Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003. Updated by Dr Jannet Gomez, Postgraduate Student in Clinical Dermatology, Queen Mary University London, United Kingdom, April 2016.
Introduction
Causes
Demographics
Clinical features
Complications
Diagnosis
Treatment
Prevention
Trichomycosis axillaris is a superficial bacterial infection of underarm hair. The disease is characterised by yellow, black or red granular nodules or concretions that stick to the hair shaft. It can also affect pubic hair (when it is called trichomycosis pubis), scrotal hair, and intergluteal hair.
The name is misleading because "trichomycosis" is bacterial in origin rather than a fungal infection.
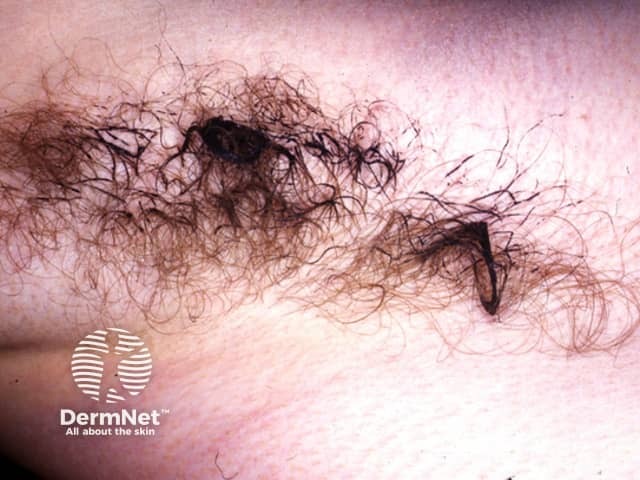
Trichomycosis axillaris
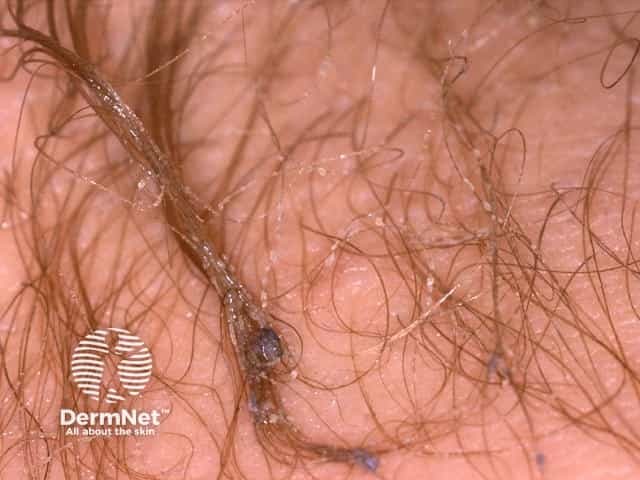
Trichomycosis axillaris
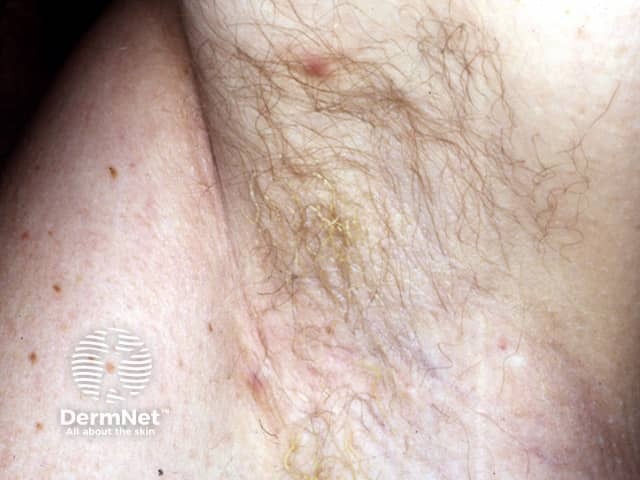
Trichomycosis axillaris
Trichomycosis axillaris is caused by the overgrowth of Corynebacterium (Corynebacterium tenuis, C propinguum, C flavescens) and Serratia marcescens. The concretions consist of tightly packed bacteria. The bacteria proliferate in moist areas of the body, thus mainly affect underarm hairs, and to a lesser extent, pubic hair.
The bacteria cause malodour due to the metabolisation of testosterone in sweat into smelly compounds.
Trichomycosis axillaris occurs in males and females of all races in temperate and tropical climates. It appears to be more common in men than women but this is because many women shave their underarm hair.
Contributing factors include:
Trichomycosis axillaris is symptomless and often ignored. Signs include:
The corynebacterial triad is the occurrence of erythrasma, trichomycosis axillaris, and pitted keratolysis in a single individual.
Trichomycosis axillaris is a benign condition that does not have any complications.
The condition may resemble pubic lice (pediculosis) and Trichosporon aselie infections.
The fastest way to get rid of trichomycosis axillaris is to clip the affected hairs or shave the area
Effective topical antibacterial preparations include clindamycin, erythromycin and fusidic acid. Clotrimazole powder is also curative.
Recurrences of trichomycosis axillaris are prevented by keeping the underarm dry and clean.