What is coma?
Coma is a state of prolonged unconsciousness when the patient does not move or respond to a painful stimulus, light, or sound.
Coma usually requires management in an intensive care unit. Causes of coma include head injury, stroke, brain tumour, drugs, alcohol, diabetes mellitus, and infection. Assessment of the skin may provide a diagnostic clue as to the cause of the coma or reflect the patient’s comatose state.
Causes of coma and their possible associated skin signs
Coma can result from a serious fall or accident.
- Bruises, lacerations, or swelling may indicate that the patient has been subjected to a traumatic insult.
- An electrical shock may cause skin signs of an electrical burn, and may be significant enough to cause the patient to fall or be thrown.
Coma can be associated with a wide range of infections.
- Bacterial meningitis
- Purpura fulminans which is commonly preceded by petechiae and acrocyanosis.
- Viral encephalitis
- Nonspecific maculopapular rash may occur.
- Vesicles raise the possibility of severe varicella zoster infection or rarely disseminated herpes zoster infection.
- A tick may suggest tick-borne encephalitis.
- Rickettsial infections
- Maculopapular rash that comes after fever.
- Scrub typhus may be associated with an eschar.
- Cryptococcal infection
- Papules, pustules, nodules, and ulcers.
- Secondary syphilis
- Maculopapular rash on the palms and soles.
- Toxic shock syndrome and other severe skin infections can be associated with septic encephalopathy.
Coma is caused by a variety of toxins.
- Carbon monoxide poisoning
- Mucous membranes and lips may have a cherry red appearance.
- Skin lesions include erythema and blistering with an appearance similar to burns.
- Cholinesterase inhibitor toxicity
- Dry flushed skin.
- Inhaled mercury exposure
- Acrodynia: pink, perspiring, swollen and peeling hands and feet.
- Hypoxic ischaemic encephalopathy
- Pressure injuries indicated prolonged immobility
- Embolic stroke. There are different types of emboli. These may be distinguished by cutaneous findings:
- Cholesterol emboli: includes livedo reticularis and progressive peripheral ischaemia
- Septic emboli: peripheral skin signs include splinter haemorrhages, petechiae, Osler nodes, and Janeway lesions
- Tumour emboli: if there is accompanying embolism to the skin, myxomatous tissue from an atrial myxoma can be revealed on biopsy
- Fat emboli: may be associated with long bone fractures and a characteristic petechial rash; involves the upper body including the sub-conjunctivae.
- Subarachnoid haemorrhage
- Rarely associated with gnathostomiasis with its characteristic facial larva migrans profunda sign.
- Seizures
- Traumatic injury to the tongue or lips.
- Sturge-Weber syndrome is associated with seizure activity.
- Acute intermittent porphyria and systemic lupus erythematosus (SLE) rarely presents with seizures.
Coma can be a manifestation of a systemic disease.
- Hepatic encephalopathy
- Associated with signs of liver disease or chronic alcohol use.
- End stage renal disease
- AV fistulae and calciphylaxis with tender indurated erythematous papules or nodules.
- Myxoedema coma
- Includes skin signs such as pretibial oedema.
- Hypoadrenalism
- Skin signs of adrenal insufficiency.
- Diabetic ketoacidosis
- Dry skin and mucous membranes.
- Cutaneous vasculitic lesions can sometimes be associated with systemic pathology. This includes involvement of the cerebral vessels. Those particularly relevant to coma include:
- Antiphospholipid syndrome
- Variety of skin signs including livedo reticularis and superficial thrombophlebitis.
- Hyperviscosity syndrome
- Mucosal bleeding.
Cutaneous paraneoplastic syndromes
- Variety of skin signs including papulosquamous, erythematous, and bullous pemphigoid lesions.
- In this setting, coma can result from cerebral metastases or other paraneoplastic phenomenon, such as seizures.
Coma can be associated with nutritional deficiencies.
- Vitamin B3 (niacin) deficiency
- Variable skin signs that include hyperkeratosis, hyperpigmentation, and mucosal erythema.
Drug hypersensitivity syndromes
- Initial morbilliform rash, that can progress to widespread desquamation with Stevens Johnson syndrome/toxic epidermal necrolysis.
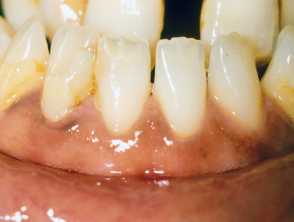
Gingival pigmentation was the clue to underlying Addison disease, presenting as an Addisonian crisis
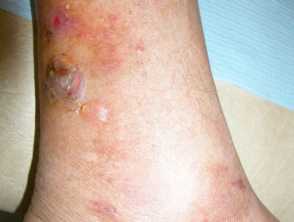
The blisters in this patient are due to bullosis diabeticorum; coma was due to hyperglycaemia
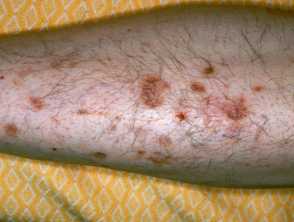
Diabetic shin spots, (diabetic dermopathy) was the clue to diabetes in this comatose patient
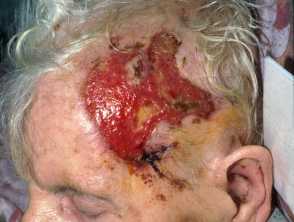
The extending ulcer on this lady's temple was the result of temporal arteritis, which had caused visual loss and ultimately coma
Livedo reticularis was the result of a medium-size-vessel vasculitis; associated cerebral vasculitis resulted in coma
The tick causing tick-borne encephalitis was still attached
Skin signs of coma
What are the skin signs that result from a patient being in a coma?
Pressure ulcers
Pressure ulcers can occur due to immobility, hypotension, malnutrition, use of vasoactive medication, and inability to communicate their ischaemic pain.
Prevention of pressure ulcer includes limiting pressure, friction, and shear, while managing comorbid conditions that may interfere with wound healing, such as diabetes.
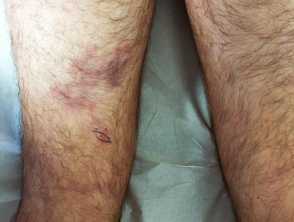
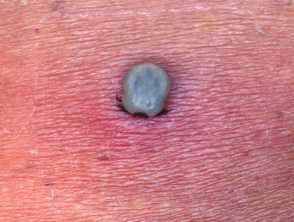
Coma blisters
Coma blisters, multiple, tense, blood-filled blisters appearing at pressure sites, typically occur 2–3 days after the onset of coma and are often self-limiting, resolving after several weeks.
Traditionally associated with barbiturate overdose, coma blisters can develop in association with coma due to other causes (eg, diabetic coma). They are thought to be caused by hypotension-associated necrosis and pressure.
Skin biopsy shows a subepidermal blister and sweat gland and sweat duct necrosis. Thrombi in dermal vessels is often a clue the coma is not drug-induced.
What other skin signs might you see in someone with a coma?
- Skin signs may occur as a result of management of a comatose patient.
- Examples include pressure areas from an endotracheal tube or dermatitis from exposure to adhesive dressings to secure devices.
- Critically ill comatose patients may require high dose vasopressor therapy
- Can be associated with digital ischaemia.
- Cutaneous drug reactions are not uncommon in this population.
- Skin signs may also be incidental, reflecting pre-existing pathology or post-admission development.