Introduction
The manufacturing of chemicals has a major impact on important industries such as agriculture, but the nature of this work can take a toll on its workers. According to a European Union Study, around one of four cases of occupational dermatoses is related to chemical exposure. Occupational dermatoses affects approximately 4–11 out of every 1000 workers in the chemical industry.
Why are workers in the chemical industry at risk?
The elevated risk for workers in the chemical industry comes from several important factors:
- Constant exposure to a wide variety of chemicals, including chemicals that are irritants and sensitisers, carcinogens and mutagens
- Uneven safety regulations throughout the global chemical industry
- Lack of compliance with the use of personal protective equipment among some chemical industry workers.
In developed nations, rates of dermatoses have gone down due to increased automation, changes in chemical manufacturing processes, and better education for employers and employees.
Understanding occupational skin disorders
The skin offers a natural defence against pathogens and other potentially harmful substances. However, forces like friction, heat and cold, irritants and allergens can all eventually cause a breach in this natural barrier, leaving it more vulnerable to breakdown and to secondary bacterial skin infections. While occupational skin diseases can affect workers from any sector, some occupations — like work in the chemical industry — put their workers on higher risk.
Occupational skin diseases have an economic impact. The wider economic impact of these disorders largely stems from:
- Loss of occupation due to poor health
- Medical costs
- Missed workdays
- Decreases in job productivity
- The possible necessity of switching occupations.
Skin disorders related to work in the chemical industry
Workers in the chemical industry are at risk for several different kinds of skin diseases.
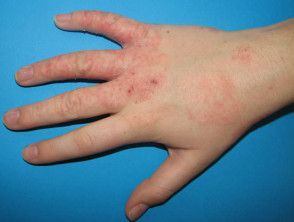
Contact dermatitis
Contact dermatitis is the most common skin complaint among chemical industry workers, who may develop allergic contact dermatitis and/or irritant contact dermatitis.
- In around 80% of cases, the hands are affected; other common sites are wrists, forearms, face, neck and ears.
- Dermatitis may persist long term.
- Acute dermatitis presents with swelling, redness, and blisters, while later, chronic dermatitis is fissured, dry or scaly.
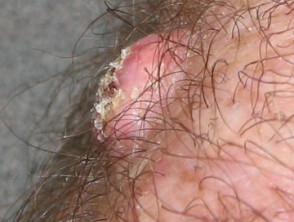
Follicular lesions
- Oil folliculitis stems from exposure to cutting oils and tar products.
- Chlorine-based chemicals such as chloronaphthalene and chlorodiphenyls can also cause chloracne.
- Poor hygiene and lack of compliance with personal protective equipment contribute.
Skin cancer
- Skin lesions can be due to exposure to chemicals like polycyclic hydrocarbons.
- They can be benign or malignant.
- Lesions may not appear until several decades after exposure.
- They are generally diagnosed by biopsy.
Chemical burns
There are high rates of chemical burns in the chemical industry.
-
- Common causes are solvents, acids, alkalis, detergents and oxidising agents.
- The use of gloves and other forms of personal protective equipment can reduce the risk of chemical burns.
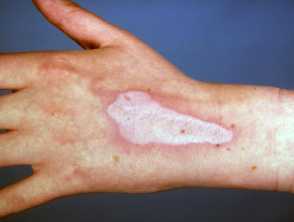
Contact leukoderma
Contact leukoderma or white patches can occur if the skin is in contact with phenolic compounds and are a hazard in industries exposed to these.
Skin disorders in chemical industry workers
Workplace risk assessment
A thorough workplace risk assessment should identify any problems with poor workplace safety.
Workplace safety guidelines should include:
- Knowledge of all work site chemicals and their properties
- Protective or preventative measures
- Methods to eliminate dangerous substances and replace them with less hazardous ones where possible
- The aim of reduced employee chemical exposure through automation or enclosure of processes.
Personal protective equipment
Due to the dangerous nature of chemical work, different kinds of personal protective equipment might be needed in order to keep employees safe, including:
- Gloves
- Goggles or other eye protectors
- Respirator masks
- Chemoprotective clothing and aprons.
Hand care advice for chemical industry workers
Taking care of the hands is important for workers in the chemical industry. They can do this by:
- Choosing the right glove for the right job
- Washing hands with mild soap as needed and drying them thoroughly; using alcohol gel or hand sanitiser where appropriate
- Applying emollients and moisturisers as needed
- Knowing early signs of dermatitis, such as chronic dryness, maceration (moist peeling skin) and redness.
Diagnosis and treatment of occupational hand dermatoses
Diagnosis of an occupational skin disorder should be based on the following:
- Clinical signs and symptoms (the appearance, location and course of lesions)
- The patient’s personal and medical history
- The patient’s occupational history (the nature of the patient’s work, the potential for hazardous exposure, duration of exposure and length of time on the job, and particular job tasks)
- Patch tests if contact allergy is suspected
- Biopsy, if indicated.
Treatment of dermatitis can include:
- Emollients
- Topical corticosteroids
- Short courses of oral prednisone or prednisolone
- Referral to a dermatologist if the symptoms persist or resist first-line treatment.