Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Mark Duffill, Dermatologist, Hamilton, New Zealand, 2008.
Pressure urticaria is a form of chronic inducible urticaria characterised by the appearance of weals and/or angioedema after pressure to the skin.
Pressure urticaria is uncommon but probably not rare. It is a chronic disease with a mean duration of 9 years. The peak age of onset is in the 20s and 30s. It is also called delayed-pressure urticaria/angioedema.

Pressure urticaria
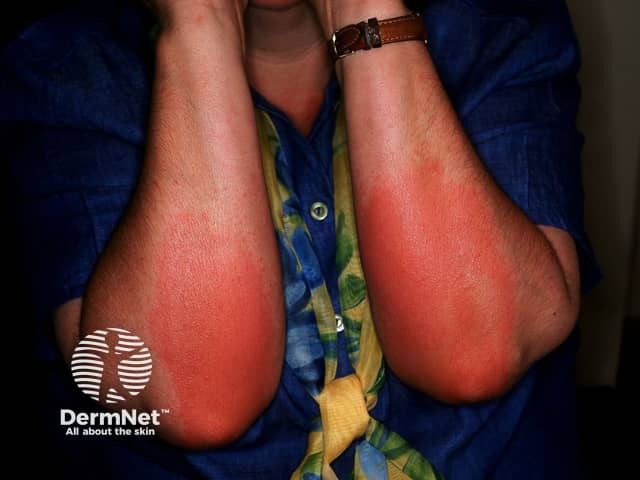
Pressure urticaria
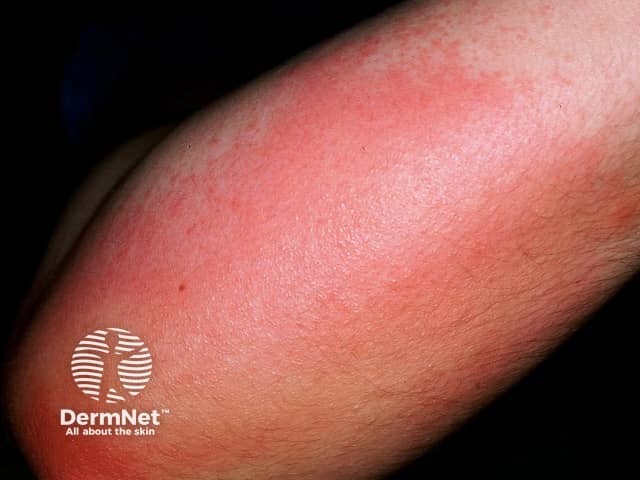
Pressure urticaria
The weal in pressure urticaria consists of redness and swelling of the skin and subcutaneous tissues. Lesions may last for 8–72 hours.
Pressure urticaria has a significant adverse impact on the quality of life of patients, with important limitations in everyday activities such as prolonged walking or standing. It can be disabling in patients who perform manual labour.
The cause of pressure urticaria is unclear but it is likely to be an autoimmune disease. Cells called mast cells are an important part in the process. Mast cells are tissue cells that contain chemicals, including histamine, which provoke wealing.
The diagnosis of delayed pressure urticaria is made clinically. It can be confirmed if a delayed weal occurs after a standardised pressure stimulus. This is often painful. In immediate pressure urticaria, a weal will appear within minutes of the stimulus.
A blood count may show an increased white cell count and ESR, but it is often normal.
A skin biopsy of delayed pressure urticaria shows inflammatory infiltrates which vary with the age of the weal. No vasculitis is found.
The results of treatment of pressure urticaria are relatively disappointing.