management, hand dermatitis usually recovers completely. A few days off work may be helpful. When occupational dermatitis is severe, it may not be possible to work for weeks or months. Occasionally a change of occupation is necessary.