Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Cliff Rosendahl, Associate Professor, School of Medicine, The University of Queensland, Australia, 2013. Reviewed by Prof Luc Thomas, Lyon 1 University, France. Updated by Dr Todd Gunson, Dermatologist, Auckland, New Zealand in July 2014.
What is the nail matrix? Introduction Why is a biopsy undertaken? Procedure Trap door technique Risks
The nail matrix consists of specialised cells that produce the nail plate. It is located at the end of the digit (finger or toe) under the the skin beyond the distal phalangeal joint. It can be seen protruding as a white half-moon shape at the base of some nails.
Nail matrix biopsy is a surgical procedure in which a tissue specimen is obtained from the nail matrix.
Nail matrix biopsy is undertaken to make or confirm a diagnosis of a disorder that is affecting the nail plate. The following list describes some conditions in which this procedure may be undertaken.
Nail matrix biopsy is usually undertaken under local anaesthetic. Most often a digital block is performed, whereby the sensory nerves entering at the base of the affected finger or toe are numbed via an injection.
Various techniques are used to biopsy the nail matrix depending on the situation and the specialist's preference. The overlying nail plate may be removed for pathological examination, or replaced after the procedure. All techniques involve examining the matrix for the origin of the problem. It is important that adequate and appropriate sample is taken to make an accurate diagnosis, while minimising permanent damage/scarring to the matrix tissue.
Techniques include:
To minimise nail dystrophy, the biopsy should be performed on the distal matrix wherever possible, because this is responsible for producing the undersurface of the nail plate.
One technique is the “trap door” or “pop the bonnet” method used to biopsy of pigmented nail matrix lesions. This allows a direct view of the nail matrix permitting precise targeted biopsy of the lesion.
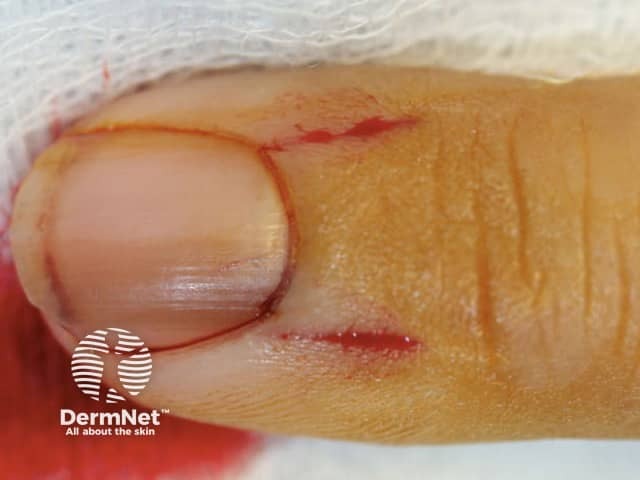
Figure 1
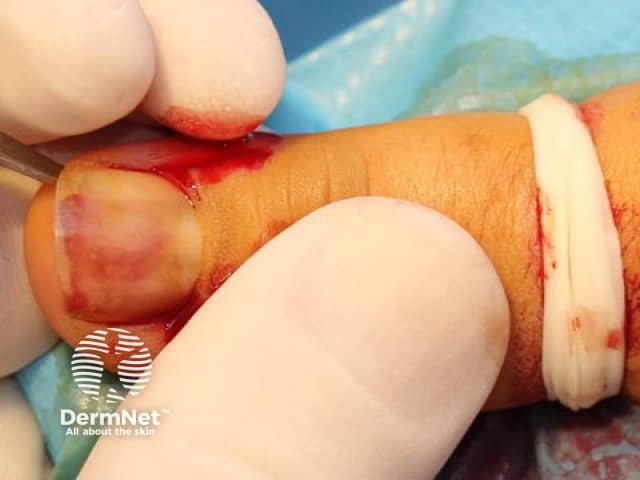
Figure 2
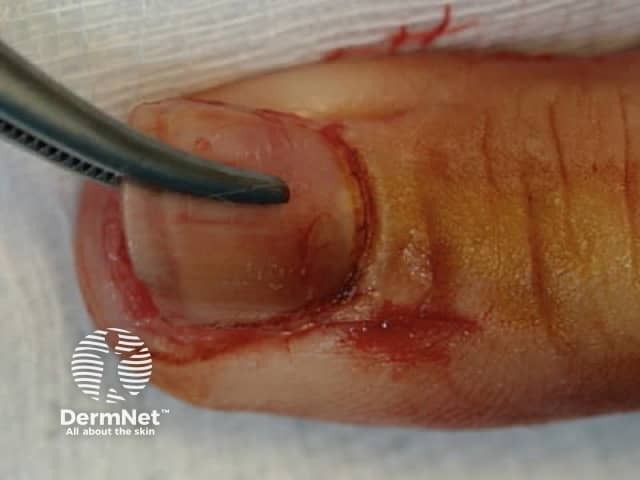
Figure 3
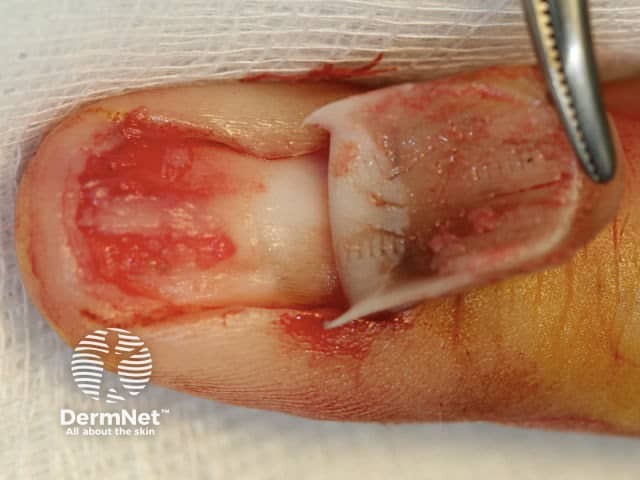
Figure 4
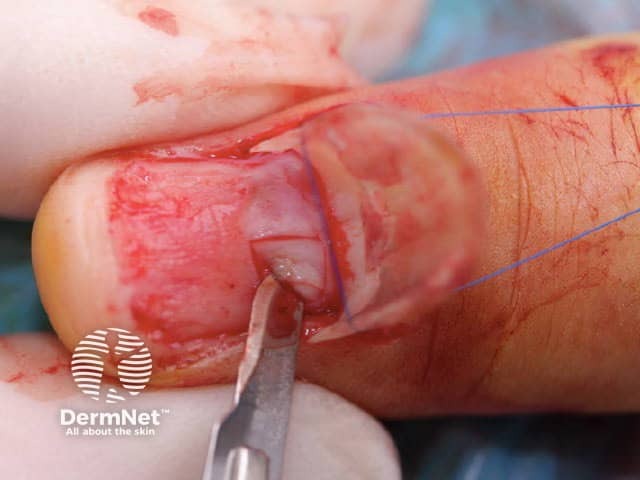
Figure 5
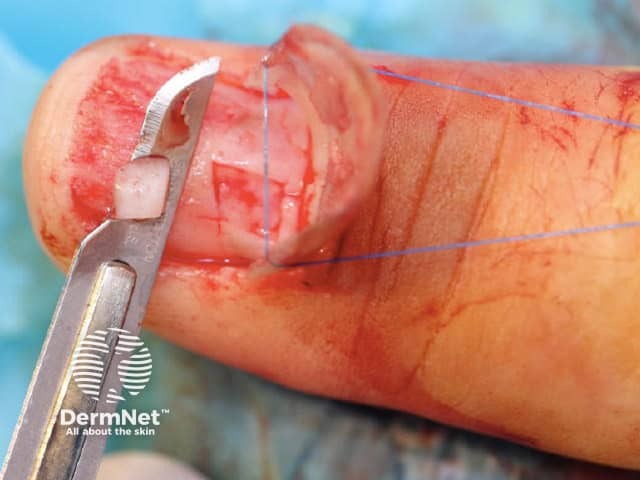
Figure 6
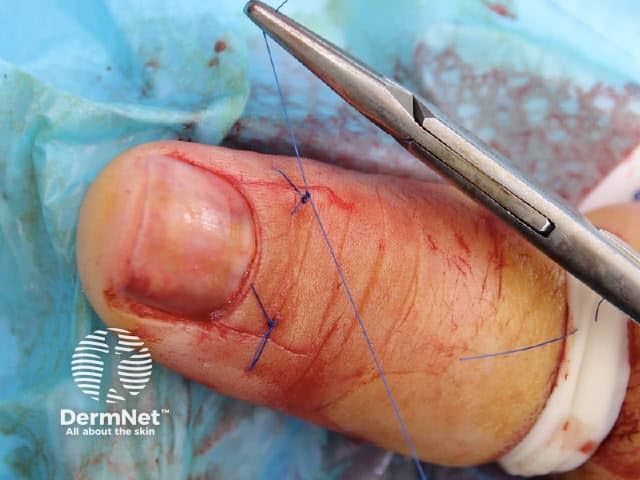
Figure 7
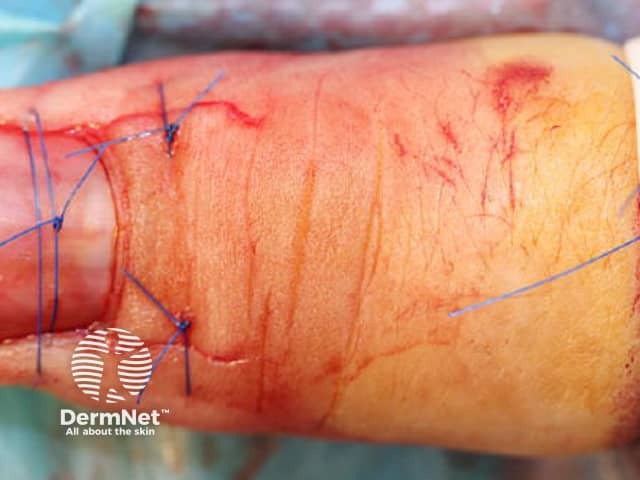
Figure 8
Nail biopsy can lead to any of the usual complications from a surgical procedure, such as bleeding, infection, nerve damage, and scarring.
Scarring of the nail matrix is common and may result in permanent deformity of the nail plate. Persistent paraesthesia (abnormal sensation) is one of the most common complications (7% in one study), likely due to damage to small nerves during the surgery. Overall, the complication rate following nail surgery performed by a specialist is low.