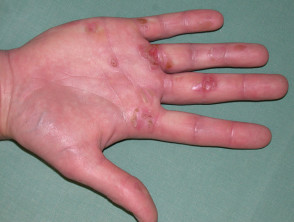
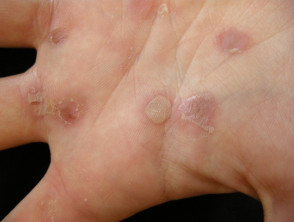
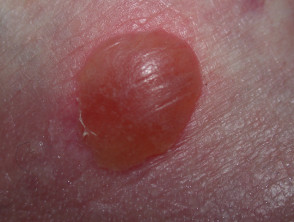
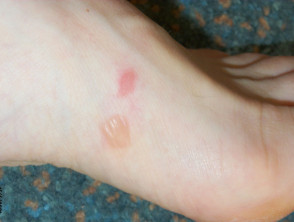
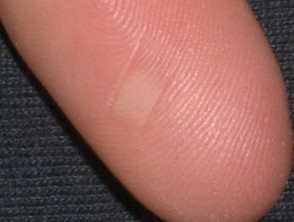
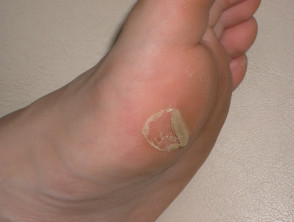
What is a friction blister?
A friction blister is a blister caused by the skin repeatedly rubbing against another object. It most often forms on the palms, fingers, soles, sides of the feet and toes. The top of the blister is rubbed off where skin is thinner, such as the top of the hand or foot, forming an abrasion. In areas of thinner skin, friction causes chafing without blistering.
What causes friction blister?
A friction blister occurs when there is contact, pressure and movement between the skin and something touching it – such as a heel rubbed by a new or unfamilar shoe.
Sheer forces cause mechanical separation of the layers of epidermal cells. The gap fills with fluid, forming a subepidermal bulla (blister). A blister forms more quickly if pressure and movement on the skin is severe or the skin is damp.
Who gets friction blisters?
Friction blisters occur from time to time in nearly males and females of all ages. Exacerbating factors include:
- Heat — they are particularly prevalent in tropical climates.
- Prolonged or vigorous exercise — they are common in athletes (especially marathon runners) and soldiers; one third of 872 American soldiers surveyed when in Iraq had blisters.1 Blisters on the palms may arise from rowing, or in children playing on monkey bars.
- Carrying a heavy load increases the risk of blisters.
- Excessive sweating — hyperhidrosis softens the skin so the skin splits more easily.
- Tight, uncomfortable or new shoes, which repetitively rub on one or two areas of skin.
- Unabsorbent or thin socks — these do not absorb moisture well and do not protect the skin adequately from damage by shoes or boots.
- Rough or hard fabrics may cause blisters on other sites, such as armpits or groin.
Blisters may also arise on pressure areas such as the hip, as a complication of surgery or loss of consciousness, classically following barbiturate poisoning.
There are some specific diseases that make the skin more fragile than usual, also causing blisters in response to friction or injury.
- Genetic disposition — epidermolysis bullosa is a group of disorders in which the skin blisters easily.
- Immunobullous disease — epidermolysis bullosa acquisita.
- Metabolic disease — porphyria cutanea tarda
- Sun damage — especially overexposure to solaria or tanning beds
- Certain medications — pseudoporphyria due to nonsteroidal anti-inflammatories or antibiotics (doxycycline)
What are the clinical features of friction blister?
Rubbing on the skin first peels off surface cells. More pressure causes the affected skin to redden, heat up and to sting. The red skin then becomes pale as the blister forms. The blister usually contains clear fluid but bleeding changes the colour to red/brown.
Blisters occur where the stratum corneum (the outer cell layer) is very thick, as is the case on the sole of the foot and palm of hands. Where the skin is thinner, friction tends to sheer off the epidermis completely, resulting in an erosion (sore).
If the blister remains intact, the fluid will resorb and the damaged skin will peel off some days later.
Friction blisters
Should I have any tests done?
Tests are not necessary for typical friction blisters. The following investigations may be considered when blistering is frequent, extensive or failing to heal.
- Swab to check for bacterial infection with Staphylococcus aureus or Streptococcus pyogenes (impetigo or cellulitis).
- Skin biopsy of a new friction blister for histopathology reveals intraepidermal split without inflammation. Specific features may lead to another diagnosis.
- Skin biopsy for direct immunofluorescence, positive in immunobullous diseases, is negative in friction blister.
- Genetic tests may be requested if epidermolysis bullosa is suspected.
Complications of friction blister
Intact friction blisters usually heal up quickly without scarring. Healing is sometimes delayed. Problems may include:
- Pain impeding performance
- Wound infection: this presents with increasing pain and redness around the blister/erosion, a red streak heading for the groin or armpit, and pus formation. Infection is more common in diabetics and immune impaired individuals.
- Pyogenic granuloma may occasionally arise at the site of a blister some days later.
- Scarring due to infection or deeper injury.
How should I treat a friction blister?
Friction blisters will heal on their own. However, dressings are helpful to protect from further damage. Hydrocolloid blister plasters may promote faster healing.
Large blisters can be drained by pricking with a sterile needle. It's best to keep the roof of the blister in place if possible, to reduce pain and lessen the chance of infection. If the roof of the blister has come off leaving an eroded skin surface, clean the wound carefully and apply a clean dressing.
Infected friction blisters or erosions may require topical antibiotics or antiseptics for a few days. Systemic antibiotics must be used if cellulitis occurs. Antibiotics should not be used if the wound is not infected.
Can I prevent friction blisters?
If prone to friction blisters, the following measures may be useful.
- Well-fitting boots and shoes; use orthotics if necessary to reduce pressure points.
- Neoprene insoles
- Moisture absorbent socks, changed as soon as they are damp
- 2 pairs of socks: thinner inner polyester layer and thicker wool or polypropylene outer layer
- Gaiters to prevent gravel and plant materials entering the footwear
- Lamb's wool padding over and around areas prone to blister
- Various proprietary foam padding, cushioning and protective barrier products, which are available at the shoe counter of your local pharmacy
Antiperspirant, petroleum jelly or silicone lubrication, powders and topical skin adhesives have been advocated and may prove useful. However, they have not been shown scientifically to reduce discomfort or improve healing.
Some hardening occurs with repetitive low intensity exercise because of callus formation (epidermal thickening).