Introduction
Melioidosis and glanders are infectious diseases caused by species of the bacterial genus Burkholderia. These infectious diseases differ in geographical range and ecology.
What is glanders?
Glanders is a rare, sporadic disease caused by the bacterium Burkholderia mallei (this bacterium has been known by a variety of other names, such as Pseudomonas mallei, Actinobacillus mallei, Pfeifferella mallei, Malleomyces mallei, Corynebacterium mallei, Mycobacterium mallei, and Bacillus mallei).
Glanders is primarily a disease of horses, although it may occur in other animals. It is uncommon now that horses are used less frequently for transport, but it is sometimes seen in parts of Africa, Asia, the Middle East, and Central and South America. Infection with B. mallei may occur in people in direct contact with infected animals. The bacteria enter the body through an abrasion on the skin or via the mucosal surfaces of the eyes, nose, and respiratory tract. Cases of person-to-person transmission have rarely been reported. Glanders can prove fatal, and it is considered to be a potential biological warfare agent because it is highly infectious by inhalation.
Glanders is also known as farcy and malleus.
Who gets glanders?
Anyone working closely with infected animals (mostly horses) or tissue from them, especially horses, is at risk of glanders: veterinarians, stable hands, laboratory workers, butchers, and abattoir workers.
How is glanders acquired?
B. mallei is a host-adapted derivative of B. pseudomallei, the cause of melioidosis. B. mallei bacteria are spread to humans and animals via contact with infected horses and other animals through skin abrasions, mucous membranes, or the inhalation of contaminated dust. Person-to-person transmission is rare.
What are the clinical features of glanders?
The incubation period for glanders is around 1–14 days after infection. The clinical presentation will depend upon the mode of entry and it is similar to that of melioidosis. Symptoms common to all forms include fever, sweating, muscle ache, chest pain, and headache.
Localised infection
Localised infection is characterised by cutaneous inflammation with ulceration at the site of entry (a cut or scratch on the skin).
- Lymphangitis (a red streak tracking to nearby lymph nodes) develops, and swollen lymph nodes or abscesses may also occur.
- Infection involving the mucous membranes (the eyes, nose, or respiratory tract) will result in excess mucous production at those sites.
- The nasal septum and palate may be destroyed by the infection.
- Lymph nodes in the neck become enlarged, giving rise to the name glanders (from the French, glandres).
- Fever, malaise, and headache may occur.
- Systemic infection may affect the lungs, spleen, liver, and other tissues.
Pulmonary infection
Glanders can result in pneumonia, lung abscesses, and pleural effusion due to direct inhalation or bloodborne spread.
- Symptoms are coughing, chest pain, and shortness of breath.
- There may be non-specific symptoms such as fever, headache, sweating, and muscle pain.
- Skin abscesses may develop several months after inhalation of the organisms.
- If untreated, the pulmonary infection is likely to progress to septicaemia.
Bloodstream infection (septicaemia)
In septicaemia due to glanders:
- Skin lesions — papules, pustules, blisters, ulcers, and abscesses may occur
- Multiple organ systems can be affected leading to abscesses and organ failure
- Death usually occurs within 10 days.
Chronic infection
Multiple abscesses due to glanders may develop in the liver, spleen, lung, skin, or muscles.
- The symptoms are less severe than those described in acute infection.
- Chronic infection is reported to persist for up to 25 years in some cases.
What are the complications of glanders?
Systemic infection may lead to multiple organ failure and death.
How is glanders diagnosed?
The diagnosis of glanders is confirmed by culture from blood, sputum, or other infected sites.
Be sure to inform the laboratory of the suspected or confirmed diagnosis.
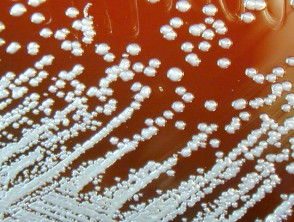
Burkholderia mallei in culture
Credit: PIXNIO.
What is the differential diagnosis for glanders?
The differential diagnoses for glanders includes any infectious disease causing fever, headache, muscle pain with pneumonia, abscesses, or skin involvement. These diseases include:
- Tuberculosis
- Staphylococcal disease with sepsis
- Invasive Klebsiella infection
- Anthrax
- Tularaemia
- Cat scratch disease
- Melioidosis
- Plague.
What is the treatment for glanders?
As it is a bacterial infection, antibiotics are the mainstay of treatment for glanders. As the infection is rare in humans, there are currently no evidence-based treatment guidelines, but a similar treatment approach to that recommended for melioidosis should be adopted.
Prevention of glanders
No vaccine is currently available for glanders. Prevention involves identifying and eradicating infecting animals in endemic areas and appropriate use of personal protective equipment in the healthcare setting and those dealing with potentially infected animals.
What is the outcome of glanders?
Glanders carried a high fatality rate in the pre-antibiotic era, but there have been few human cases since the introduction of antibiotics. It is expected that the outcomes for glanders would be similar to those seen in melioidosis.