Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Catriona Wootton, Consultant Dermatologist, Nottingham University Hospitals NHS Trust, Nottingham, Nottinghamshire, UK. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. April 2019. Updated November 2019.
Introduction
Introduction
Demographics
Spread
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Prevention
Outcome
Melioidosis and glanders are infectious diseases with similar clinical presentations, both caused by species of the bacterial genus Burkholderia. The two diseases differ in their geographical spread and ecology.
Melioidosis is an uncommon tropical disease caused by the bacterium, Burkholderia pseudomallei (formerly Pseudomonas pseudomallei and Malleomyces pseudomallei). Melioidosis is endemic in South-East Asia and northern Australia, and cases also occur in the South Pacific, Africa, India, the Middle East, and Central and South America. It has the potential to produce fatal disease and is considered a potential biological warfare agent because it is highly infectious, especially by inhalation [1].
Melioidosis is also called Whitmore disease, Vietnamese time bomb, Nightcliff gardener's disease, morphia injector’s septicaemia, and paddy-field disease.
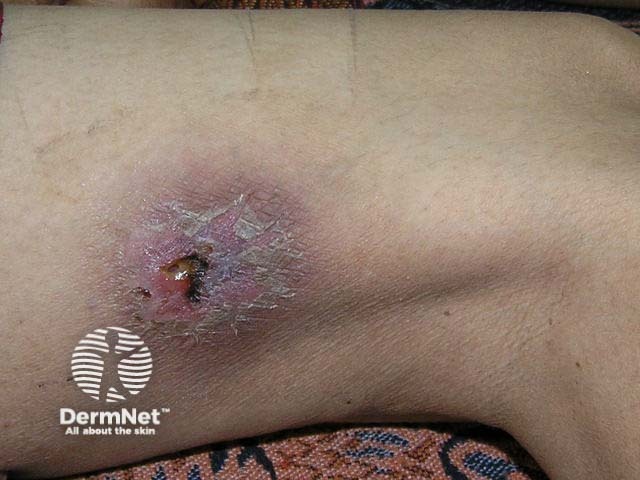
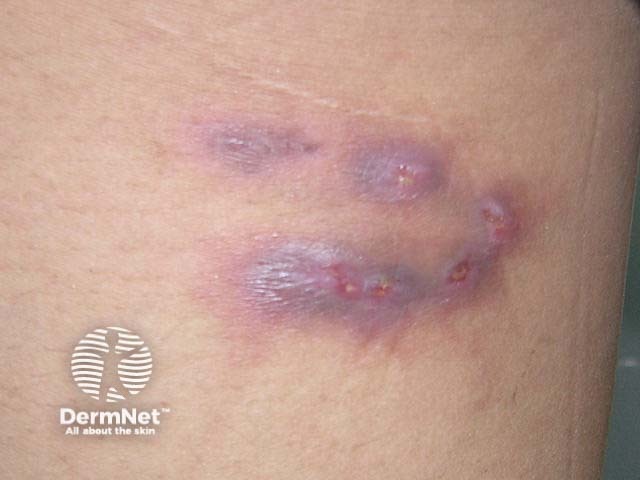
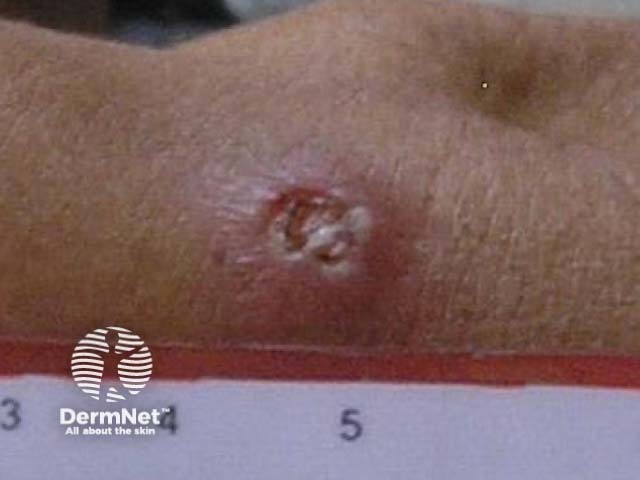
Melioidosis predominantly occurs in people who have frequent contact with soil or surface water, such as workers in rice paddies, particularly during the rainy season. Travellers to rural areas in endemic countries may be at risk if they come into contact with contaminated soil or water, especially if they are immunosuppressed or have a chronic condition such as diabetes, liver or kidney disease, or chronic lung disease [1]. Historically, melioidosis has also been described as being transmitted via intravenous drug use, but this is now extremely rare.
B. pseudomallei can be acquired by humans and animals via contact with contaminated soil (especially through skin abrasions), inhalation of dust, and the ingestion or aspiration of contaminated water. Person-to-person transmission is very rare. The organism is categorised as a Hazard Group 3 biological agent, so specimens from patients with suspected melioidosis must be handled in a containment laboratory to reduce the risk of laboratory-acquired infection.
Most cases of melioidosis in endemic areas are recently acquired (within a few days). However, the incubation period for melioidosis can range up to many years. The disease may develop following surgery, during intercurrent illness, or at times of stress years after exposure, as has been well documented in US servicemen who served in Vietnam [2]. The different presentations of the disease are discussed below.
In healthy people, exposure to B. pseudomallei may be associated with asymptomatic seroconversion (the time period where antibodies develop and become detectable in the blood).
Localised infection with melioidosis results from direct inoculation through a skin abrasion.
Pulmonary infection is the most common presentation for melioidosis.
Septicaemia, or acute bloodstream infection, is the most severe form of melioidosis.
In disseminated melioidosis, abscesses develop in various body sites, such as the skin, lymph nodes, muscle, brain, or internal organs (especially the liver, spleen, lung, and prostate).
Melioidosis can be life-threatening. The risk is increased with:
Complications of melioidosis include:
Culture from blood, sputum, or other infected sites will confirm the diagnosis.
Any infectious disease causing fever, headache, muscle pain with pneumonia, abscesses, or skin involvement could be included in the differential diagnoses for melioidosis, including:
Antibiotics are the mainstay of treatment for melioidosis. Currently, ceftazidime is the treatment of choice during the acute phase.
There is currently no effective vaccine for melioidosis. The risk of exposure to B. pseudomallei can be minimised by:
The septicaemic form of melioidosis carries a very high mortality risk (90%) if not appropriately treated. There is also the potential for the disease to recur in patients many years after the initial infection, including in patients who were asymptomatic originally.
Scarring may occur from chronic skin lesions.
Wiersinga WJ, Virk HS, Torres AG, et al. Melioidosis. Nat Rev Dis Primers 2018; 4: 17107. DOI: 10.1038/nrdp.2017.107. PubMed Central