Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Millicent Osti, Resident Medical Officer, The Royal Melbourne Hospital, Melbourne, VIC, Australia; A/Prof Rosemary Nixon, Dermatologist, East Melbourne Dermatology, Melbourne, VIC, Australia. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. October 2018.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Lipodermatosclerosis is a chronic inflammatory condition characterised by subcutaneous fibrosis and hardening of the skin on the lower legs.
Lipodermatosclerosis is also known as sclerosing panniculitis and hypodermitis sclerodermaformis.
Lipodermatosclerosis is common, affecting middle-aged or older people. It is more common in women and is associated with immobility and a high body mass index (obesity) [1].
Lipodermatosclerosis is an inflammatory skin condition resulting from underlying venous insufficiency. This is caused by:
The resulting venous hypertension causes an increase of leukocytes within the veins, which then migrate into surrounding tissue. The leukocytes become activated, attracting and releasing proinflammatory cells and cytokines, inducing a chronic inflammatory state. Increased collagen production leads to the fibrosis of subcutaneous fat [2].
Acute lipodermatosclerosis may mimic cellulitis, with induration, erythema, pain, itch, aching, and a feeling of swelling or heaviness in one or, more often, both lower limbs [2].
In the acute phase, signs may be localised to a single plaque but are usually more widespread. The most commonly affected areas are the pretibial or medial aspect of the leg.
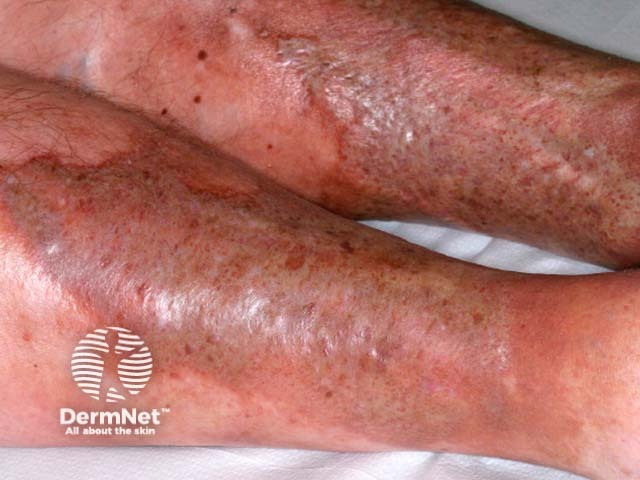
Acute lipodermatosclerosis
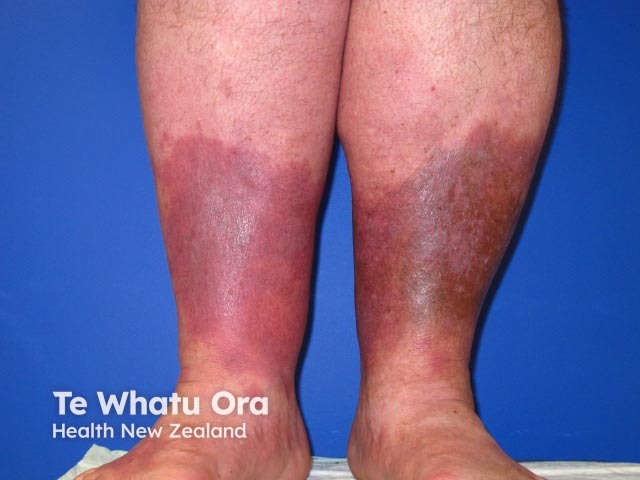
Acute lipodermatosclerosis
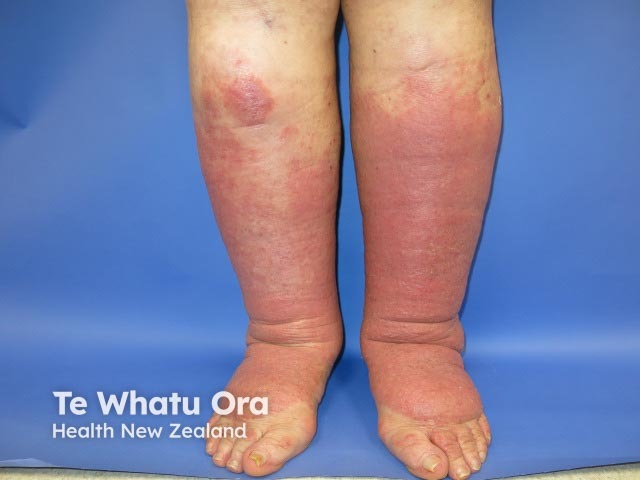
Acute lipodermatosclerosis
See more images of acute lipodermatosclerosis.
Induration, erythema, and pain continue in the chronic phase of lipodermatosclerosis. Subcutaneous fibrosis may result in significant narrowing of the distal lower limb, causing the leg to have an ‘upside-down champagne bottle’ appearance [1,2].
Other clinical features of chronic venous insufficiency may be present, including hyperpigmentation of the skin from haemosiderin deposition, atrophie blanche, varicose veins, venous eczema, and venous ulcers.
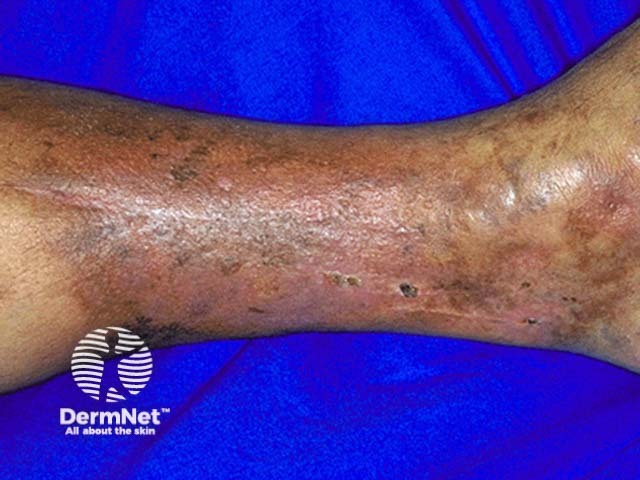
Lipodermatosclerosis
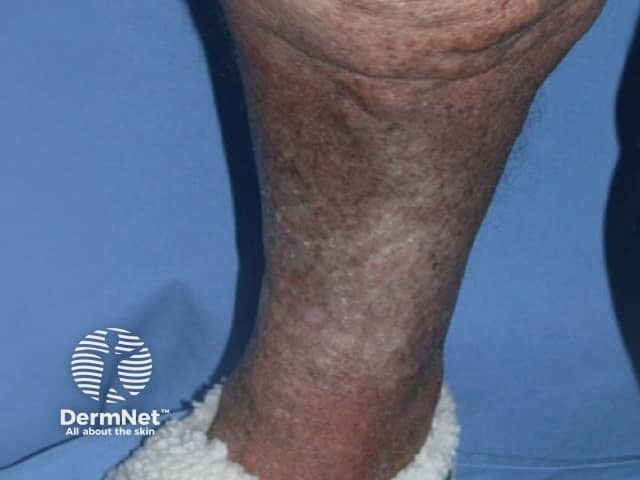
Lipodermatosclerosis
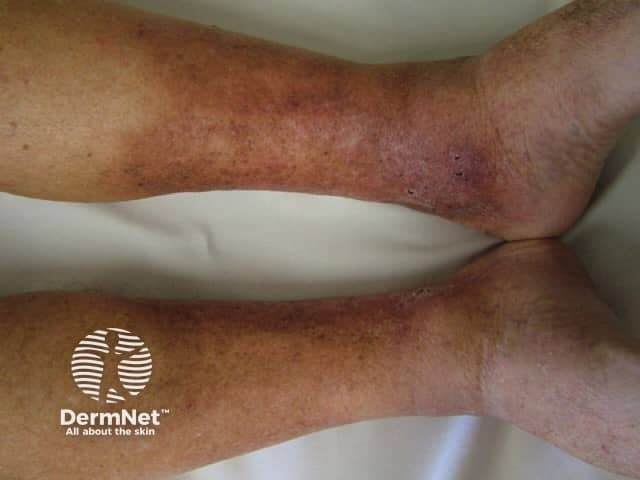
Lipodermatosclerosis
See more images of chronic lipodermatosclerosis.
Lipodermatosclerosis is associated with poor wound healing because of the chronic inflammatory state and fibrosis. Venous ulcers commonly co-exist and may be difficult to treat.
Lipodermatosclerosis is usually diagnosed clinically. Underlying venous insufficiency may be confirmed using Doppler studies.
A biopsy is helpful but should be performed with caution because of the likelihood of poor wound healing [3]. Any biopsy also needs to include the panniculus. The characteristic features seen upon biopsy are dependent on the stage of disease but include subcutaneous lobular and septal changes including:
Differential diagnoses for lipodermatosclerosis can include:
Physical activity (walking) should be encouraged to increase the functionality of the calf muscle pump. Weight reduction is effective if obesity is a factor.
Mechanical compression therapy using compression stockings or socks is the mainstay of treatment, encouraging venous return and assisting with symptom control, but may be poorly tolerated in some individuals.
Elevation of the legs can help reduce oedema and pain.
Treatment of underlying venous insufficiency can improve symptoms and may reduce the risk of ulcer recurrence. Referral to a vascular surgeon should be considered. Leg vein therapies include:
Venous insufficiency is a progressive disease. Although treatment can improve symptoms or slow progression, its associated conditions such as lipodermatosclerosis are usually chronic and recurring.