Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Dushiyanthi Rasanathan, House Surgeon, General Medicine, North Shore Hospital, Auckland, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. June 2019.
Ethnic dermatology is an area of interest dedicated to the presentation, diagnosis, and management of skin disorders in patients who have pigmented skin. It is also referred to as dermatology in skin of colour [1].
Ethnicity is defined as “the ethnic group or groups a person identifies with or has a sense of belonging to. It is a measure of cultural affiliation, in contrast to race, ancestry, nationality, or citizenship” [2]. Ethnicity is self-identified, and an individual may belong to more than one ethnic group. Ethnic dermatology highlights the importance of genetics, biology, and cultural practices on skin conditions.

Ethnic diversity
The manifestation of skin diseases can vary between ethnic groups and skin colours.
Clinical dermatology emerged as an independent discipline in Europe during the 19th and 20th centuries [3]. This was a time in which anthropologists and philosophers categorised human racial groups within a hierarchy, being influenced by social ideas of the period [4].
Classical descriptions of skin conditions were based on patients with lighter skin [1]. Traditional dermatology does not encompass the social and cultural issues of people with darker skin, which may influence dermatological presentation and the patient’s perspective towards disease, healthcare, and treatment [5].
Ethnic dermatology is a non-specific term for a heterogeneous group with darker or non-Caucasian skin [3].
Melanin is the key determinant of skin colour. Eumelanin (the normal melanin) and phaeomelanin (a red pigment) are synthesised by melanocytes in the basal layer of the epidermis. The colour of the skin is dependent upon the variation in the amount and type of melanin [4].
Eczema presents as itchy, dry skin, with erythema visible in fair skin due to dilatation of the capillaries.
In more pigmented skin, erythema is inapparent and is replaced by patches of darkened skin colour. Inflammation results in the release of inflammatory mediators that increase melanogenesis by the melanocytes, resulting in post-inflammatory hyperpigmentation [3,9].
Skin cancers in skin of colour, including melanoma, often present at an advanced stage or atypically with a poorer prognosis than skin cancer in lighter skin populations [8,10].
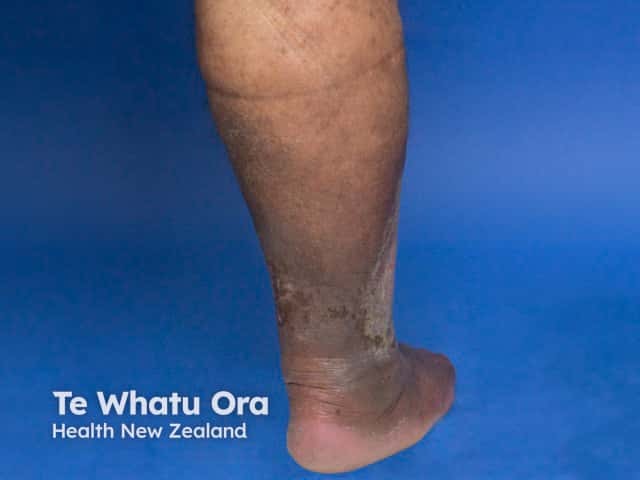
Venous eczema
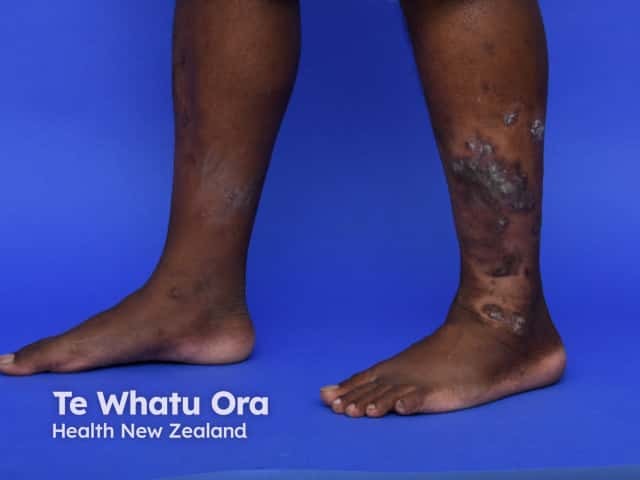
Psoriasis
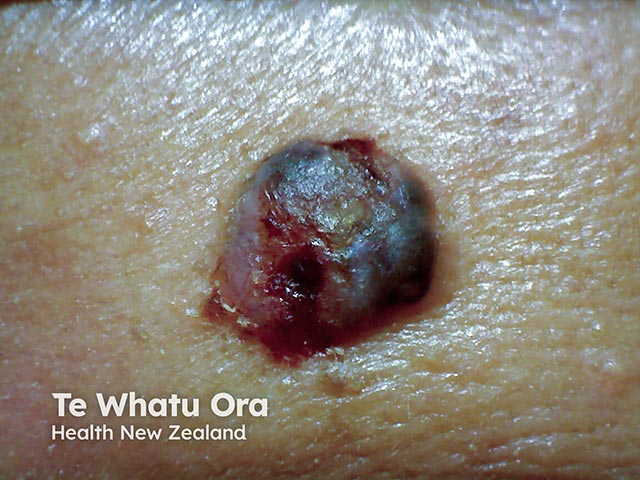
Basal cell carcinoma
Cultural definitions of beauty vary from culture to culture and are associated with deeply entrenched beliefs within ethnic populations.
Ethnic groups with these beliefs often come from a background of colonisation by Europeans, who historically held positions of greater status and wellbeing compared to the indigenous populations. The legacy continues with advertising continuing to promote lighter skin as a standard of wealth, power, modernity, and wellbeing [4]. Conversely, those with lighter skin may be seeking a tan or to disguise their skin colour with make-up.
Skin lightening or bleaching creams involve the cosmetic use of a range of agents widely available in the Middle East, Asia, South America, and elsewhere that are sold in ethnic stores and supermarkets — despite legal restrictions in many jurisdictions due to their serious potential side effects [11].