Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Claire Jordan Wiggins, Riyad N.H. Seervai, Medical Students, Baylor College of Medicine, Houston, Texas, USA. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. April 2020.
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
A cutaneous angiofibroma is a benign vascular neoplasm composed of dermal fibrous tissue and blood vessels.
Angiofibroma is classified by association with a genetic disorder or according to its body site [1].
Angiofibromas are associated with the following genetic disorders:
Angiofibromas are more commonly acquired.
Tuberous sclerosis is a neurocutaneous autosomal dominant syndrome, in which angiofibromas appear in childhood in the nasolabial folds and on the central face [2]. Patients with tuberous sclerosis commonly develop an oral fibroma or a periungal angiofibroma (Koenen tumour) over time [1]. The facial angiofibromas associated with tuberous sclerosis are also called adenoma sebaceum, juvenile angiofibroma, and Pringle tumour.
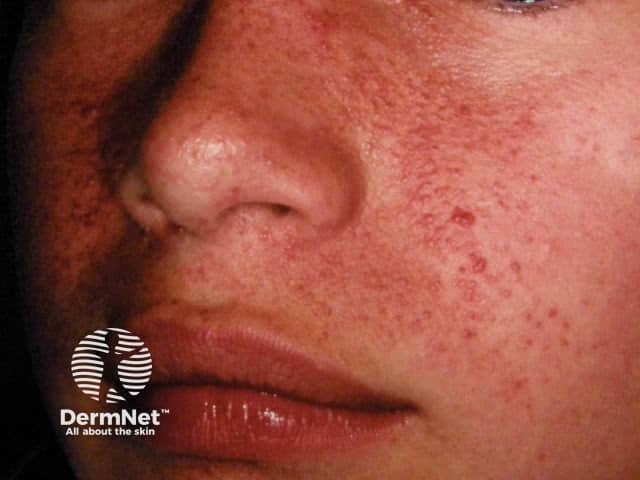
Angiofibromas in tuberous sclerosis
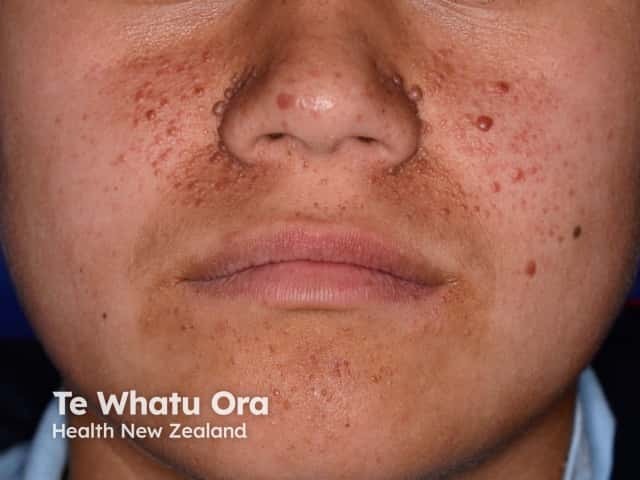
Angiofibromas in tuberous sclerosis
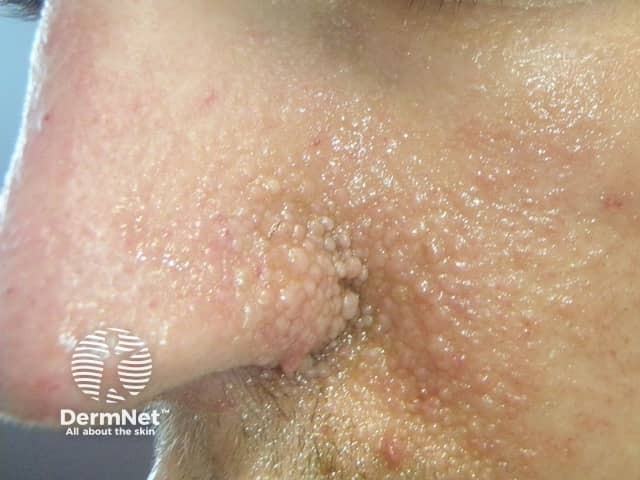
Angiofibromas in tuberous sclerosis
Facial angiofibromas have been reported in Birt-Hogg-Dubé syndrome, a rare genodermatosis characterised by skin and renal tumours, as well as spontaneous pneumothorax [3]. Most of the cutaneous lesions however are fibrofolliculomas, which are abnormal growths of the hair follicles.
Multiple endocrine neoplasia type 1 is a hereditary syndrome that leads to tumours in several endocrine organs [1].
Angiofibromas can also be acquired and unrelated to a genetic syndrome, commonly in the form of:
A fibrous papule is characteristically found in adults as a solitary lesion usually on the nose, often clinically mistaken for a basal cell carcinoma or melanocytic naevus. It is thought to be a form of dermal naevus.
Multiple pearly penile papules occur in 10–30% of adult males on the coronal edge and sulcus. They can be mistaken for viral warts [1,2].
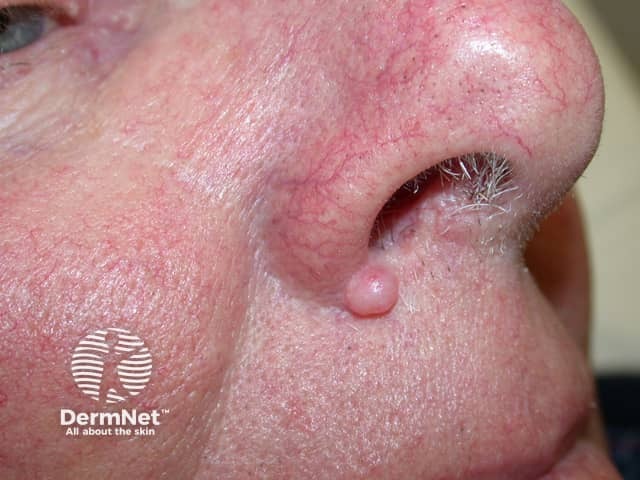
Fibrous papule
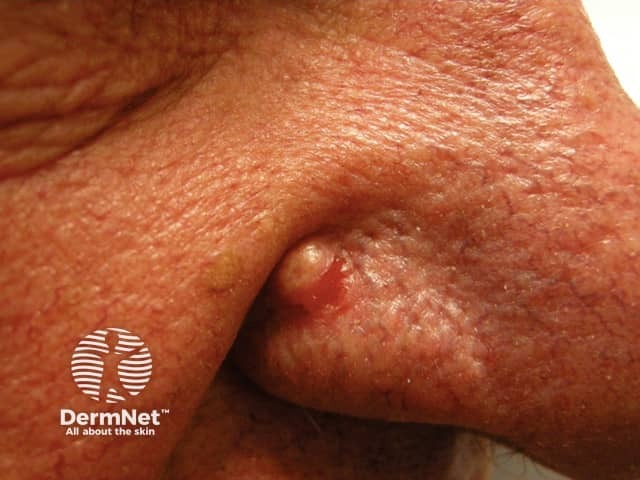
Fibrous papule of the nose
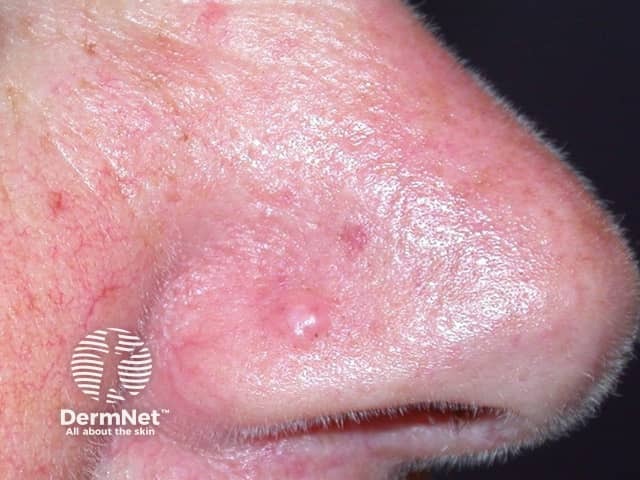
Fibrous papule of the nose
See penile pearly papules images.
Angiofibromas are caused by a local overgrowth of collagen, fibroblasts, and blood vessels.
Genetic mosaicism for these genetic conditions must also be considered [4]. What specifically triggers the development of angiofibroma is unknown.
An angiofibroma is a firm, flesh-coloured dome-shaped papule less than 5 mm in diameter. Small capillaries may be visible on the surface of the lesion.
Angiofibromas may be itchy and may also bleed. Those associated with genetic syndromes result in facial disfigurement and stigmatisation [1]. See Psychosocial factors in dermatology.
The diagnosis of angiofibroma may be made clinically or after a skin biopsy. The histopathology of angiofibroma shows an ‘onion skin’ pattern around vessels and follicles, hyperkeratosis, and vascular proliferation [5].
If an underlying genetic condition is suspected, appropriate genetic screening and evaluation are required [1].
The differential diagnosis for angiofibroma depends on its location [1].
Differential diagnoses for facial lesions that can resemble angiofibromas can include:
Differential diagnoses for periungual lesions that can resemble angiofibroma can include:
Differential diagnoses for penile lesions that can resemble angiofibroma can include:
Angiofibromas are benign and do not always require removal. Options for treatment of angiofibromas include:
Multiple treatments are often necessary [1].
Although angiofibromas are benign, they are persistent. Angiofibromas can be removed for cosmetic or pain-related reasons. The recurrence rate for angiofibromas associated with tuberous sclerosis may be as high as 80% [1].