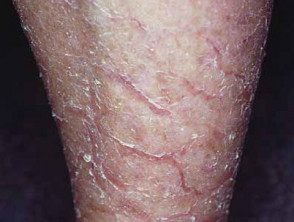
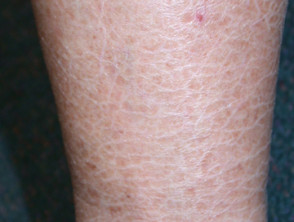
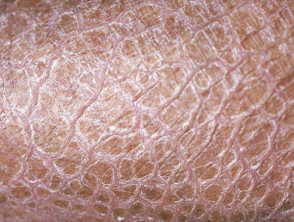
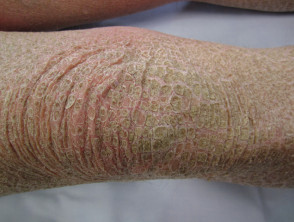
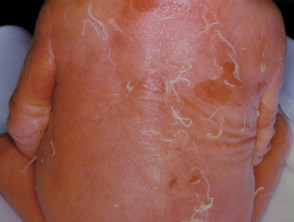
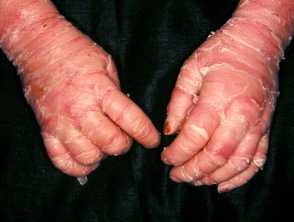
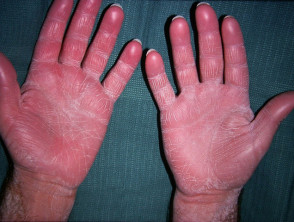
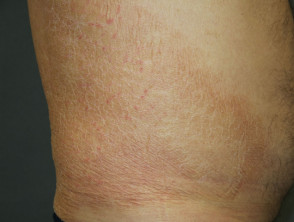
What is ichthyosis?
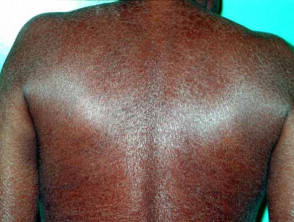
Ichthyosis is a disorder of cornification, characterised by persistently dry, thickened, 'fish scale' skin. There are at least 20 varieties of ichthyosis, including inherited and acquired forms.
Who gets ichthyosis?
Inherited forms of ichthyosis
Inherited types of ichthyosis may be congenital or have delayed onset.
- Ichthyosis vulgaris (1:250—1000) has an autosomal dominant inheritance, meaning an abnormal gene is inherited from a parent. Penetrance is 90%. Onset is delayed until at least three months of age.
- Recessive X-linked ichthyosis (1:2000—6000) mainly affects males, who have a single X chromosome with the abnormal gene. Females are protected by usually having a normal second X chromosome. Onset may be congenital or delayed by up to 6 months.
- In autosomal recessive congenital ichthyosis (1:3–500,000) one abnormal gene is inherited from each parent.
- Keratinopathic ichthyoses (1:200,000) have recessive and dominant forms and present at birth with a collodion membrane.
Ichthyosis can also be due to a new spontaneous mutation.
Acquired ichthyosis
Acquired ichthyosis appears in adult life. People with ichthyosis may have a systemic disease, such as:
- Hodgkin lymphoma
- Underactive thyroid
- Sarcoidosis
- Cancer (ichthyosis may be a cutaneous marker of internal malignancy)
- HIV infection.
Ichthyosis may be provoked by certain medications:
- Nicotinic acid
- Kava
- Targeted cancer therapy (eg, vemurafenib, EGFR and protein kinase inhibitors)
- Hydroxyurea.
What causes ichthyosis?
The inherited forms of ichthyosis occur as a result of genetic mutations that alter the appearance and behaviour of keratinocytes (skin cells) in the stratum corneum (the outer skin barrier layer). Studies have shown that there are inflammatory cells and cytokines in the Th17 pathway that contribute to symptoms and signs.
The cause of acquired ichthyosis is unknown.
How are inherited ichthyoses classified?
Names and classification of ichthyoses are evolving with a greater understanding of the molecular causes of the diseases [1]. The mutated genes are shown in italics.
Common ichthyoses
The common ichthyoses are:
- Ichthyosis vulgaris (95% of all ichthyosis cases) FLG (filaggrin is a structural protein)
- Recessive X-linked ichthyosis STS.
Autosomal recessive congenital ichthyosis
- Harlequin ichthyosis ABCA12.
- Lamellar ichthyosis TGM1 (transglutaminase 1 is an enzyme) and others.
- Congenital ichthyosiform erythroderma ALOXE3 and others.
Keratinopathic ichthyoses
This group has keratin mutations. The main types of keratinopathic ichthyoses are:
- Epidermolytic ichthyosis* KRT1, KRT10
- Superficial epidermolytic ichthyosis¶ KRT2
- Ichthyosis Curth-Macklin§ KRT1
- Congenital reticular ichthyosiform erythroderma.
* Previously called epidermolytic hyperkeratosis or bullous ichthyosiform erythroderma
¶ Previously called ichthyosis bullosa Siemens
§ Previously called ichthyosis hystrix
There are many other rare types of ichthyosis with defined gene abnormalities and clinical features.
What are the clinical features of ichthyosis?
Ichthyosis varies in appearance and severity depending on the cause and the effect of modifying genes.
Ichthyosis vulgaris
- The skin may appear normal at birth.
- By the age of 5, the skin is dry with fine white scale.
- Affects abdomen, arms and legs, sparing creases of arms and legs.
- Causes keratosis pilaris.
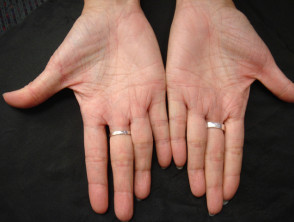
- Palms are excessively lined.
- Associated with atopic eczema in 50%.
Recessive X-linked ichthyosis
- Generalised fine or rhomboid grey/brown scale is present at or within six months of birth.
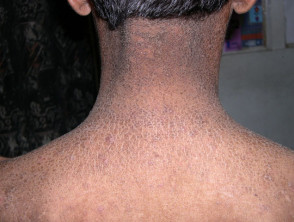
- Scaling is most prominent over the extremities, neck, trunk, and buttocks.
- Palms are normal.
- Corneal opacities in 50%.
- Only affects males.
- Undescended testicles in 5–20%.
Autosomal recessive congenital ichthyosis-1 (ARCI1)
- The baby is encased by collodion membrane at birth, which cracks and is then shed; 10% are self-healing.
- Harlequin ichthyosis: severe collodion membrane, ectropion (drooping lower eyelids), eclabium (out-turned lips) and contractures.
- Lamellar ichthyosis: plate-like dark scaling over the whole body, including creases of arms and legs.
- Bathing suit variant: localised to scalp and trunk (warmer sites of the body).
- Nonbullous congenital ichthyosiform erythroderma (NCIE): erythroderma and fine white, superficial, semiadherent scales.
- Palmoplantar keratoderma varies with affected gene.
Keratinopathic ichthyoses
- Skin is moist, red, and tender at birth.
- Fluid-filled blisters may occur which may become infected and give rise to a foul skin odour.
- Thick, generalised white to brown scaling occurs within a few weeks especially over extensor joints.
- Epidermolytic ichthyosis may cause slowly extending annular polycyclic erythematous plaques.
- Porcupine or spiky appearance in ichthyosis Curth-Macklin, due to a varied thickness of scale.
- KT-1 mutation causes palmoplantar keratoderma (KRT-10 does not).
- Growth failure may occur.
- Mosaic form causes epidermal naevus.
Acquired ichthyosis
- Resembles ichthyosis vulgaris but develops in adult life.
- May have an underlying disease.
- The patient may be taking a drug known to cause dry skin.
Ichthyosis
See more images of ichthyosis.
Ichthyosis syndromes
Ichthyosis is a component of several rare congenital syndromes. These include:
- KID GJB2, GJB6 (keratitis, ichthyosis, and deafness)
- CHIME PIGL (colobomas of the eye, heart defects, ichthyosis, intellectual disability, and ear defects)
- Netherton syndrome SPINK5 (ichthyosis, erythroderma, hair shaft defects, atopic features)
- Sjögren-Larsson ALDH3A2 (ichthyosis, spastic diplegia, pigmentary retinopathy, and intellectual disability)
- Refsum disease PHYH/PEX7 (ichthyosis and pigmentary retinopathy).
How is ichthyosis diagnosed?
Ichthyosis is usually a clinical diagnosis. Genetic testing is available in some centres and prenatal testing may be available for X-linked ichthyosis.
Recessive X-linked ichthyosis is confirmed by absent steroid sulphatase in fibroblasts and elevated plasma cholesterol sulfate levels.
Biopsy reveals:
- Thick, hyperkeratotic stratum corneum
- Reduced or absent granular cell layer and filaggrin in ichthyosis vulgaris
- Lamellar body ‘ghosts’ in lamellar ichthyosis
- Vacuolar degeneration of suprabasal keratinocytes and coarse keratohyalin granules in a thickened granular layer in keratinopathic ichthyosis.
What problems does ichthyosis cause?
People who have very severe ichthyosis may need to spend several hours each day caring for their skin. The problems they encounter may include:
- Overheating: ichthyosis may affect normal temperature control by reducing the ability to sweat
- Limited movement: dry, scaly skin may make it too painful to move some parts of the body
- Secondary bacterial infection: cracking and splitting of the skin may lead to a skin infection and sometimes to systemic infection
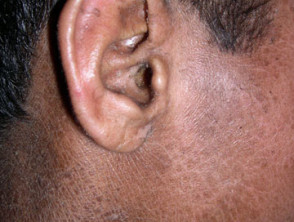
- Impaired hearing or eyesight: skin may build up over the ears or eyes.
What is the treatment for ichthyosis?
There is no cure for the inherited forms of ichthyosis. The following may be useful:
- Non-soap cleansers (soap may exacerbate dryness)
- Bathing in salt water
- Rubbing with a pumice stone or exfoliating sponge to remove scale
- Moisturising creams containing urea, salicylic acid or alpha hydroxy acids. These are best applied to damp skin.
- In severe disease, the oral retinoids acitretin and isotretinoin
- Oral antibiotics for secondary bacterial infection
- Vitamin D supplementation for patients with severe forms of ichthyosis.
Studies are on-going to evaluate the effect of monoclonal antibodies targeting the Th17 immune pathways.
What is the outlook for ichthyosis?
The most severe forms of ichthyosis may threaten the life of an affected newborn, but most people with ichthyosis have a normal lifespan.
Inherited forms of ichthyosis persist lifelong.
Acquired ichthyosis may resolve if the underlying cause can be effectively treated or a causative drug discontinued.