Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Sarah Liley, medical student, University of Auckland, Auckland, New Zealand. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy editor: Maria McGivern. April 2017.
Introduction
Demographics
Contraindications
Regulations
Procedures
Side effects and risks
Body piercing is the practice of creating an opening through a part of the human body to allow for adornment with jewels, metals or cultural pieces either for temporary or permanent use.
Like tattooing, body piercing is a form of body modification. Related body piercing techniques include [1]:
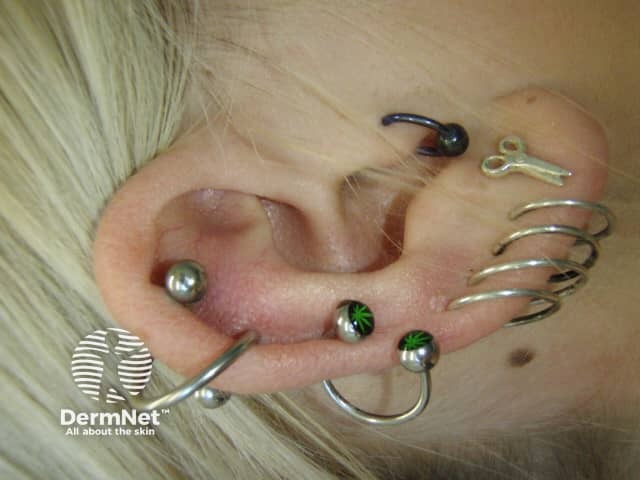
Earrings
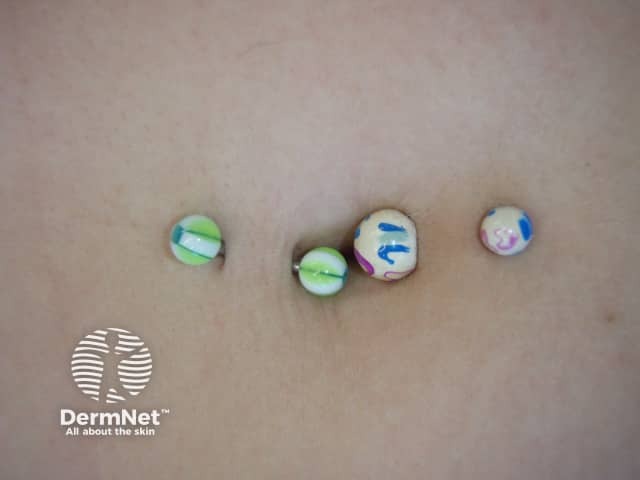
Belly button jewelry
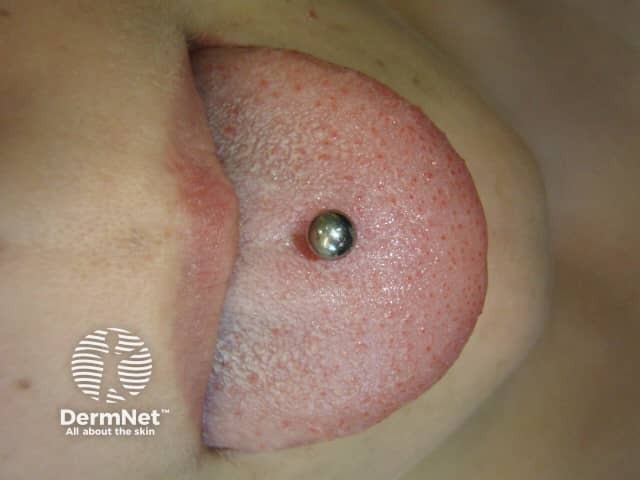
Tongue stud
Body piercing is observed across diverse cultures and has been practised for thousands of years. In Western populations, its prevalence wavers dramatically. Its popularity is determined by the reasons people decided to have a piercing; for example, to feel unique, for aesthetic reasons, eroticism, or conformity, or as a form of rebellion or self-control.
The incidence of body piercing is greatest in young adults and in women. It is correlated with increased risk-taking behaviour and a search for identity [2,3], but not with psychopathology or low self-esteem [4]. Multiple piercings (> 4) and/or intimate piercings, such as of the nipples or genitalia, increases the risk of concurrent high-risk behaviours and emotional distress [5].
Traditional forms and uses of body piercing continue to be practised world-wide, including in religious customs and cultural ceremonies incorporating spiritual beliefs and/or culture-specific symbolism. Traditional therapeutic uses of piercing include scarification and acupuncture-like piercing; for example, left nasal piercing in Ayurvedic medicine is thought to reduce the pain of menstruation and childbirth. Conversely, piercings placed in specific points have been blamed for ill health and infertility.
Maori and Pacific peoples may use bone or other traditional materials for cultural piercing [6]. Piercing techniques, adornments and possible complications from traditional piercing vary considerably. Fundamental in all cases is the importance of infection control measures and, where necessary, respectful, culturally-competent medical management.
Body piercing is also performed surgically to insert a magnetic tongue barbell in individuals with tetraplegia to help with the use of tongue-operated assistive technology [7].
Materials known to cause allergy — including anaphylaxis — must be avoided in the individuals undergoing body piercing, including any sanitary products normally used in the procedure (eg, nickel plated items, latex surgical gloves).
Body piercing is strongly contraindicated in individuals with local infection or inflammatory disease, including:
Body piercing is moderately contraindicated in individuals with the following conditions or circumstances:
Body piercing is widely considered a simple procedure, with potential complications being under-recognised by both providers and their clients [6,13,14]. Commercial body piercing (not including regular ear piercing) is typically done at tattoo studios and non-commercial piercing ‘backyard jobs’ are not uncommon [6,14].
The setting and regulation of industry standards for body piercing, under the overarching domain of public health, is the responsibility of the relevant territorial authorities. The New Zealand Ministry of Health provides Guidelines for the safe piercing of skin [6], which may form the basis of any local standards or serve as a resource for providers and their customers where there are no local governing standards.
In New Zealand, few regulatory standards are described or enforced. Most councils have age restrictions on carrying out body piercing, with interested individuals needing to be either 16 or 18 years of age at minimum. Adolescents may undergo body piercing prior to this age when providers are given written parental consent. With the exception of ear piercing where infants and children (usually girls) may have their ears pierced with parental consent, further body piercing in this age group is not regulated and has not been reported.
Intoxication and peer pressure may independently affect an individual’s decision to undertake the procedure. Individuals interested in undergoing body piercing should educate themselves on the topic and assess the risks; visiting multiple providers (to review sanitation, ask questions and check out reviews) is strongly recommended.
Once the procedure has been performed, the pierced individual should avoid public swimming pools and spas due to the risk of infection. Contact with the piercing site should be avoided aside from cleaning. Cleaning should be once to twice daily with antimicrobial soap and water. Oral piercings should be cleaned with antiseptic, alcohol-free mouthwash. Ice may be used to reduce swelling. Intimate piercings and alternative piercing types require special care.
Healing times vary and are affected by the location of the piercing, individual client factors and aftercare. Any pus, ongoing bleeding, or other concerns should be reviewed by a medical professional.
The lack of regulation and incident reporting (especially regarding sensitive or high-risk piercings), means that estimates of the incidence of adverse effects of body piercing are inconsistent and unreliable [14].
Immediate complications of the body piercing procedure may include:
The following cutaneous adverse effects may occur.
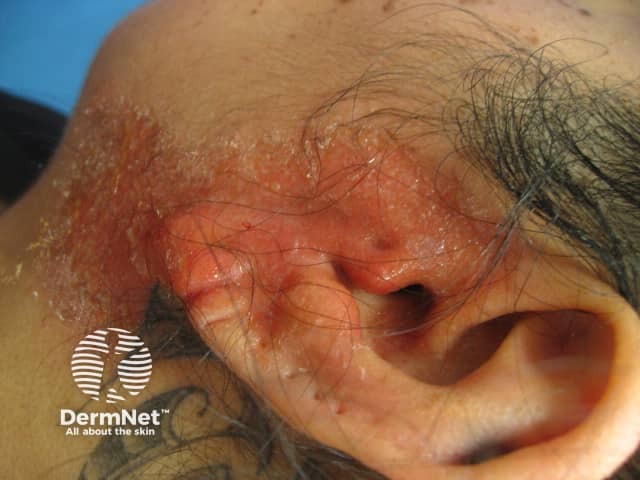
Contact dermatitis to disinfectant
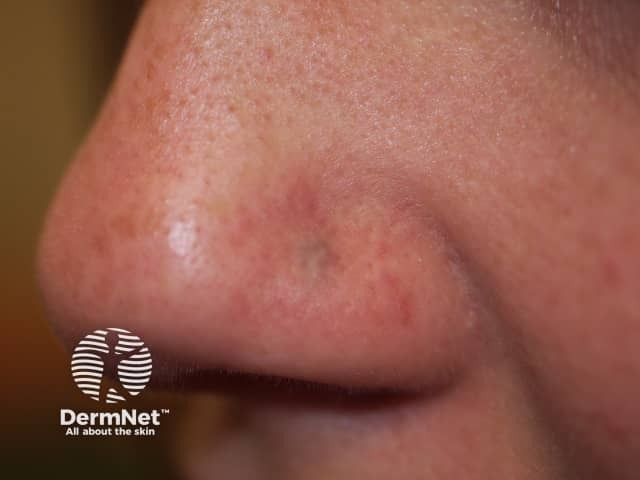
Blue discolouration of piercing scar
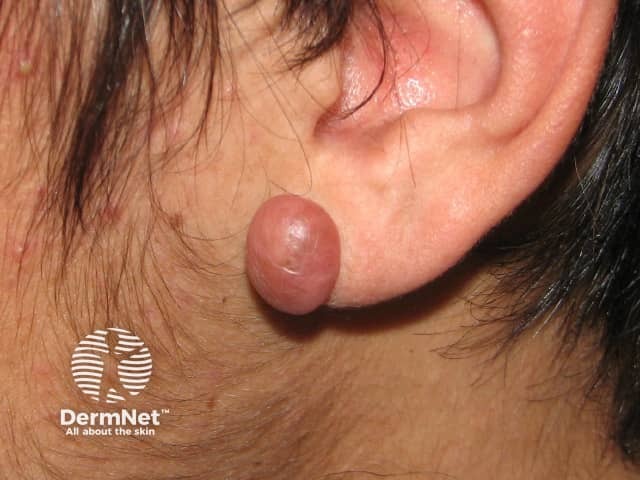
Keloid scar at site of ear piercing
The penetration of the skin barrier with body piercing exposes underlying tissues. With body piercing, wound healing is slow due to the presence of a foreign body (the piercing jewellery), and in cartilaginous piercings, poor blood supply. The risk of infectious complications is greater in deep piercings and those through mucosal surfaces. Oral infections can also swell and occlude the body piercing client’s airway.
The list of potential infectious complications includes:
The most frequently isolated pathogens are Pseudomonas aeruginosa and Staphylococcus aureus. Potential viral infections include hepatitis B, hepatitis C and human immunodeficiency virus (HIV). As a precaution, body piercing clients should not donate blood for 6 months after piercing procedures.
Body piercing can have psychological effects on individuals who undergo the procedure.