Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Mark Duffill, Dermatologist, Hamilton, New Zealand, 2008; revised Hon A/Prof Amanda Oakley Chief Editor, 2015; Updated by: Dr Ayesha Vos, Junior Medical Officer, Eastern Health, Melbourne, Victoria, Australia; A/Prof Rosemary Nixon AM, Dermatologist, The Skin Institute, Carlton, Victoria, Australia. Copy edited by Gus Mitchell. January 2021.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Appendix: What drugs are reported to cause symmetrical drug-related intertriginous and flexural exanthema?
Symmetrical drug-related intertriginous and flexural exanthema (SDRIFE) is an adverse drug eruption presenting as a distinctive erythematous rash involving the skin folds. It was initially called ‘baboon syndrome’ as the buttocks were predominantly affected in the first patients described with this reaction, although this may be an unrelated entity caused by sensitisation to a topical agent followed by systemic exposure.
Symmetrical drug-related intertriginous and flexural exanthema can affect all age groups, but is rare in children. SDRIFE shows a male predominance of 3:1.
Symmetrical drug-related intertriginous and flexural exanthema is a type IV delayed hypersensitivity reaction to a systemic drug [see Allergies explained]. The reason for the characteristic distribution of the rash is not known.
Amoxicillin and other beta-lactam antibiotics (penicillins, cephalosporins) are the most common cause of SDRIFE, accounting for approximately 50% of cases. A detailed list of medications reported in association with SDRIFE is found in the appendix.
Symmetrical drug-related intertriginous and flexural exanthema appears hours to days after exposure to the medication. The rash presents as a well-defined redness of the buttocks, natal cleft, and/or upper inner thighs, resembling the red bottom of baboons. The redness is usually symmetrical and often forms a V-shape. The neck, axillae, and other large skin folds (flexures) may also be involved.
Rare clinical features include pustules, vesicles/bullae, petechiae/purpura, and oral mucosal lesions.
A key feature is the lack of systemic symptoms. The affected person is not unwell and the rash is not accompanied by any other symptoms.

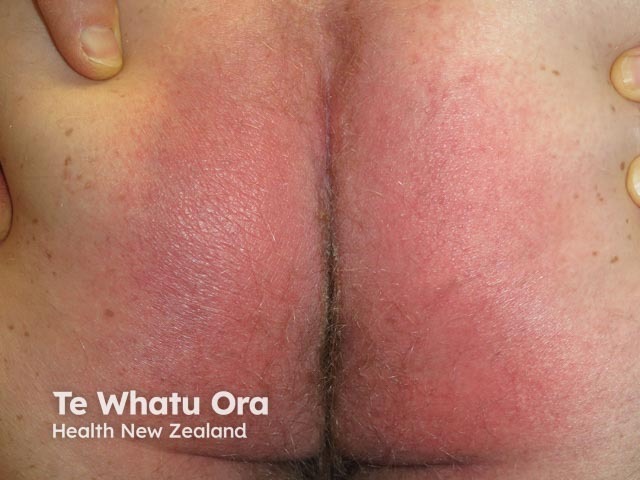
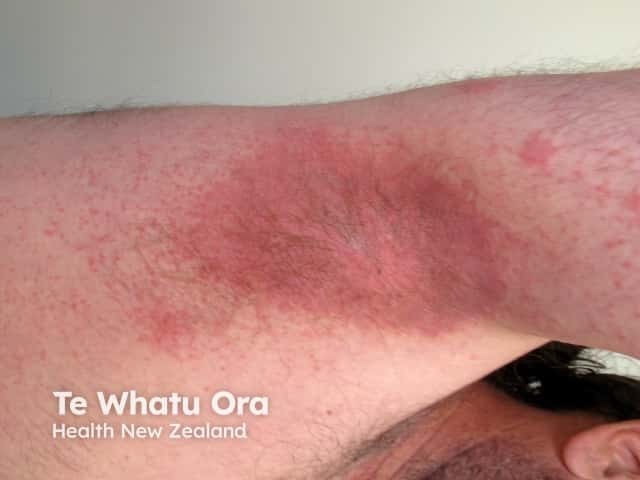
SDRIFE
Symmetrical drug-related intertriginous and flexural exanthema has not been reported to be associated with any complications.
Symmetrical drug-related intertriginous and flexural exanthema is usually a clinical diagnosis with the following suggested diagnostic criteria:
Skin biopsy shows nonspecific inflammation consisting of a superficial perivascular mononuclear cell infiltrate.
Patch tests applied to a previously affected area several weeks after recovery may show a positive reaction to the causative agent in 50% of cases. An oral challenge with the suspected drug (drug provocation test) will trigger the same skin reaction in the majority of cases.
Differential diagnoses for symmetrical drug-related intertriginous and flexural exanthema can include:
Treatment of symmetrical drug-related intertriginous and flexural exanthema requires the cessation of the suspected drug. Topical steroids may hasten resolution of the erythema.
Symmetrical drug-related intertriginous and flexural exanthema is a benign self-limited reaction that resolves when the offending drug is withdrawn. However, it will usually recur on re-exposure to the causative drug.
Alphabetical listing of agents reported to trigger SDRIFE (note this list may not be complete)