Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Vanessa Ngan, Staff Writer, 2003; A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, February 2016; DermNet Update August 2021. Copy edited by Gus Mitchell
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Nail psoriasis, also known as psoriatic nail dystrophy, is due to psoriasis involving the nail matrix or nail bed, resulting in specific and non-specific clinical changes in the nail.
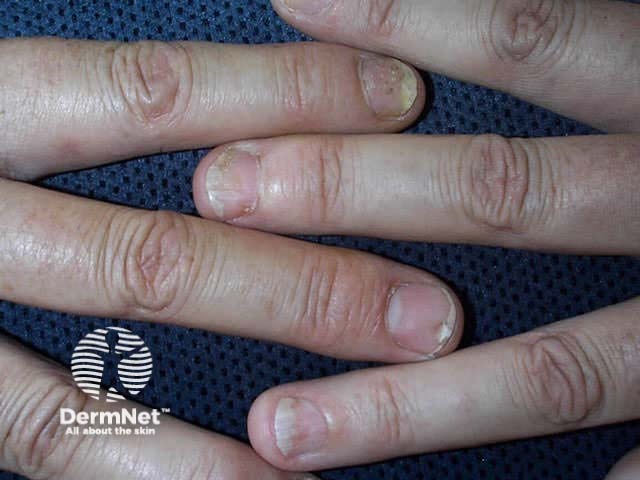
Nail psoriasis
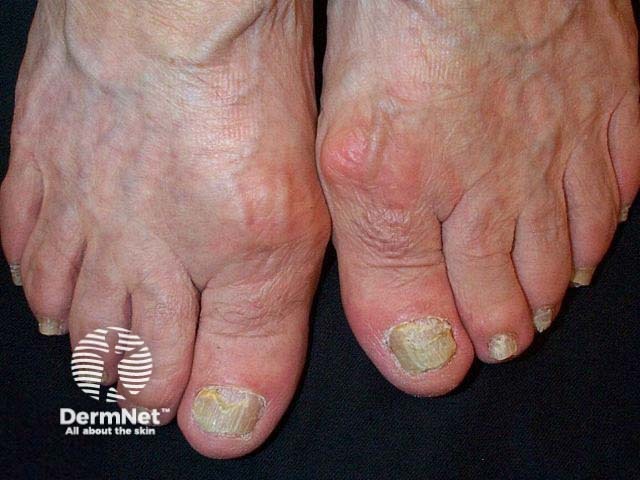
Nail psoriasis
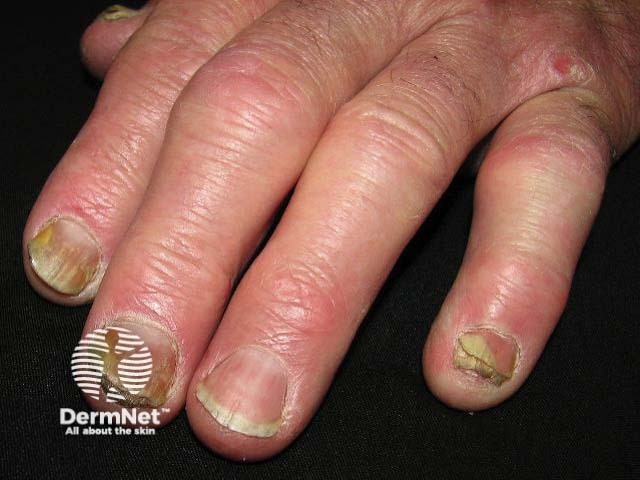
Nail psoriasis
Nail psoriasis affects 90% of patients with chronic plaque psoriasis at some time in their life. It is more common in adults with a prevalence of up to 80%, compared to children in whom it has been reported in 7–13%. In the absence of skin or joint disease, psoriatic nail disease has been described in 5–10% of adults.
Psoriatic nail disease may be a risk factor the development of psoriatic arthritis and is often associated with prolonged severe cutaneous psoriasis.
Nail psoriasis can affect all races and age groups, and both sexes, although a male predominance has been reported in one large case series.
Psoriasis is a multifactorial systemic disease including inflammation and epidermal hyperproliferation.
Nail psoriasis can involve the nail bed, nail matrix, hyponychium, and nail folds.
Theories include:
Fingernails and toenails can be affected by nail psoriasis.
Psoriatic nail dystrophy can cause tenderness and pain, altered sense of fine touch, and difficulty picking up or manipulating objects such as shoelaces or buttons.
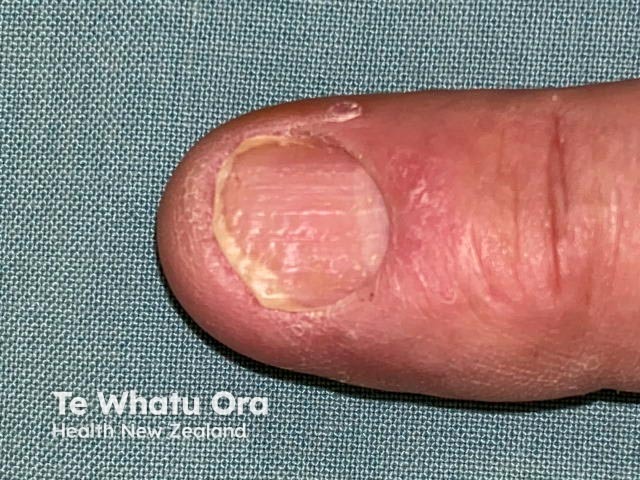
Pitting and onychorrhexis
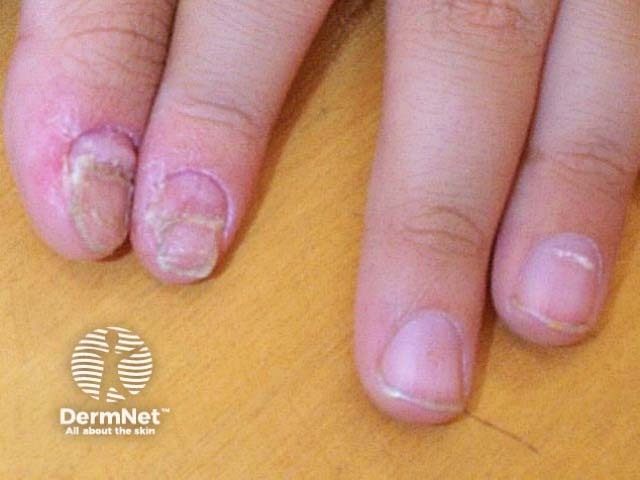
Leukonychia and Beau lines
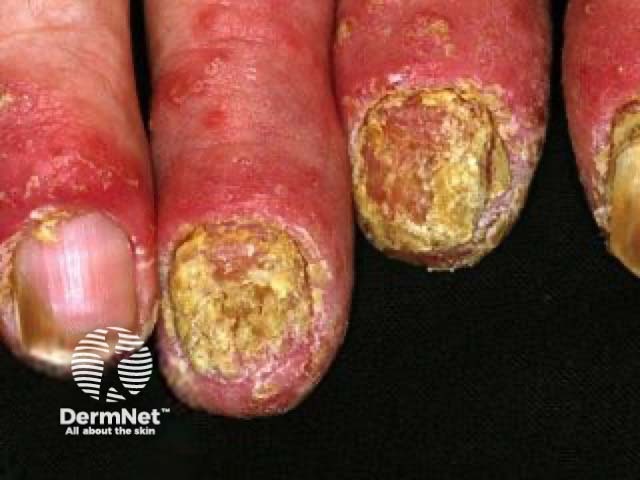
Crumbling nails

Onycholysis and salmon patch
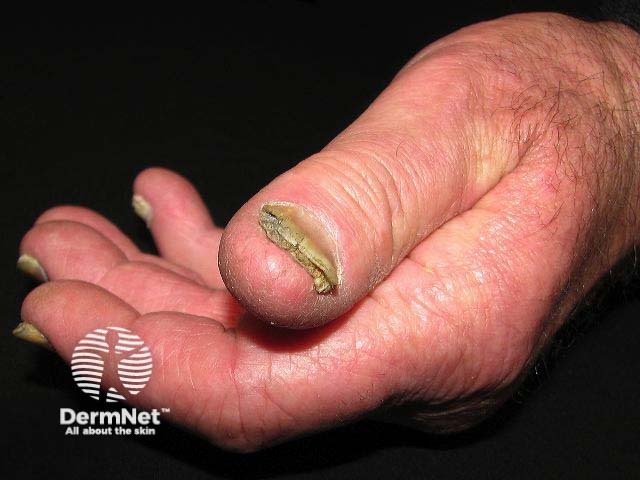
Subungual hyperkeratosis
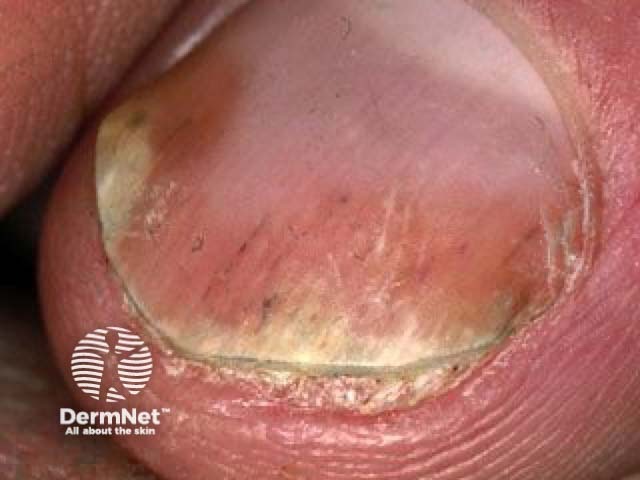
Splinter haemorrhages
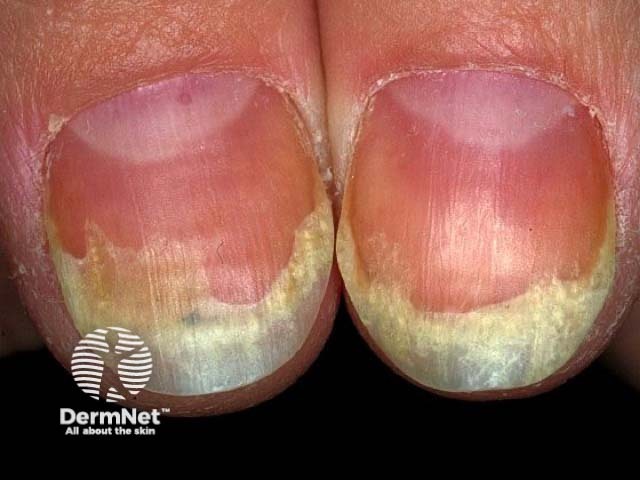
Onycholysis and red dot in lunule
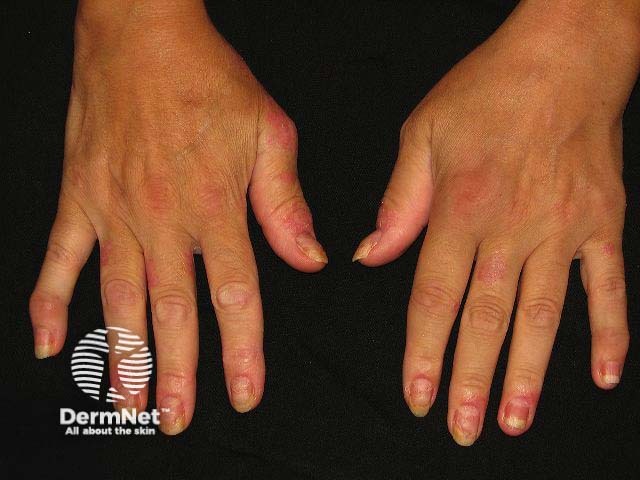
Periungual psoriasis and paronychia
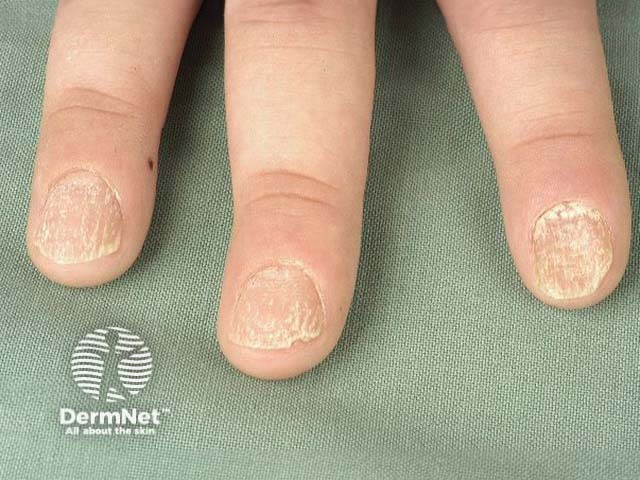
Trachyonychia
[see also Nail psoriasis images]
Nail psoriasis is usually diagnosed clinically in a patient with psoriatic arthritis and/or cutaneous psoriasis.
The severity of nail psoriasis can be estimated using the Nail Psoriasis Severity Index (NAPSI) in which each nail is divided into quadrants and scored for clinical signs to come up with a numerical score.
Nail clippings for fungal microscopy and culture should be taken as onychomycosis may precede or complicate psoriatic nail dystrophy, and immunosuppressive medications may be used in treatment.
A proximal nail matrix biopsy is occasionally needed to confirm the diagnosis of nail psoriasis, particularly in the absence of signs of psoriasis elsewhere or where only a single nail is affected and a tumour cannot be excluded by other means. Biopsy can lead to permanent nail deformity.
Nail psoriasis has a variable response to treatment. The visible response may take weeks or months due to slow growth of the nail plate, and relapses are common.
Psoriatic nail disease can fluctuate in severity over time and can resolve spontaneously.