Introduction
Streptococci (plural of streptococcus) are bacteria that are commonly found harmlessly living in the human respiratory, gut and genitourinary systems. Several species are capable of causing disease in humans, including skin diseases.
What skin disease is due to streptococcal skin infection?
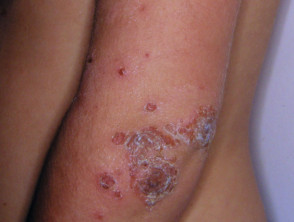
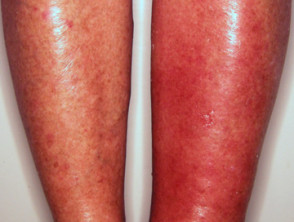
Skin diseases due to direct infection with streptococcus include:
- Impetigo
- Ecthyma
- Cellulitis
- Erysipelas
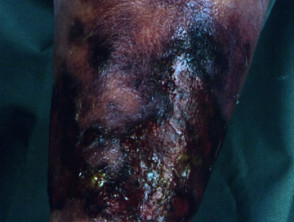
- Necrotising fasciitis
- Secondary skin infection of wounds, dermatitis, scabies, diabetic ulcers etc.
- Tropical ulcers
- Blistering distal dactylitis
- Streptococcal perianal and/or vulval dermatitis.
Streptococcal disease
In addition, streptococci are capable of causing skin disease through means other than direct infection of the skin; for example:
- Scarlet fever is a reaction to a circulating toxin that is produced by some strains of streptococcus
- Streptococcal toxic shock-like syndrome (STSS)
- Allergic hypersensitivity to streptococcal bacteria may result in erythema nodosum or vasculitis
- Psoriasis, especially guttate forms, may be provoked or aggravated by streptococcal infection
- Pustulosis acuta generalisata: scattered sterile pustules on hands, feet and elsewhere following an streptococcal upper respiratory tract infection; may be associated with painful joints.
Bacteriology of streptococci
Streptococci are classified as Gram-positive cocci based on their appearance under a microscope. They are spherical or ovoid in shape and tend to forms chains with each other.
Streptococci that cause human disease are usually facultative anaerobes; that is, they prefer lower levels of oxygen in their environment. Streptococci are further classified into subtypes based on sugar chains expressed on their outer shell (Lancefield group) and their behaviour when grown in the laboratory (alpha- or beta- haemolysis). Most streptococci important in skin infections belong to the Lancefield groups A, C and G, and are beta-haemolytic. Streptococci pneumoniae (pneumococci) are bacteria important in pneumonia and meningitis but rarely cause skin disease. Pneumococci are alpha-haemolytic and do not belong to the Lancefield group.
Lancefield Group A
This group consists of a single type of streptococcus called Streptococcus pyogenes. Up to one-fifth of the healthy population can carry S. pyogenes in the throat. S. pyogenes produces many toxins and enzymes that aid it in establishing infection. It is an important cause of pharyngitis, impetigo, cellulitis and necrotising fasciitis. It is capable of inducing scarlet fever, post-infectious glomerulonephritis (kidney disease) and rheumatic fever (heart disease).
Several of these products produce an antibody response in the patient's blood that aids in detection of recent streptococcal infection (eg, anti-DNAase, anti-streptolysin). These can help in the diagnosis of rheumatic fever, post-streptococcal glomerulonephritis and erythema nodosum.
- The serum ASOT reaches a maximum around three to six weeks after infection and starts to fall in six to eight weeks, returning to baseline after 6–12 months.
- The serum anti-DNase B titre can take up to six to eight weeks to reach a maximum and starts to fall three months after infection, returning to baseline more slowly.
Rapid-result throat swabs are also available but are not absolutely reliable and should be interpreted in the clinical context (remembering that asymptomatic carriage of streptococci in the throat is common).
Lancefield Group C and G
These bacteria occasionally cause infections similar to Lancefield Group A and usually affects am older person or chronically ill patient.
Pneumococci
S pneumoniae bacteria may live in the throat and nose of healthy people. They produce a sticky substance on their outer shell which enables them to attach to the lining of the nose or throat and invade, causing infections in some patients. Most infections involve the respiratory tract or meninges but pneumococci occasionally causes cellulitis. Cellulitis due to pneumococci usually affects patients with connective tissue disease or HIV infection.
Treatment of streptococcal skin infection
It can be difficult to distinguish clinically between skin infection caused by streptococci and other bacteria such as Staphylococcus aureus. Antibiotics should therefore be chosen to cover the most likely organisms. Flucloxacillin is more appropriate than simple penicillin as it treats both Staphylococcus (staph) and strep.
If the laboratory has confirmed streptococcal infection, then the most appropriate antibiotic is usually penicillin. All streptococci in the Lancefield group are very sensitive to penicillin. Those patients with penicillin allergy may be given erythromycin or a cephalosporin (eg, ceftriaxone), which are effective against most streptococci although some erythromycin resistance is emerging. In very severe S. pyogenes infections, such as necrotising fasciitis, clindamycin may be added to penicillin as very large numbers of bacteria may overwhelm penicillin's mechanism of action.
Pneumococcal skin infections are generally treated with penicillin but low levels of resistance have recently been reported. In more serious infections, ceftriaxone or vancomycin may be more appropriate.