Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Kevin Zheng, Medical Student, University of Auckland, New Zealand; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, August 2015.
Introduction
Demographics
Embryogenesis
Clinical features
Diagnosis
Treatment
A supernumerary nipple is a minor malformation of mammary tissue resulting in extra nipple(s) and/or associated tissue. It is also known as accessory nipple, third nipple, ectopic nipple, or extra nipple.
A supernumerary nipple is distinct from:
Supernumerary nipples are congenital, and usually harmless. However, they are influenced by hormones and susceptible to other disease processes.
Supernumerary nipples or breasts are found in up to 6% of the population. They present as either isolated findings or as features of genetic syndromes. These include:
There have been some reports of an increased risk of urinary tract abnormalities in patients with supernumerary nipples, although this is disputed.
Most isolated cases of supernumerary nipples are sporadic, however they are familial in approximately 6% of reported cases. They exhibit an autosomal dominant pattern of inheritance with incomplete penetrance.
Supernumerary nipple is formed early on in the development of the embryo.
Mammary ridges form from thickening strips of ectoderm—these are the “milk lines” that extend from the axilla to the groin.
Mammary buds develop from downgrowth of epidermis from the ridges.
Failure of regression of mammary ridges result in the formation of the supernumerary nipple.
Supernumerary nipples usually occur anywhere along the two vertical milk lines that originate in the axilla, descend through the region where nipples are typically situated, and terminate at the groin. About 5% of supernumerary nipples form outside the milk lines on the skin of the neck, back, vulva or thigh.
A supernumerary nipple is present at birth. It often appears similar to a congenital organoid or melanocytic naevus. Most supernumerary nipples are much smaller than the normal areola and nipple. They may be solitary or multiple, arising on one or both nipple line(s).
They may be pink or brown, and at least the central nipple is elevated off the skin surface. There may be a central dimple. Supernumerary nipples may develop prominent hair at puberty.
If the supernumerary nipple contains glandular tissue, it can enlarge during puberty, swell and become tender premenstrually, and undergo lactation.
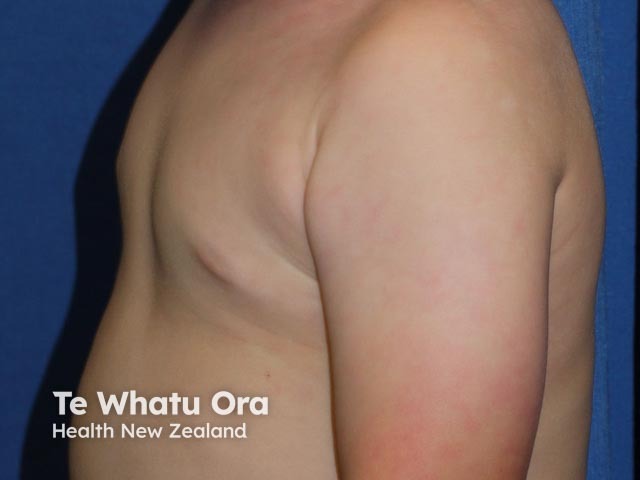
supernumerary nipple

supernumerary nipple 11 s

supernumerary nipple

supernumerary nipple
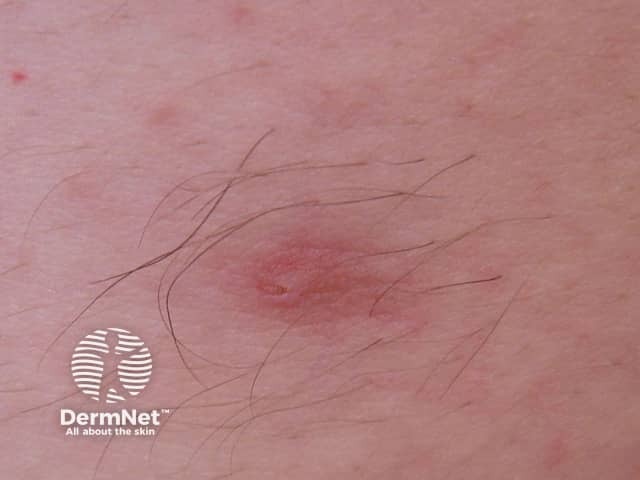
supernumerary nipple
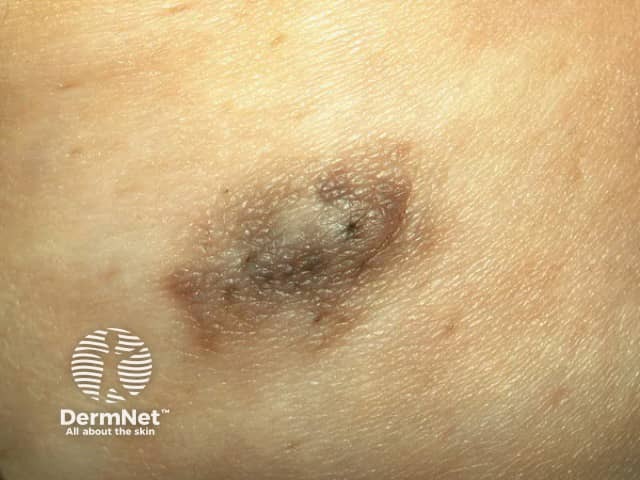
supernumerary nipple
See more images of supernumerary nipple ...
A clinical classification tool is the Kajava supernumerary nipple classification (1915).
Histology provides definitive diagnosis, as it resembles the normal nipple:
Usually no treatment is required. Surgical removal can be considered for cosmetic purposes or if there is discomfort from lactation or tenderness.
Supernumerary nipples can undergo similar diseases to normal breast tissue. There are reported cases of supernumerary nipples developing: