Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Bob Chan, Dermatology Registrar, Christchurch, New Zealand.
Introduction
Sweat gland naevus
Syringoma
Poroma
Hidradenoma
Hydrocystoma
Tubular forms of sweat gland adenoma
Spiradenoma
Cylindroma
Papillary adenocarcinoma
Apocrine adenocarcinoma
Sweat gland lesions originate from sweat gland or sweat duct cell lines. They are not often identified clinically before a biopsy. They are classified by their histological features.
There are two types of sweat glands: eccrine glands and apocrine glands. Eccrine and apocrine glands, hair follicles, and sebaceous glands (which produce sebum) are often referred to as epidermal adnexal structures.
Sweat gland lesions generally have variable apocrine or eccrine differentiation. Traditionally these lesions have been categorized under either the apocrine or eccrine groups, but significant overlaps do exist.
Eccrine glands play an important role in the regulation of body temperature. They are distributed over the entire body skin but are highest in density on the palms and soles. Eccrine glands secrete a salty solution, which reaches the skin pores via an eccrine duct.
Eccrine sweat is a sterile electrolyte solution primarily containing sodium chloride, potassium and bicarbonate, with smaller quantities of various other components such as glucose and antimicrobial peptides. Sweat rate differs depending on the site on the body, the degree of thermal or physical stress, and between individuals. Under maximal stimulation, the body can produce 3 litres of eccrine sweat per hour.
In contrast, apocrine glands produce an oily fluid rich in triglycerides and fatty acids – subsequent colonisation by anaerobic bacteria results in body odour.
Eccrine and apocrine naevi are rare malformations of the glandular component of an eccrine or apocrine gland. The glands within a sweat gland naevus are increased in size and number from birth. Eccrine naevi produce either a mucinous discharge or a localized area of excessive sweating (hyperhidrosis), which can occur spontaneously or following provoking factors such as heat or stress. Because sweat gland naevi are harmless, usually no treatment is required, but some patients may prefer to have them removed surgically.
A rare naevus called porokeratotic eccrine ostial and dermal duct naevus is categorised within epidermal naevi.

Sweat gland naevus
Link to sweat gland naevus video.
Syringomas are benign adnexal growths with ductal (syringeal) differentiation, from either eccrine or apocrine lineage. Eccrine syringomas appear as crops of small, firm, skin coloured papules (bumps). They are most commonly found around the eyes and on the eyelids, but they can occur on other sites.
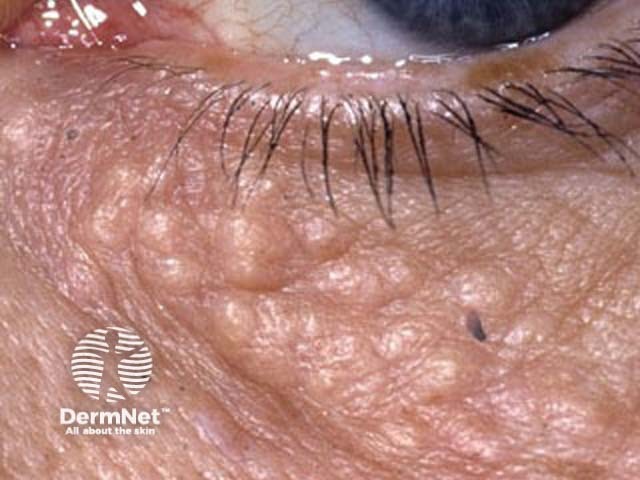
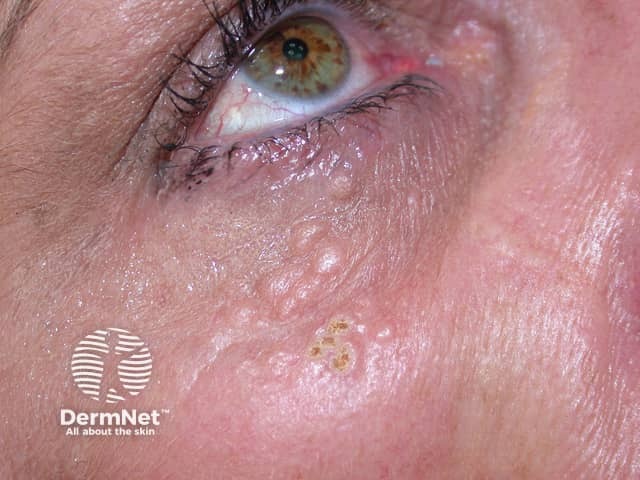
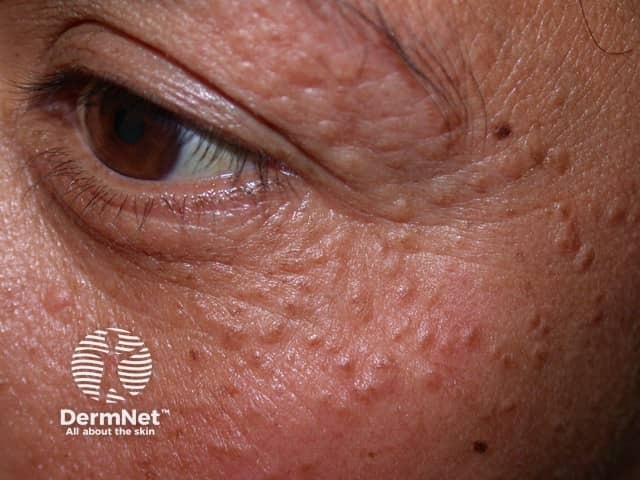
Syringomas are more commonly found in the Asian population, and there is an association with Down syndrome. Some are familial but the causative gene is not known.
Findings on skin biopsy are characteristic, with a well-circumscribed proliferation of epithelial tubules, nests, and cords embedded in a dense fibrous stroma, found in the upper half of the dermis.
Because they are deep in the skin, it is difficult to remove syringomas without causing scarring. Treatment options include cryotherapy, electrosurgical destruction, laser ablation, and surgical excision.
Poromas are a group of benign growths of poroid differentiation, i.e. derived from cells of the terminal duct and connected to the epidermis. They can be of either eccrine or apocrine lineage. They may present as papules (bumps), plaques (thickened patches like seborrhoeic keratoses), or nodules (lumps). Names used to describe poromas include:
Poromas usually have a reddish colour due to prominent underlying blood vessels and may resemble pyogenic granuloma. They may also appear darker than surrounding skin.
Poromas may arise on any skin surface but those with eccrine differentiation are most commonly found on the palms, soles and scalp. When multiple, they are sometimes described as poromatosis.
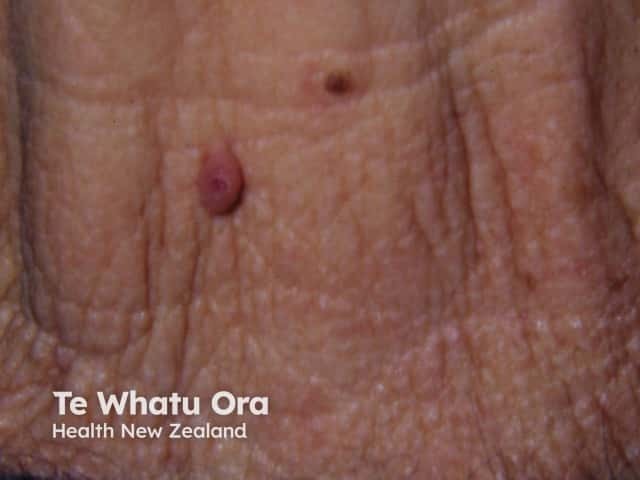
Eccrine poroma
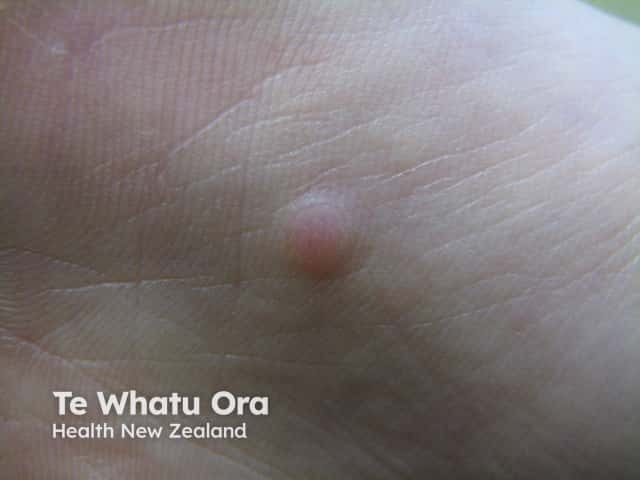
Eccrine poroma
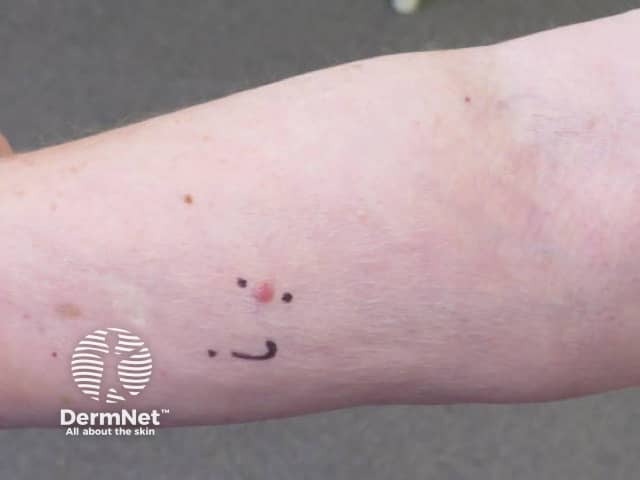
Eccrine poroma
See more images of eccrine poroma.
Skin biopsy of poroma shows the growth of terminal duct cells. The report may describe a circumscribed proliferation of compact cuboidal keratinocytes with small monomorphous nuclei and scant eosinophilic cytoplasm. The narrow ducts are often lined by a row of cuboidal cells. Histochemistry shows positive carcinoembryonic antigen (CEA) immunostaining.
Poromas are usually removed by surgical excision and electrosurgical destruction.
Hidradenoma or acrospiroma is a benign dermal growth closely related to poroma except without connection to the epidermis. Hidroacanthoma can also be of apocrine or eccrine origin. It appears as a solitary nodule (lump) or cyst (when it is called cystic hidradenoma) and may appear on any site. Hidradenoma may be solid or produce a watery discharge. Complete surgical excision is curative.
Poroid hidradenoma refers to a hybrid lesion with features of hidradenoma and poroma.
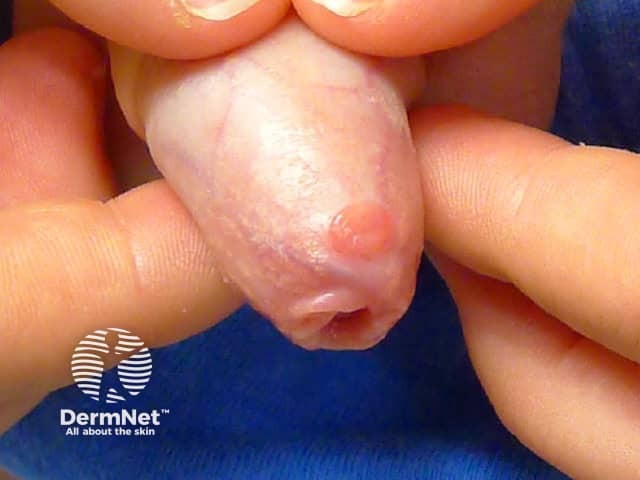
Cystic hidradenoma
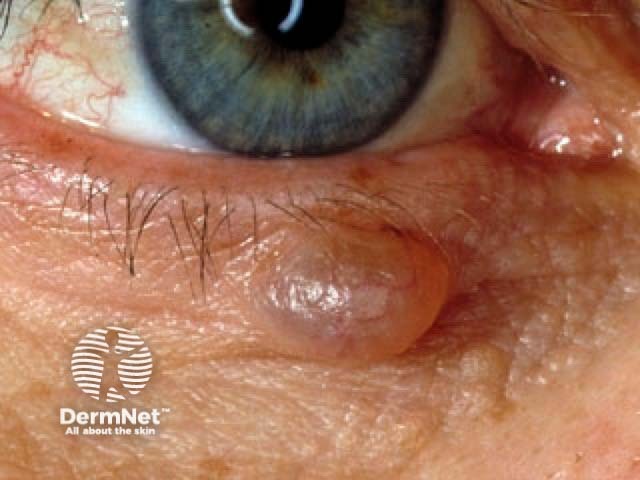
Hidrocystoma of the eyelid
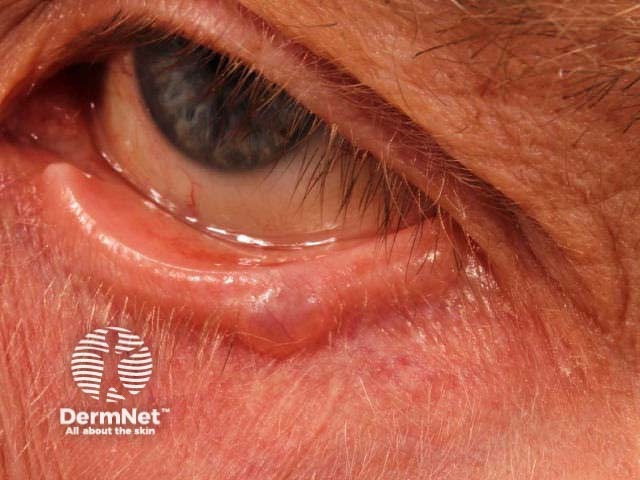
Hidrocystoma of the eyelid
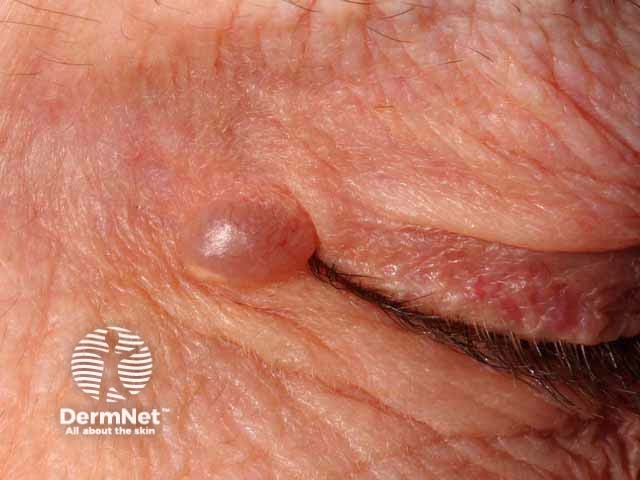
Hidrocystoma of the eyelid
Some eccrine/apocrine tumours have glandular differentiation. They present as papules, plaques or nodules and are diagnosed on biopsy. There are often combinations of histological patterns.
Historically spiradenomas have been designated under the eccrine lineage, but are now thought to be more closely related to the apocrine lineage, because:
Spiradenomas present as nodules, and are usually painful. They are usually found over the head, neck and trunk. There is an association with cylindromas, and a genetic condition (Brooke-Spiegler syndrome) results in multiple spiradenomas, cylindromas, and trichoblastomas.
Spiradenomas are harmless but may be treated with conservative excision.
Cylindromas are undifferentiated tumours of apocrine origin. They may be solitary or multiple and most often arise on the scalp. Turban tumours are multiple cylindromas.
Under the microscope, cylindroma has islands of cells fitting together like a jigsaw.
Cylindromas are usually excised.
Papillary adenocarcinomas are uncommon skin cancers derived from eccrine tissue. They are typically found on the fingers, palms, toes or soles. They present as a slowly growing, solitary nodule and can measure up to several centimetres in size. Variants of these lesions were previously called papillary adenoma or tubulopapillary carcinoma.
Papillary adenocarcinoma is aggressive and may erode underlying bone, or metastasize to other sites of the body.
Treatment involves surgical excision of the entire lesion.
Cancers derived from apocrine tissue are often described as adnexal carcinomas. Variants include:
Apocrine adenocarcinoma may develop within recognisable benign tumours allowing classification as follows.
Characteristically, these cancers present as rapidly growing nodules within a longstanding, previously stable lesion. They may ulcerate or bleed. They should be widely excised. Metastasis is uncommon.