Introduction and definitions
This page describes vesiculobullous and pustular lesions in newborns and their differentiating characteristics.
- A neonate is a newborn baby under 28 days of age.
- Vesicles are small blisters containing clear fluid.
- Bullae are large blisters containing clear fluid.
- Pustules are circumscribed lesions that contain dense cellular content.
Vesiculobullous and pustular lesions in neonates can be due to miscellaneous benign conditions, an infection, a genodermatosis, or a transient autoimmune bullous disorder.
Fluid-filled skin lesions
Benign disorders causing blisters and pustules in neonates
There are several benign disorders that may present within a few days of birth with blisters and pustules. These include:
- Congenital sucking blisters — blisters and erosions on the forearm, hands, and fingers caused by vigorous sucking by the fetus while in the womb
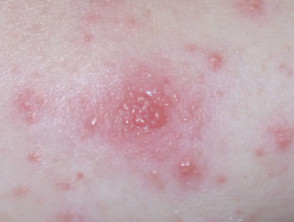
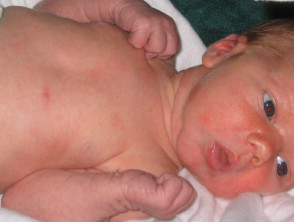
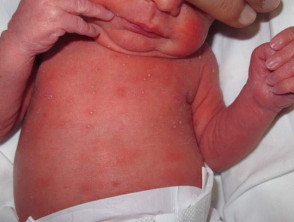
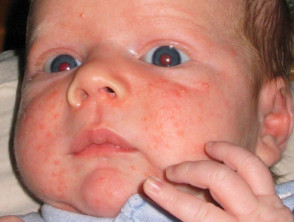
- Erythema toxicum neonatorum — a transient combination of erythematous macules, papules, and pustules on the face, trunk, and limbs
- Transient neonatal pustular melanosis — an uncommon pustular condition may be a variant of erythema toxicum neonatorum
- Neonatal acne — presents with comedones on the scalp, upper chest, and back and inflammatory lesions on the cheeks, chin, and forehead.
Benign neonatal conditions
Neonatal blistering diseases may be due to viral, bacterial, fungal, or parasitic infection.
Viral infection
- Herpes simplex virus (HSV) is the most common viral infection in newborns.
- Varicella zoster virus (VZV) is the cause of chickenpox and shingles.
- Coxsackieviruses and other enteroviruses cause hand, foot, and mouth disease.
- Cytomegalovirus (CMV) is a rare cause of blisters.
The onset of viral infections is within days to weeks after birth.
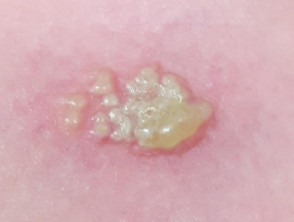
- HSV and VZV present as grouped vesicles on an erythematous base, evolving to pustules and then crusted erosions.
- Localised blisters due to herpes simplex are often found on the face and scalp and sometimes on the trunk and buttocks. Neonates may develop disseminated HSV.
- HSV may be associated with prematurity and low birth weight and can complicate other vesiculopustular disorders.
- Primary varicella infection in neonates (chickenpox) has a high mortality rate of 25%.
Viral infections that cause blisters
Bacterial infection
- Staphylococcus aureus may cause impetigo or staphylococcal scalded skin syndrome (SSSS).
- Streptococcus pyogenes may cause impetigo.
- Pseudomonas aeruginosa may cause abscesses.
- Listeria monocytogenes is the cause of listeriosis.
- Treponema pallidum causes congenital syphilis.
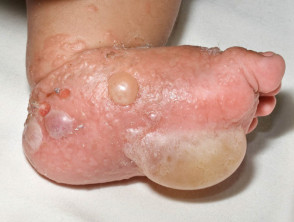
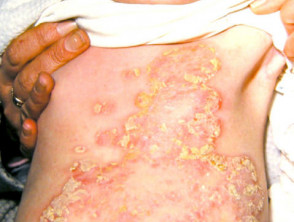
Staphylococcal infection in a neonate usually presents with localised superficial, flaccid, vesiculobullous or pustular lesions that rupture to reveal an erythematous base and then form seropurulent crusts. The infection may extend to cause fever and widespread SSSS [1].
Listeriosis is a cause of premature birth. It presents early with multiple pustules on the mucous membranes and skin and may progress to cause meningitis and septicaemia [1].
Congenital syphilis is associated with generalised haemorrhagic bullae and petechiae.
Staphylococcal infections in newborn babies
Fungal infection
An infection caused by Candida albicans tends to occur a few weeks after birth or in an older baby, often presenting as oral thrush (white sticky plaques on a reddened mucosa) or napkin dermatitis. Candida infections are characterised by very superficial blisters and pustules associated with erythematous papules and plaques in intertriginous sites. Systemic mycosis with disseminated candida can also occur in neonates [1].
Oral Candida albicans infection
Parasitic infection
Scabies is caused by the parasitic mite Sarcoptes scabiei. In a young baby, it causes a widespread vesiculopustular eruption, that is prominent on the palms and soles. The source of the infestation is likely to be a family member or visitor with an itchy rash [1].
Scabies in an infant
Blistering from genodermatoses in neonates
The blistering genodermatoses are:
- Epidermolysis bullosa
- Epidermolytic ichthyosis
- Aplasia cutis congenita
- Incontinentia pigmenti
- Cutaneous mastocytosis
- Congenital forms of porphyria.
Inherited vesiculopustular and bullous genodermatoses are rare. They should be suspected in newborns with a family history of a genodermatosis or consanguinity [2].
- The clinical diagnosis of epidermolysis bullosa may be unreliable due to the variable presentation. Epidermolysis bullosa is associated with generalised skin fragility and blistering after minor trauma and has extracutaneous manifestations [2].
- Epidermolytic ichthyosis is a keratinopathy that presents with widespread blisters and scaling. A localised variant causes an epidermal naevus [1].
- Aplasia cutis congenita is a congenital focal absence of skin, most often an isolated lesion midline of the posterior scalp. It is sometimes associated with other physical defects or disorders [1].
- Incontinentia pigmenti presents along Blaschko lines (eg, as a linear eruption on one limb). It has four stages of development (the vesicular, verrucous, hyperpigmented, and atrophic/hypopigmented stages) that may be present simultaneously; blistering is a feature in 50% of cases [1].
Genodermatoses that can blister
Blistering from transient autoimmune diseases in neonates
Maternal history of an autoimmune blistering disease can lead to a newborn presenting with the same autoimmune bullous disorder. Maternally transmitted autoimmune bullous disorders usually resolve within a few months of birth [1]. These include:
- Pemphigus vulgaris
- Pemphigus foliaceus
- Bullous pemphigoid
- Epidermolysis bullosa acquisita
- Linear immunoglobulin A dermatosis.
What tests should be done in a neonate with blisters?
An initial investigation in a neonate with blisters includes scraping fluid and cells from an intact blister for viral/bacterial/fungal microscopy, culture, and testing for a polymerase chain reaction to specific organisms [1,2].
A skin biopsy, with or without direct immunofluorescence, should be undertaken if the infectious screen is negative and in those patients refractory to an initial therapy [3].
Blood, urine, and cerebrospinal fluid cultures can be used to detect disseminated disease in SSSS and herpes simplex [1].
Genodermatoses can be confirmed by skin biopsy using standard light microscopy, transmission electron microscopy, and immunofluorescence microscopy. Molecular genetic testing should also be considered [2].
An autoimmune blistering disease is investigated by a cord blood sample with serum indirect immunofluorescence on salt-split skin, and autoantibody enzyme-linked immunosorbent assay to desmoglein 1 and 3 and bullous pemphigoid antigen BP180. If there is no history of blistering in the mother, a lesional skin biopsy should be performed for histopathology. A perilesional skin biopsy should be submitted for direct immunofluorescence [2,4].
What is the treatment for blistering in neonates?
The treatment of the blistering disease depends on the diagnosis.
A benign disorder such as neonatal acne, erythema toxicum neonatorum, and transient neonatal pustular melanosis is self-limiting and no specific treatment is required [1].
Bacterial infection should be managed with empirical antibiotics according to each country's guidelines.
The management of epidermolysis bullosa is focused on prevention, wound care, and the optimisation of nutrition [2]. Aplasia cutis congenita is usually managed by conservative wound care.
Most cases of neonatal autoimmune blistering disease are self-limiting, and symptoms may be reduced by the use of topical corticosteroids [3].