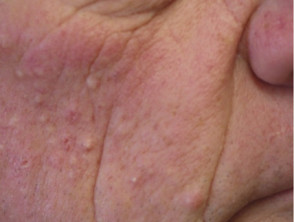
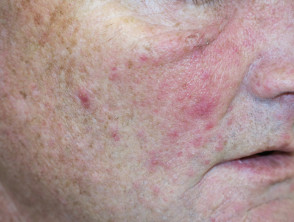
What are follicular eruptions?
Follicular eruptions are skin conditions based on the hair follicle.
Follicular eruptions due to drugs may be acute or chronic eruptions. They present with monomorphic erythematous follicular papules and pustules.
Follicular eruptions due to drugs are also known as acneiform eruptions, papulopustular eruptions, drug-induced folliculitis and drug-induced acne.
Who gets follicular eruptions due to drugs?
Follicular eruptions are relatively uncommon, representing approximately 1% of adverse cutaneous reactions to drugs. They are most likely to occur on certain medications, and in acne-prone patients and age groups such as adolescents, with males thought to be more frequently affected than females.
Follicular eruptions due to drugs are easier to diagnose in age groups that do not typically experience acne vulgaris as this is a much more prevalent disorder and so the diagnosis of drug-induced acne is often not considered initially.
The risk of an eruption developing is proportional to the dose and duration of therapy.
Which drugs cause follicular eruptions?
The classes of drugs (and common causative individual medications within these classes) that are best known to cause follicular eruptions are:
- Antibiotics (isoniazid, rifampicin and tetracyclines)
- Steroids (adrenocorticotropic hormone [ACTH], androgens, systemic corticosteroids)
- Hormones (oral contraceptives)
- Halogens (iodides and bromides)
- Immunosuppressants (azathioprine, ciclosporin, sirolimus)
- Lithium
- Anticonvulsants
- Epidermal growth factor receptor inhibitors (EGFRIs)
- Vitamins (B1, B6, B12).
Why do some drugs cause follicular eruptions?
There are proposed mechanisms for the ways in which some drugs are likely to cause folliculitis.
- Steroids have long been known to cause drug-induced acne through their effect on sebaceous glands.
- Lithium does not show a clear dose-dependent relationship with follicular eruptions but high concentrations of lithium have been found in the skin, suggesting it can accumulate there and resulting in the occurrence of follicular eruptions.
- Sirolimus is thought to induce acne because it inhibits epidermal growth factor.
- The mechanism by which EGFRIs cause follicular eruptions is unclear, but there are EGFR receptors in the epidermis, sebaceous glands and hair follicles, as well as in the keratinocytes. It has been proposed the effect of EGFRIs on the keratinocytes possibly results in apoptosis and then vesicle and pustule formation.
What are the clinical features of follicular eruptions due to drugs?
The time course of follicular eruptions depend on the responsible drug.
- Acute eruptions usually appear within the first 2 weeks of a course of medication.
- The papules and pustules often erupt over a short period of time (days to weeks in the case of steroids, halogens and EGFRIs).
- Chronic eruptions may appear after months or years on a medication such as lithium or anticonvulsants.
Typical characteristics of drug-induced follicular eruptions include:
-
- Crops of erythematous papules and pustules that appear similar to each other
- Located on the trunk, shoulders, upper arms and face
- Unlike acne vulgaris, comedones are absent.
Follicular eruptions due to drugs
How are follicular eruptions due to drugs diagnosed?
A follicular eruption due to a drug is generally diagnosed on the basis of the clinical appearance and a history of exposure to a drug known to be causative.
It may be appropriate to check the levels of suspected drugs where they are measurable (eg, lithium).
If a skin biopsy is taken, histological features may reveal:
- Dilation of the hair follicles
- Erosion of the infundibular epithelium
- Aggregates of neutrophils
- A perifollicular lymphoneutrophilic infiltrate, including foreign body giant cells.
Bacterial culture is not usually necessary, and is negative. Microscopy sometimes reveals Malassezia yeasts, particularly when corticosteroids are the cause of the eruption (steroid acne).
Differential diagnosis
Other diagnoses that should be considered in patients with follicular eruptions include:
- Acne vulgaris
- Folliculitis due to infection (bacterial, viral and fungal) or irritant factors.
It is also possible to have a drug-induced folliculitis complicated by an overlying infection, especially in EGFRI-induced folliculitis.
What is the treatment for follicular eruptions due to drugs?
The initial, and most important, management should be to withdraw the offending medication if this is possible.
The evidence for best treatment of persistent follicular eruptions is not robust and is the subject of ongoing research in patients who must continue the causative drugs.
Mild folliculitis may respond to topical treatment for acne:
- Benzoyl peroxide
- Clindamycin or erythromycin
- Retinoids, such as tretinoin.
If required, systemic therapy may include:
- A tetracycline antibiotic, such as doxycycline and minocycline
- Oral isotretinoin.
What is the outcome for follicular eruptions due to drugs?
Most cases of follicular eruptions due to drugs will resolve within a few weeks of withdrawal of the causative medication. In persistent cases, the advice of a dermatologist should be sought.