What are systemic mycoses?
Systemic mycoses are fungal infections affecting internal organs. In the right circumstances the fungi enter the body via the lungs, through the gut, paranasal sinuses or skin. The fungi can then spread via the bloodstream to multiple organs including the skin, often causing multiple organs to fail and eventually resulting in the death of the patient.
What causes systemic mycoses?
Patients who are immunocompromised are more predisposed to systemic mycoses, but they can develop in otherwise healthy patients. Systemic mycoses can be split between two main varieties, endemic respiratory infections and opportunistic infections.
Endemic respiratory infections
Fungi that can cause systemic infection in people with normal immune function as well as those who are immune-compromised, include:
- Histoplasma capsulatum (causing histoplasmosis)
- Coccidioides immitis (causing coccidioidomycosis)
- Blastomyces dermatitidis (causing blastomycosis)
- Paracoccidioides brasiliensis (causing paracoccidioidomycosis)
- Talaromyces marneffei (causing talaromycosis)
These fungi are found in soil and wood debris. Histoplasma is prevalent in Southern USA, Central America, South America, Africa and Asia. Coccidioides and Paracoccidioides are prevalent in Southern USA and Central America. Blastomyces is most often found in North America. Talaromyces marneffei (formerly known as Penicillium marneffei) is endemic in tropical Southeast Asia.
Opportunistic infections
Fungi that only result in systemic infection in immunocompromised or sick people include:
- Candida species including non-albicans candida (causing candidiasis)
- Aspergillus species (causing aspergillosis)
- Cryptococcus (causing cryptococcosis)
- Zygomycetes (causing zygomycosis).
These fungi are found in or on normal skin, decaying vegetable matter, and bird droppings respectively, but not exclusively. They are present throughout the world.
Who is at risk of systemic mycoses?
Immune compromised people are at risk of systemic mycoses. Immunodeficiency can result from:
- Human immunodeficiency virus (HIV) infection
- Systemic malignancy (cancer)
- Neutropenia (low white blood cell count)
- Organ transplant recipients and following haematological stem cell transplant
- After a major surgical operation
- Poorly controlled diabetes mellitus
- Adult-onset immunodeficiency syndrome
- Very old or very young.
What are the clinical features of systemic mycoses?
The clinical features of a systemic mycosis depend on the specific infection and which organs have been affected. Infections in people with normal immune function may result in very minor symptoms or none at all (this is called subclinical infection). General symptoms of illness may include:
- Fever
- Cough
- Loss of appetite.
Lungs
Invasive lung mycoses typically result in a progressive dry cough, shortness of breath, pain when taking a deep breath and fever. These symptoms may progress to the point of life-threatening acute respiratory distress syndrome. Haemoptysis (the coughing up of blood) is also sometimes seen, particularly if any inflammation of the large airways is present.
Bone
Bone infection can develop from spread through the blood or rarely via direct spread from an overlying ulcer and infected skin. Fever and pain in the affected bone are cardinal symptoms. This would usually be investigated with x-rays, computed tomography (CT) scanning and an aspiration via a needle to obtain a specimen for culture.
Brain
Brain involvement by systemic mycoses has a particularly high mortality. Symptoms suggesting the involvement of the brain include headaches, seizures and deficits in normal brain control over movement or sensation. These are assessed by CT or magnetic resonance imaging (MRI) brain scans and if suggestive, then may be followed up by biopsy of the brain.
Meningitis
Inflammation of the tissue surrounding the brain can develop, particularly with candidiasis and cryptococcosis. Symptoms usually include headache, stiff neck and irritability.
Eyes
Almost any of the eye structures may be infected by mycoses. Candida spp. and Cryptococcus spp. are the most commonly infecting mycoses. The symptoms depend on which part of the eye is infected but may include visual blurring, dark or black images floating in the visual field, pain and a red eye.
Skin
A variety of skin changes may be seen in association with systemic mycoses. The skin lesions depend partly on which fungus is the cause.
| Infection | Clinical features |
|---|---|
| Candidiasis |
|
| Aspergillosis |
|
| Cryptococcosis |
|
| Blastomycosis |
|
| Histoplasmosis |
|
| Coccidioidomycosis |
|
| Talaromycosis |
|
| Zycomycosis |
|
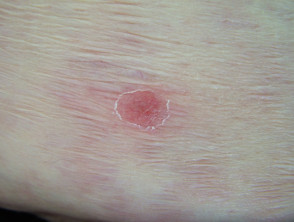
Aspergillus skin lesion
What tests can be done to diagnose systemic mycoses?
The most reliable tests to confirm infection are skin biopsy for histological (microscopic) analysis and fungal culture. Blood can also be cultured.
What treatment is available for systemic mycoses?
Once a diagnosis of systemic mycoses has been established the immune compromise should be reversed if possible, for example by discontinuing immune-suppressing medications or at least reducing their dose.
Systemic antifungal medications can also be given. Suitable drugs include:
- Amphotericin B
- Fluconazole
- Itraconazole
- Voriconazole
- Caspofungin
The prognosis depends on the patient’s immune function and the extent of infection when treatment is started. Despite treatment, many patients die of their infection.