Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Karen Koch, Dermatologist, Waikato Hospital, Hamilton, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. June 2019.
Introduction Demographics Causes Clinical features Diagnosis Differential diagnoses Treatment Outcome
Erythema annulare centrifugum is a chronic reactive form of annular erythema characterised by erythematous, circular, arciform, and polycyclic lesions, with a characteristic delicate scale behind the advancing edge (‘trailing scale’).
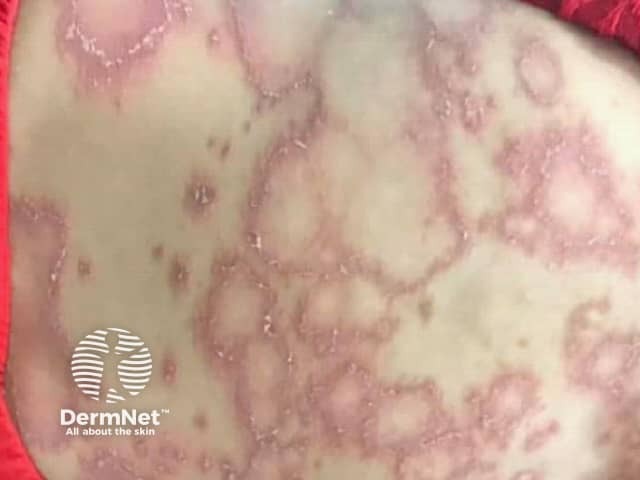
Erythema annulare centrifugum

Annular erythema
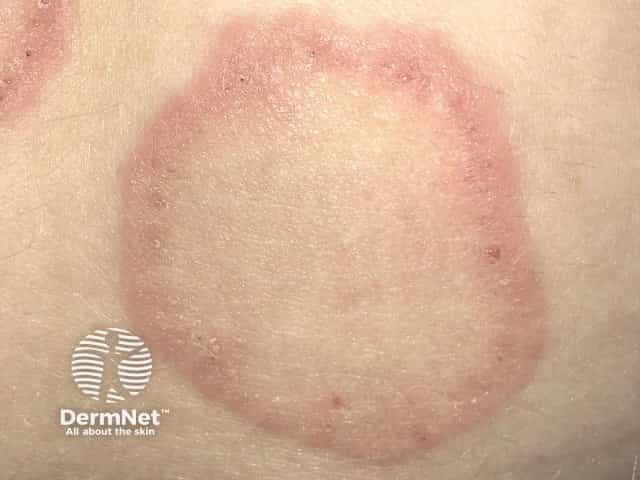
Erythema annulare centrifugum
See more images of erythema annulare centrifugum.
Erythema annulare centrifugum most often occurs in adults, but all ages can be affected. The average age of onset is 40 years [1].
Erythema annulare centrifugum has been shown to occur in association with underlying medical conditions and medications in 33–72% of cases [1,2]. It is thought to be a form of hypersensitivity reaction.
The most commonly associated conditions are:
Dietary causes of erythema annulare centrifugum include blue cheese and tomatoes. Stress has also been associated with the disease [1,3].
Erythema annulare centrifugum typically affects the thighs, buttocks, and upper arms. However, any location on the body can be affected.
Erythema annulare centrifugum usually starts as a small pink papule that gradually enlarges over several weeks to form annular plaques with central clearing. These plaques can vary in size from a few millimetres to a few centimetres in size. Annular lesions can be partial (arciform) and coalesce to form polycyclic (ringed), serpiginous (wavy), and gyrate (revolving) patterns.
Classically, the annular or arciform lesions have an advancing outer erythematous edge with a trailing (inner) scaly edge. The rash may be itchy.
Erythema annulare centrifugum can sometimes be diagnosed on clinical features alone if the characteristic trailing scale is present. The diagnosis can be confirmed by skin biopsy in which the typical features of superficial or deep erythema annulare centrifugum are noted: a dense perivascular lymphocytic infiltrate involving either the superficial or deep vascular plexus, which is known as a ‘coat-sleeve’ appearance. Secondary changes to the epidermis may include spongiosis (inflammation of intercellular oedema), parakeratosis (disturbance in the keratinisation process), and hyperkeratosis (thickening of the outer layer of the epidermis) [2].
Investigations for an underlying cause should be guided by the patient's history and examination findings. An age- and symptom-appropriate cancer screening should be undertaken.
Toenail clippings and skin scrapings should be submitted for mycology if onychomycosis, tinea pedis, or tinea corporis are suspected.
Several skin conditions should be considered in the differential diagnosis of erythema annulare centrifugum. Conditions to consider include other forms of annular erythema:
Other disorders to be considered include:
Annular scaly plaques are also common in discoid eczema, chronic plaque psoriasis, seborrhoeic dermatitis, pityriasis rosea, porokeratosis, and sarcoidosis.
It is essential to identify and treat the underlying cause of erythema annulare centrifugum where possible, such as a cutaneous fungal infection.
Topical medications that have been used to treat erythema annulare centrifugum include:
Systemic medications that have been used to treat the underlying cause of erythema annulare centrifugum include:
Etanercept [8] has been reported to induce remission in a case of widespread erythema annulare centrifugum.
Erythema annulare centrifugum tends to recur over several months or years, but it can spontaneously remit. Kim et al showed that 18.5% of affected individuals had persistent skin lesions for over 1 year and that the average duration of skin lesions was 4.7 months [1].