Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2013. Updated by A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, January 2018. DermNet Update July 2021
Introduction Demographics Causes Diagnosis Differential diagnoses Treatment Outcome
Sebaceous carcinoma is a rare aggressive skin cancer arising from a sebaceous gland. Sebaceous carcinoma is sometimes called sebaceous gland adenocarcinoma.
Periocular sebaceous carcinoma affects adults. It occurs more frequently in Asian populations than Caucasians and is more common in women than in men, particularly those around 60 to 80 years of age.
Extraocular sebaceous carcinomas occur mainly in older adults and without predilection for male or female.
Patients with Muir-Torre syndrome (a predisposing genetic syndrome) may be diagnosed at a younger age.
Sebaceous glands are small glands connected to hair follicles in the skin. They are located in any hair-bearing region of the body but are most numerous on the skin of the scalp and face. The glands are responsible for producing sebum which is an oily substance that keeps hair and skin moisturised.
The exact cause of sebaceous carcinoma is unclear. The following have been reported to possibly increase the risk of these tumours:
What are the clinical features of sebaceous carcinoma?
Sebaceous carcinoma most commonly develops from the meibomian glands of the eye which are located mostly in the upper but also in the lower eyelids.
Extraocular sebaceous carcinoma accounts for about 25% of sebaceous carcinomas. These tumours mostly occur around the head and the neck. Other sites where these tumours have been found include the genitals, ear canal, breasts, trunk, and oral cavity.
The clinical presentation of extraocular lesions is as a non-specific tumour; they typically appear as a pink to a yellow-red nodule of varying sizes.
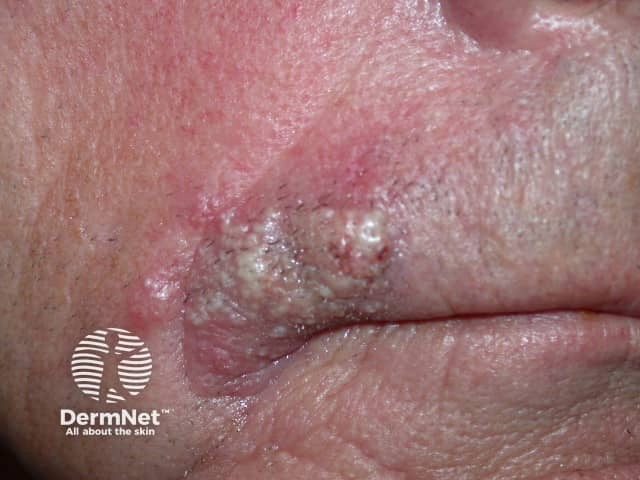
Sebaceous carcinoma
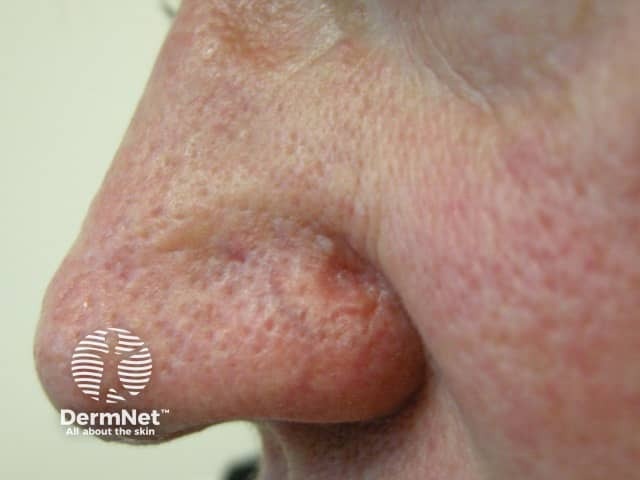
Sebaceous carcinoma
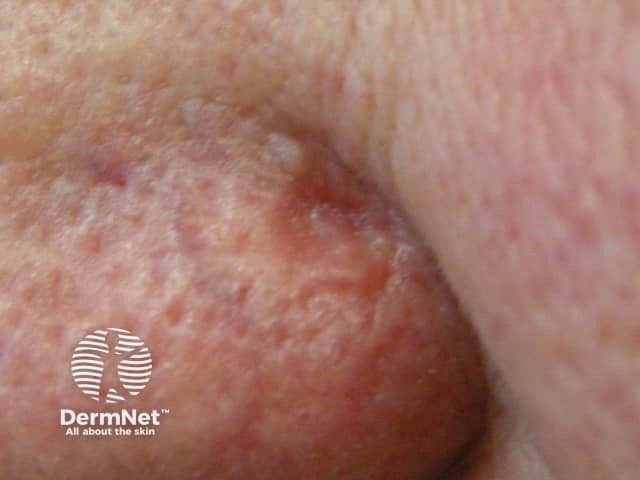
Sebaceous carcinoma
Sebaceous carcinoma may be suspected clinically. Dermoscopy may reveal typical irregular yellowish lobules and irregular linear blood vessels.
Definitive diagnosis is based upon patient history, adequate surgical biopsy and the combined knowledge of a pathologist, ophthalmologist and dermatologist. [see Sebaceous carcinoma pathology]
Immunohistochemistry stains are routinely used to determine the likelihood of Muir-Torre syndrome.
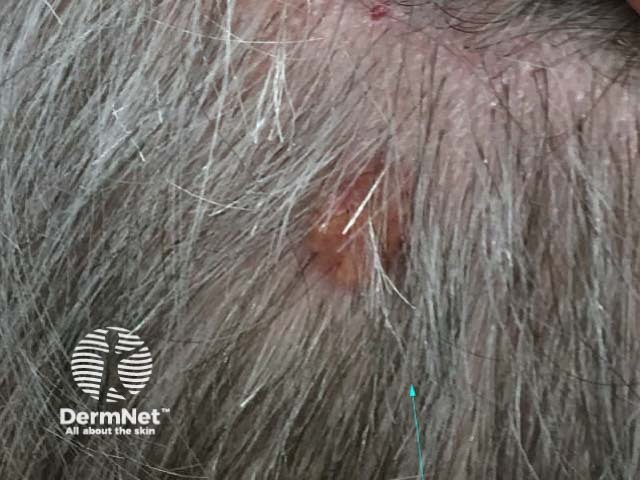
Clinical view
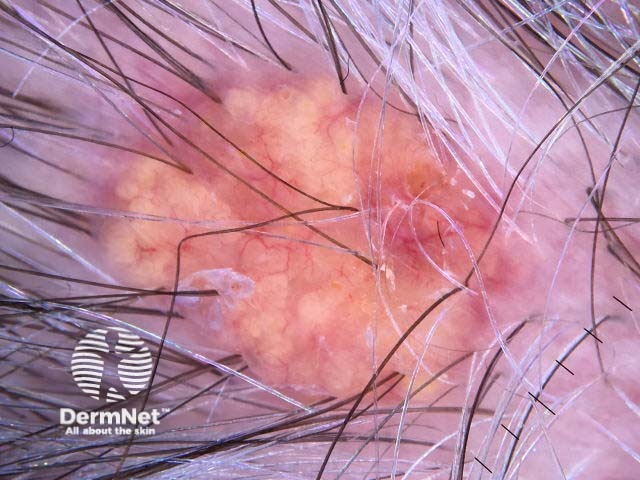
Dermoscopy view
What are the complications of sebaceous carcinoma?
Radical surgical excision with frozen section control by either a standard method or Mohs micrographic surgery is the most common and effective method of treatment.
Radiation therapy should only be used in patients unable or unwilling to undergo surgery.
Sebaceous carcinoma is an aggressive and potentially dangerous tumour that can lead to significant morbidity and mortality. The overall mortality rate is 5–10% because of inherent tumour factors, or delayed diagnosis and treatment.
Factors for a poorer prognosis include delay in diagnosis of greater than 6 months, tumour diameter greater than 1 cm, and both upper and lower eyelid involvement.