Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: February, 2024
Author: Dr Ha Eun Grace Kim, Advanced Trainee in General Medicine, North Shore Hospital, New Zealand (2024)
Previous contributors: Vanessa Ngan, Staff Writer (2005)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Otitis externa, also called external otitis or ‘swimmer’s ear’, is a common inflammatory condition of the external auditory canal (the ear canal). It is characterised by redness, swelling, scaling, and thickening of the ear canal skin lining; and varying degrees of discomfort, itch, ear discharge, and hearing loss.

A weepy otitis externa

An eczematous otitis externa

An eczematous otitis externa - the patient had also extensive scalp seborrhoeic dermatitis
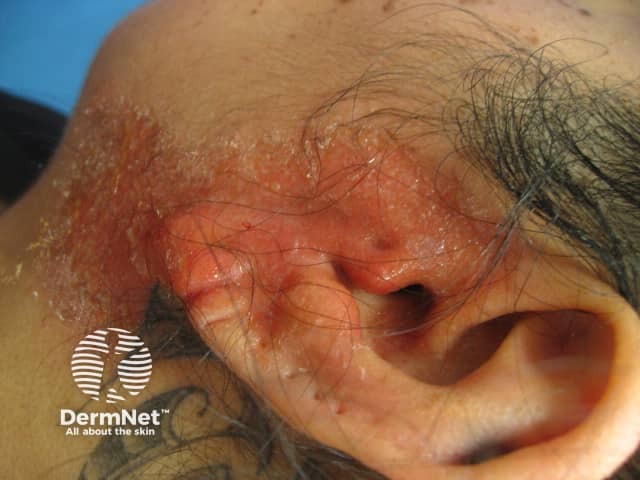
An otitis externa due to allergy to an aural medicament
It is estimated that 10% of people will develop otitis externa in their lifetime.
Otitis externa can occur in all age groups but peaks in children aged 5–9 years old. There is no gender predominance.
Incidence is highest during the summer months. This is thought to be related to increased water exposure such as recreational water activities; and warm, humid environments. Swimming is a key risk factor.
Other risk factors include:
Causes can be divided into infectious or non-infectious. Bacterial infections are the most common cause of otitis externa. Primary skin conditions are often precipitants of infectious otitis externa, but they can also be the sole cause of otitis externa.
The external auditory canal has normal bacterial flora but usually remains free from infection due to protective mechanisms such as intact skin, hair follicles, and cerumen (ear wax). The breakdown of these protective barriers leads to damage to the epithelial lining of the ear canal, and changes to its pH and the quality and amount of cerumen. This in turn leads to bacterial overgrowth.
Common causes that encourage bacterial overgrowth in the external ear include:
The most common bacteria involved in otitis externa are Pseudomonas aeruginosa (41%) and Staphylococcus aureus (15%). Up to 10% of cases of infectious otitis externa are caused by fungal infections with Aspergillus (most common) or Candida. Mixed bacterial and fungal infections can also occur.
Otitis externa caused by other dermatological conditions is often referred to as ‘eczematous otitis externa’. Potential non-infectious causes include:
Due to disruption of the skin barrier, often these conditions can become complicated by superimposed infection.
The most common symptoms of otitis externa are otalgia (ear pain or discomfort) and otorrhoea (discharge from the ear canal). The severity of symptoms can range from mild to severe.
The clinical features of otitis externa may vary according to the cause:
Erythema of the skin may not be apparent in skin of colour. Inflammation in darker skin types may instead appear violaceous or darker than the surrounding skin.
The diagnosis of otitis externa is based on history and physical examination.
Gram staining and culture of the discharge should be considered in those with severe, recurrent, or chronic otitis externa; or in those who are immunocompromised.
Other conditions that could present with similar clinical features of otitis externa include:
Considerations when deciding on specific treatment include a suspected infectious cause, the severity of the otitis externa, any immunodeficiency, and an intact or non-intact tympanic membrane.
Common topical treatments include:
Topical drops that have a combination of antibiotics and steroids may help to reduce inflammation and resolve symptoms more quickly. Drops are usually administered 3–4 times a day for 5–7 days but depend on the product used and clinical presentation. More severe infections may require 10–14 days of treatment.
Topical aminoglycosides, acetic acid solutions, and polymyxins are contraindicated in those with a non-intact tympanic membrane, due to reports of ototoxicity.
In those with marked swelling of the ear canal, an ear wick moistened with antibiotic drops may be placed in the ear canal to help reduce swelling and improve the delivery of ear drops.
Oral antimicrobials are generally not indicated unless there is evidence of extension of the infection beyond the ear canal, immunocompromise, or suspected malignant otitis externa.
Other measures may include:
Those with an acute episode of infectious otitis externa treated with antibiotic/steroid ear drops tend to notice resolution in symptoms within 7–10 days. While further episodes may occur, recurrence risk is not known.
Chronic infection, usually associated with an underlying skin condition, can lead to other complications including (rarely) conductive hearing loss.