Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Arcana Luo, Medical Student, University of Auckland, New Zealand; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, March 2014.
Introduction Causes Associated skin conditions Triggers Diagnosis Clinical features Non-cutaneous Koebner phenomenon Associated phenomena Koebner phenomenon in psoriasis Prevention Treatment
The Koebner phenomenon describes the appearance of new skin lesions of a pre-existing dermatosis on areas of cutaneous injury in otherwise healthy skin. It is also known as the Köbner phenomenon and isomorphic response.
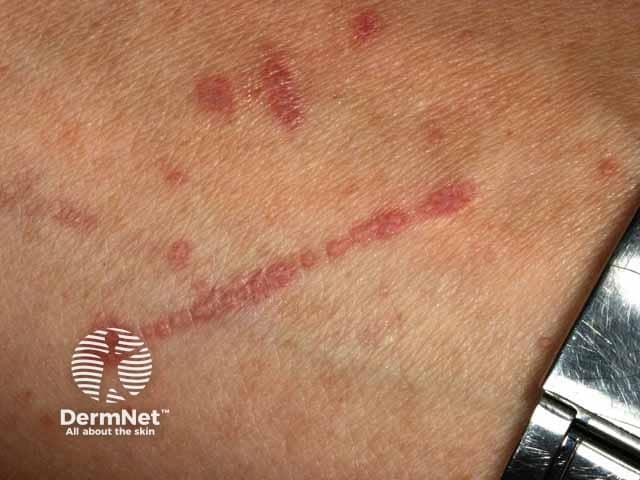
Linear lesions due to Koebner phenomenon in lichen planus
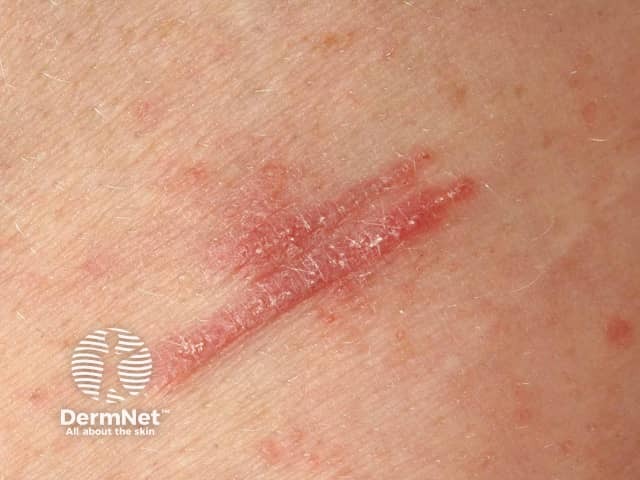
Linear lesions due to Koebner phenomenon in lichen planus
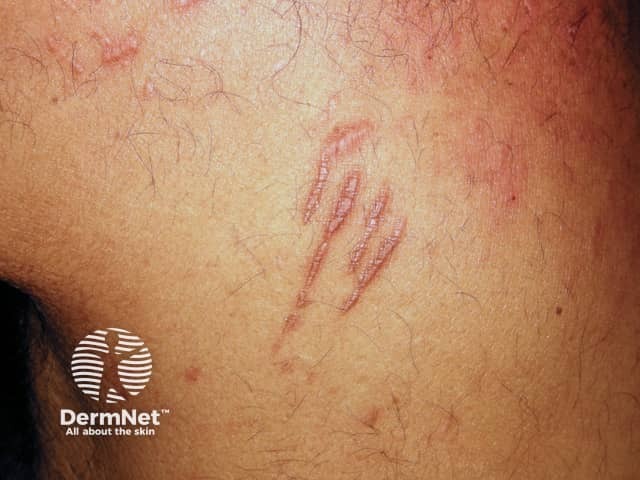
Linear lesions due to Koebner phenomenon in lichen planus
The cause of the Koebner phenomenon is unclear. Current theories suggest the Koebner phenomenon requires both epidermis and dermis to be injured at the same site. The production of inflammatory substances and neuropeptides has been postulated as a non-specific first step, triggering a secondary disease-specific process. The role of chemical messengers such as nerve growth factor (NGF) may be important.
Skin conditions that regularly manifest Koebner phenomenon are psoriasis, vitiligo and lichen planus. There have been reports of possible Koebner phenomenon in many other conditions.
A true Koebner response occurs in:
A pseudo-Koebner response occurs with infections arising in an area of trauma, but represent transfer of virus into the damaged skin:
Localised trauma can also lead to:
A variety of skin injuries have been found to trigger the Koebner phenomenon.
Trauma
Chemical irritation
Diseases/medical conditions
Other
The Koebner phenomenon is diagnosed clinically. The characteristic lesions:
Lesions may form in patients with or without pre-existing skin conditions. A true Koebner response can be confirmed by experimentally reproducing lesions with different methods of injury. However, this may not always work and is not usually practical or desirable.
Koebner phenomenon lesions are typically linear in shape as they follow the route of cutaneous injury. Aside from linear skin injury, linear lesions arising from the Koebner phenomenon can also be seen in mosaic skin disorders (eg, segmental lichen planus).
Patients differ in terms of how intensely they respond to skin injury.
Patients who develop the Koebner phenomenon in response to one method of injury are susceptible to other triggering stimuli. This is particularly noted in patients with psoriasis. Conversely, a patient who does not develop skin lesions with one type of injury is not expected to exhibit the Koebner phenomenon with another type of injury.
The time from injury to the formation of a skin lesion depends on the specific skin disease. For psoriatic plaques, it is between 10 to 20 days, with a range from 3 days to 2 years. The time to lesion formation can differ in the same patient.
Some reports suggest the Koebner phenomenon may affect other surfaces apart from the skin, such as the oral mucosa, or cause lesions in internal organs, such as the lungs after damage from chronic infection. Cutaneous lesions due to Koebner phenomenon have been reported in sarcoidosis and systemic lupus erythematosus.
Other phenomena in relation to skin trauma or inflammation are distinct from the Koebner phenomenon.
Psoriasis is the best studied condition that exhibits the Koebner phenomenon and can be used to aid diagnosis.
Koebner phenomenon has been noted to be particularly prevalent in:
Other studies indicate that the Koebner phenomenon:
Plaques due to the Koebner phenomenon can appear on any area of the body, even those not usually involved by psoriasis.
In recalcitrant psoriasis, a concurrent skin condition such as contact dermatitis may drive the disease via the Koebner phenomenon.
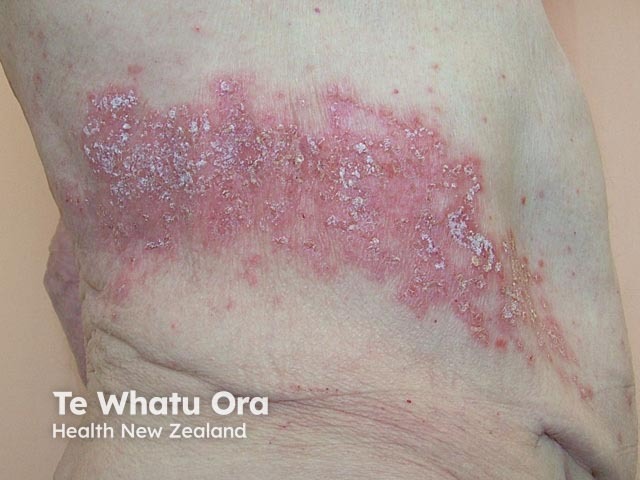
Shingles (herpes zoster)
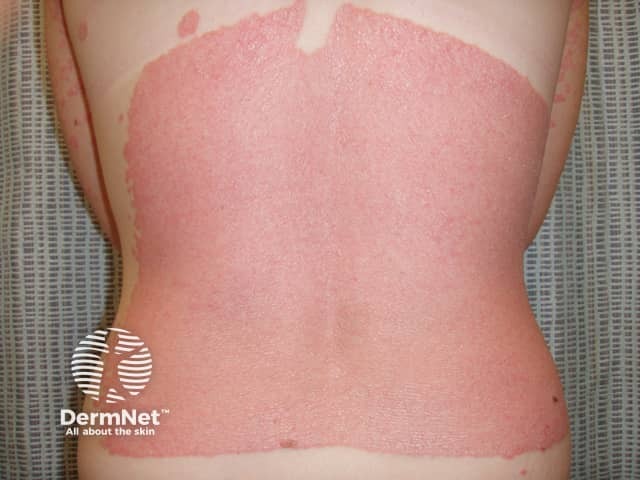
Sunburn
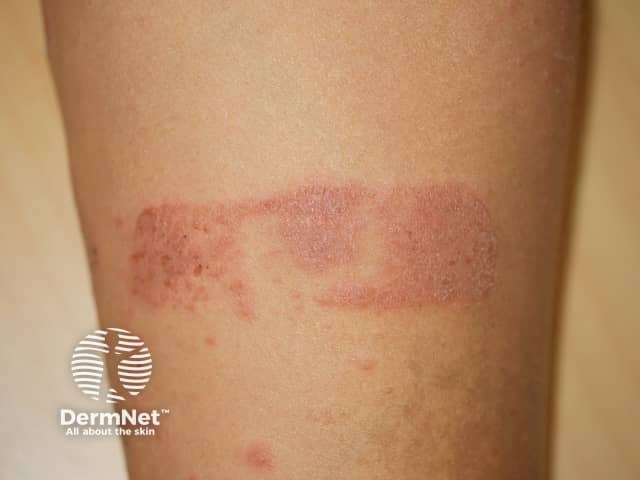
Contact dermatitis to adhesive plaster
Although it is not possible to prevent all cutaneous injury, if you are susceptible to the Koebner phenomenon, take care to avoid:
The following have been reported to prevent the Koebner phenomenon:
Treatment for the cutaneous lesions arising from the Koebner phenomenon depends on the associated skin condition.