Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Lesions (cancerous) Diagnosis and testing
Author: Rajan Ramji, Final Year Medical Student, University of Auckland, Auckland, New Zealand. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell and Maria McGivern. October 2017.
Introduction - basal cell carcinoma
Introduction - skin of colour
Demographics
Causes
Clinical features
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment - basal cell carcinoma
Treatment - advanced or metastatic basal cell carcinoma
Follow-up
Outcome
A basal cell carcinoma (BCC) is a keratinocytic or non-melanoma skin cancer formed by uncontrolled growth and replication of basal cells in the lower levels of the epidermis. A BCC is sometimes referred to as a rodent ulcer or basalioma.
Skin of colour is a subjective term referring to natural skin pigmentation ‘darker’ than white (ie, brown or black skin). When compared against a graded assessment of skin colour types such as the Fitzpatrick scale, ‘skin of colour’ may refer to skin classified as type IV or higher [1]. In some contexts, ‘skin of colour’ is also used to describe the skin type of a non-white ethnic group including those of African, Asian, South American, Pacific Island, Maori, Middle Eastern, and Hispanic descent [1]. See ethnic dermatology.

Superficial basal cell carcinoma
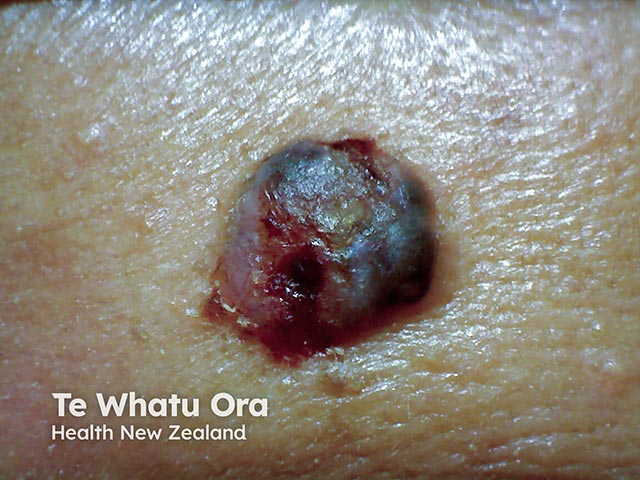
Nodulocystic basal cell carcinoma

Ulcerated basal cell carcinoma
Basal cell carcinomas (BCC) are among the most commonly diagnosed cancers worldwide and accounts for 65–75% of skin cancers [2]. It is the most common form of skin cancer seen in Caucasians, Asians, and Hispanics, and the second most common form of skin cancer seen in African Americans and Asian Indians [3].
Reported incidence rates of BCC vary across different studies and periods, although the BCC incidence rates per 100,000 population across the last 50 years include:
The incidence rates of BCC globally are increasing, and this trend is significantly more prominent in white-skinned people, particularly in older age groups and in women [5,6]. Most diagnoses of BCC occur at over 50 years of age and peak at around 70–80 years of age in both men and women, regardless of skin colour [5].
Basal cell carcinoma is more common in individuals with:
Ultraviolet (UV) radiation exposure (sunlight) is a much more significant risk factor for BCC in white-skinned people [3]. However, while sunlight is generally less of a risk factor in skin of colour, susceptibility to BCC varies between individuals with the same skin type depending on their ethnic origins [4].
BCC is thought to begin from an uncontrolled proliferation of basal cells in the skin following an abnormal genetic transformation, usually as a result of sun exposure as UV light damaging and mutating DNA [5]. In addition, UV radiation suppresses the ability of the immune system to detect and destroy tumour cells. In darker skin, a higher content of UV radiation-absorbing melanin protects the DNA from mutation and damage.
Regardless of skin colour, BCCs can occur anywhere on the skin. The most common sites are the face and ears, neck, shoulders, and back. There are various subtypes of BCC; these subtypes are described below.
A nodulocystic BCC is a small and slow-growing translucent lesion with rolled edges and telangiectasia.
Superficial BCC is the most common type of BCC found in younger adults.
Morphoeic BCC is also known as morpheaform or sclerosing BCC.
Basosquamous BCC is also known as mixed BCC and SCC.
Adenoid BCC is a rare histological variant of BCC.
Fibroepithelial tumour of Pinkus is a warty plaque, usually found on the trunk.
The diagnosis of BCC in skin of colour can be difficult due to its rarity and pigmentation. More than 50% of BCCs found in skin of colour are pigmented with a ‘pearly’ brown or black appearance.
Nodular BCCs are the predominant subtype found in skin of colour, while morphoeic BCCs are uncommon. Adenoid BCC is more common than in Caucasians.
Complications of BCCs may include:
Basal cell carcinoma has an estimated 3–10% 5-year recurrence rate depending on whether the treated lesion is a primary BCC or is itself a recurrence. Most recurrences are evident 4–12 months after treatment. Recurrence is more likely with:
The type of treatment received can also influence recurrence rates. Higher recurrence rates (~7–10%) may be seen with all treatment methods other than Mohs micrographic surgery (~1%) [8].
There is a significantly increased risk of developing new BCCs after a previous BCC. Estimates from various studies have suggested a 3-year cumulative risk of between 30 and 77% for new BCC formation. Factors associated with new BCC formation may include:
Advanced BCCs are often a result of neglect as BCCs are very slow-growing tumours, often taking months to years to reach this stage. They may be several centimetres in diameter. Advanced BCCs may infiltrate tissues below the skin and are very difficult to treat surgically.
Metastatic or invasive BCCs are rare, with an estimated occurrence rate of 0.03–0.55%. The primary BCC is often large, neglected or recurrent, and located on the head and neck region. It may arise in sites exposed to ionising radiation or ones that have had multiple prior treatments. Metastatic BCCs can be fatal.
Basal cell carcinomas are diagnosed by their typical appearance clinically and on examination using a dermatoscope [3]. The diagnosis is confirmed by incisional biopsy or excisional biopsy.
Most diagnoses occur at over 50 years of age and peak at around 70–80 years of age in both men and women, regardless of skin colour [5]. Men are much more likely to develop BCC — at double the incidence rate of women in some locations [5,8].
In patients with advanced BCCs, it can be important to determine the depth of tumour invasion and the spread to surrounding tissue. The Union for International Cancer Control (UICC) 8th edition staging system for cutaneous carcinomas (skin cancers) is a commonly used system.
TX: Primary tumour cannot be assessed
T0: No evidence of primary tumour
Tis: Carcinoma in situ
T1: Tumour ≤ 2 cm, without high-risk features
T2: Tumour > 2 and < 4 cm
T3: Tumour with the invasion of maxilla, mandible, orbit or temporal bone
T4a: Tumour with gross cortical bone/marrow invasion
T4b: Tumour with skull base or axial skeleton invasion, including foraminal involvement and vertebral foramen involvement to the epidural space
NX: Regional lymph nodes cannot be assessed
N0: No regional lymph node metastasis
N1: Metastasis in one local lymph node ≤ 3 cm
N2: Metastasis in a single ipsilateral lymph node > 3 cm and ≤ 6 cm or in multiple ipsilateral nodes ≤ 6 cm.
N3: Metastasis in lymph node ≥ 6 cm
There are several lesions that can be mistaken for a basal cell carcinoma, especially:
Malignant lesions, such as cutaneous SCC and melanoma, have a peak incidence at the same approximate age (> 50 years) as BCC and may be present simultaneously.
Treatment options are the same, regardless of skin colour. Excisional biopsy with a 3–5 mm margin is the standard and recommended treatment for most BCCs.
Smaller margins increase the risk of recurrence. Deeper incisions and more complex wound closure (flap or skin graft) may be required for larger BCCs. The removed specimen is then examined by a pathologist for a final diagnosis and disease staging [9].
Potential side effects of treatment can include infection, scarring, and temporary or permanent loss of sensation due to nerve severing.
Cryotherapy is the treatment of a superficial skin lesion by freezing it, usually with liquid nitrogen [9]. It is suitable for small superficial BCCs (≤ 1cm) on covered areas of trunk and limbs, and not advised to treat BCCs on head, neck and knees. Cryotherapy:
Complications and side effects of cryotherapy include:
Shave, curettage, and electrocautery are superficial forms of surgery. These techniques require local anaesthesia but are quick to perform and do not require sutures [9].
Mohs micrographic controlled surgery involves removing skin tissue in successively deeper horizontal sections under a local anaesthetic. Each section is examined with a microscope to identify cancerous tissue. Sections are continuously removed until no further cancerous tissue is identified [10].
Mohs margin-controlled micrographic excision has very high cure rates when performed by trained dermatologists or dermatological surgeons.
Imiquimod is a topical immune response-modifying drug [9,10]. Imiquimod cream is used when surgical removal is inappropriate.
Side effects and complications of imiquimod cream include:
5-Fluorouracil cream is a topical cytotoxic agent [9,10]. It is used to treat small superficial BCCs.
Side effects and complications with the use of 5–fluorouracil cream include:
Photodynamic therapy (PDT) refers to a technique in which BCC is treated with a photosensitising chemical and exposed to light several hours later [9,10].
Side effects and complications of photodynamic therapy include:
Radiotherapy or X-ray treatment can be used to treat primary BCCs or as adjunctive treatment, if margins are incomplete [9,10]. Radiation is mainly used if surgery is not suitable. It is best avoided in young patients and in people with genetic conditions that predispose them to skin cancer. The best cosmetic results are achieved using multiple fractions.
Side effects and complications with the use of PDT include:
Advanced or metastatic BCCs require multidisciplinary consultation. A combination of treatments may be used including:
There are no established guidelines for the follow-up after the removal of a BCC. An annual skin check is recommended for anyone who has had a BCC, given the estimated 30–77% cumulative risk of experiencing another one within three years. [8–10].
Year-round protection against excessive sun exposure is essential in all skin types.
Basal cell carcinomas are very slow-growing tumours and are unlikely to reach an advanced stage unless significantly neglected. As long as the tumour has been completely excised, BCC does not recur. However, another may develop elsewhere.
The prognosis is of the rare metastatic BCC is very poor, with a median survival time of 8 months following diagnosis [3,10].
Trakatelli M, Morton CA, Nagore E, et al. Guideline on the treatment of basal cell carcinoma. Paris: European Dermatology Forum, 2012. Available at: https://www.caraderm.org/upload/reco-Eur-CBC.pdf (accessed May 2024).