Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Gemma Law, Final Year Medical Student at Monash University; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, October 2015.
Introduction Demographics Causes Clinical features Diagnosis Treatment Outcome
Acrocyanosis is a functional peripheral vascular disorder characterised by dusky mottled discolouration, or cyanosis, of the hands, feet, and sometimes the face.
Acrocyanosis is caused by vasospasm of the small vessels of the skin in response to cold. It can be primary or secondary.
Primary acrocyanosis most often presents in adolescents and young adults (onset is often in the 20s–30s).
Secondary acrocyanosis can present at any age, depending on the underlying cause.
Causes of acrocyanosis depend on whether it is primary or secondary.
Primary acrocyanosis is genetically determined or of unknown origin. It is not associated with occlusive arterial disease. Chronic vasospasm of small cutaneous arterioles or venules results in secondary dilatation of capillaries and the sub-papillary venous plexus.
Contributing factors leading to secondary acrocyanosis can include:
Primary acrocyanosis presents with bilateral, symmetrical, painless and persistent blue discolouration of fingers and toes. Acrocyanosis may extend to include hands, feet and face. Pressure on an area of blanching leads to a slow and irregular return of blood from the periphery towards the centre (Crocq sign). Arterial pulses are normal, and there is no proximal pallor, ulceration or gangrene.
Clinical features of acrocyanosis may also include:
The presentation of secondary acrocyanosis varies depending on the underlying cause. Secondary acrocyanosis is often asymmetrical and is associated with pain and tissue damage (blue toe syndrome).
Signs of a primary disorder may be present.
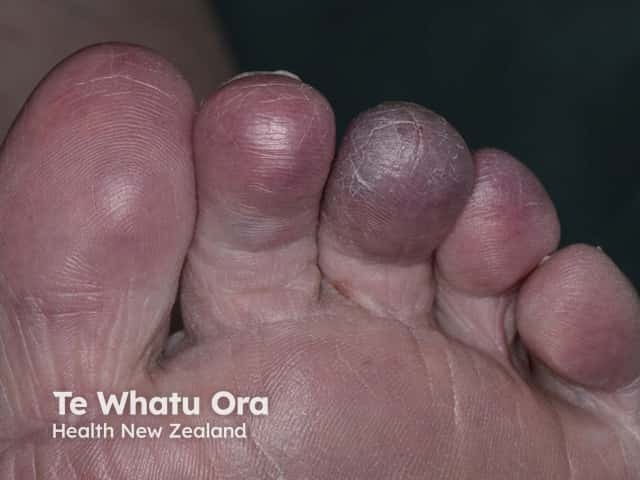
Secondary acrocyanosis
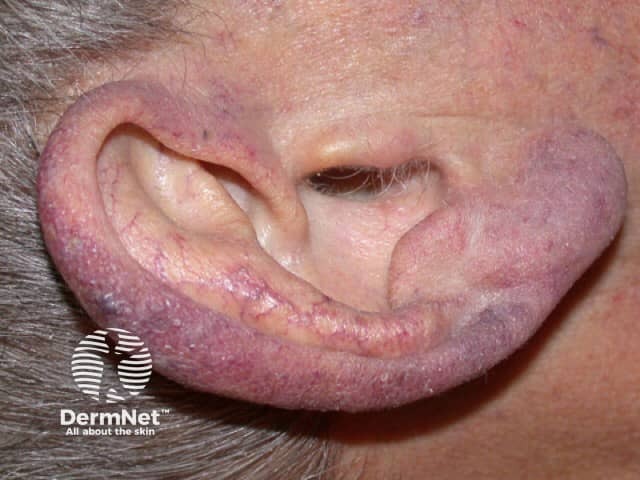
Secondary acrocyanosis
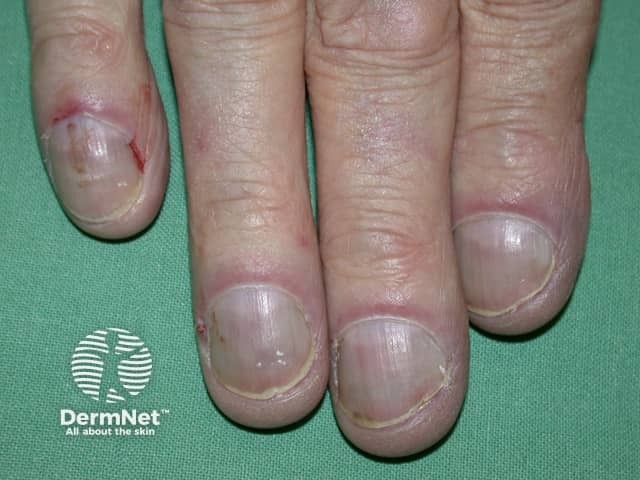
Secondary acrocyanosis
Clinical diagnosis of acrocyanosis is based on the patient's general appearance and the distribution and persistence of cyanosis.
In young adults, where the diagnosis is most likely to be primary acrocyanosis, only limited investigations are required.
In older adults, or if there are atypical features such as pain and asymmetry of acrocyanosis, a targeted history, examination and investigations will be required to determine the cause. Investigations may include:
Treatment is not required for the majority of patients with acrocyanosis and pharmacological intervention is rarely necessary. The patient should be reassured that the condition is harmless. Options for active management may include:
Note that vasodilators, eg calcium channel blockers, are not helpful (unlike in Raynaud phenomenon).
Treatment of secondary acrocyanosis depends on the underlying cause.
Primary acrocyanosis is a benign condition that usually resolves in middle age with no long-term sequelae.
Secondary acrocyanosis may resolve with treatment of primary cause. As the pathological mechanisms that cause secondary acrocyanosis vary, so does prognosis.