Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction Associated abnormalities Causes Diagnosis Treatment
Hypomelanosis of Ito is part of a rare genetic neurocutaneous syndrome. It is characterised by:
Hypomelanosis of Ito is also known as ‘incontinentia pigmenti achromians’.
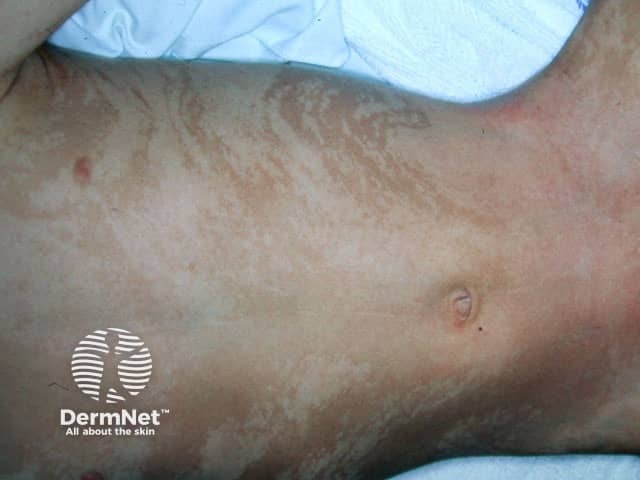
Hypomelanosis of Ito
Associated abnormalities are thought to occur in 30-50% of patients with cutaneous lesions. These include:
Hypomelanosis of Ito is believed to be due to chromosomal mosaicism and sporadic mutations. It is not an inherited disorder as the chromosomal defect occurs after conception. The specific gene(s) is most likely a balanced translocation of Xp21.2.
Hypomelanosis of Ito is present at birth and is usually picked up by a dermatologist, paediatrician or neurologist during the first or second years of life. Thorough history taking and physical examination with attention to neurological and ophthalmological findings are necessary to detect associated abnormalities.
Although recent research has estimated that 30-50% of patients with hypomelanosis of Ito have associated abnormalities, some studies report rates of associated neurological abnormalities as high as 75-94%.
The cutaneous effects of hypomelanosis of Ito do not require treatment. In many cases, the skin may develop pigment over time and blend in well with normal skin. Patients that are conscious of their appearance can use cosmetic camouflage.
Associated abnormalities require appropriate medical treatment.