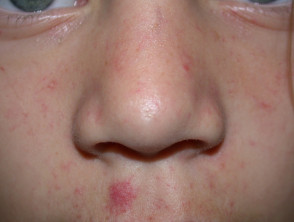
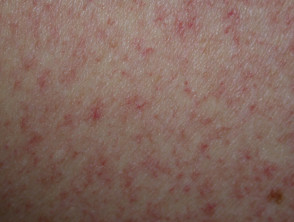
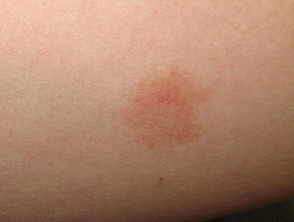
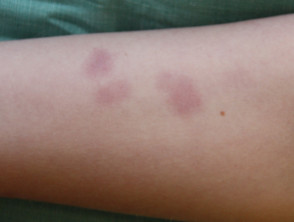
What is telangiectasia?
The term telangiectasia refers to a skin condition composed of fine red blood vessels: these are called telangiectases.
Cutaneous telangiectases are caused by permanent dilatation of small blood vessels resulting in small, red linear markings in the skin and mucous membranes. They can be primary or secondary.
- Primary telangiectases are caused by idiopathic capillary dilatation (unknown cause).
- Secondary telangiectases occur as a feature of a cutaneous or systemic disease process.
What is benign hereditary telangiectasia?
Benign hereditary telangiectasia is a primary telangiectatic disorder. It has varying clinical patterns.
What causes benign hereditary telangiectasia and who is at risk?
The precise cause of benign hereditary telangiectasia is unknown.
- It is inherited in an autosomal dominant pattern. This means it is passed on from one parent to roughly half of their children, therefore multiple family members may be affected.
- Telangiectases tend to appear in the first years of life, often between the ages of 2 and 12 years. They are rarely present at birth.
- Telangiectases are often more noticed by women, but the disorder is not thought to be more common in women.
- The telangiectases may also become more prominent during pregnancy.
- They are often distributed on light-exposed sites, implying sunlight may play a role.
What are the clinical features of benign hereditary telangiectasia?
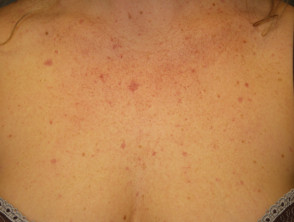
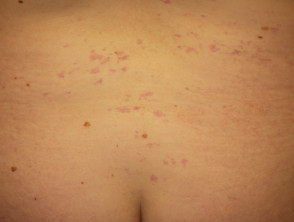
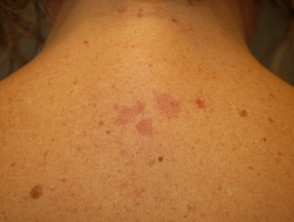
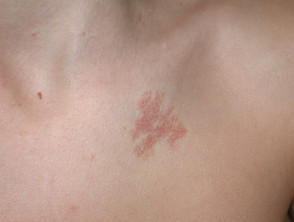
Individuals with benign hereditary telangiectasia tend to present with numerous telangiectases.
- They are often widely distributed over the face, neck, upper trunk, dorsal, hands and, less frequently, knees.
- The telangiectases may be macular, plaque-like, arborising, reticulated, punctate, mottled, spiderlike and linear.
- Punctate telangiectases may be surrounded by pale halos (steal phenomenon).
- Some lesions may be indistinguishable from spider telangiectasis.
- Early telangiectases can be small and erythematous. They often increase in size and may become paler with age.
- The mucosal membranes are not affected with the exception of the vermilion border of the lips.
- There is no systemic involvement or bleeding, in contrast to hereditary haemorrhagic telangiectasia.
- The telangiectases are invariably asymptomatic and cause only mild cosmetic concern.
Benign hereditary telangiectasia
How is benign hereditary telangiectasia diagnosed?
Benign hereditary telangiectasia is a clinical diagnosis. Histological examination of lesional skin shows dilatation of the sub-papillary venous plexus with associated upper dermal atrophy.
What are the differential diagnoses for telangiectasias?
The most important condition to rule out is hereditary haemorrhagic telangiectasia (Osler-Rendu-Weber syndrome). The differential diagnoses of primary telangiectasias in children also include:
- Spider telangiectasis
- Ataxia-telangiectasia
- Generalised essential telangiectasia
- Unilateral nevoid telangiectasia
- Angioma serpiginosum
- Capillary vascular malformations
What is the treatment and outcome of benign hereditary telangiectasia?
Due to the lack of systemic involvement, benign hereditary telangiectasia has an excellent prognosis and medical intervention is not usually required.
When treatment is requested for cosmetic reasons, the following treatments may be considered.