Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Vanessa Ngan, Staff Writer, 2005; Updated: Dr Aswan Tai, Peter MacCallum Cancer Centre, Melbourne, Australia; Dr Sarah Smithson, Dermatologist, Skin Health Institute, Melbourne, Australia. Copy edited by Gus Mitchell. April 2022
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Kyrle disease is characterised by transepidermal elimination of keratin from the dermis through the epidermis onto the skin surface. It is a subtype of primary perforating dermatosis along with reactive perforating collagenosis, perforating folliculitis, and elastosis perforans serpiginosa.
Kyrle disease was first described in 1916 by Austrian dermatologist and pathologist Josef Kyrle as “hyperkeratosis follicularis et parafollicularis in cutem penetrams” in a diabetic female patient with generalised hyperkeratotic papules.
There is longstanding controversy surrounding the classification of Kyrle disease, with some clinicians believing it to be a distinct clinical entity and others considering it as within the reactive perforating collagenosis spectrum.
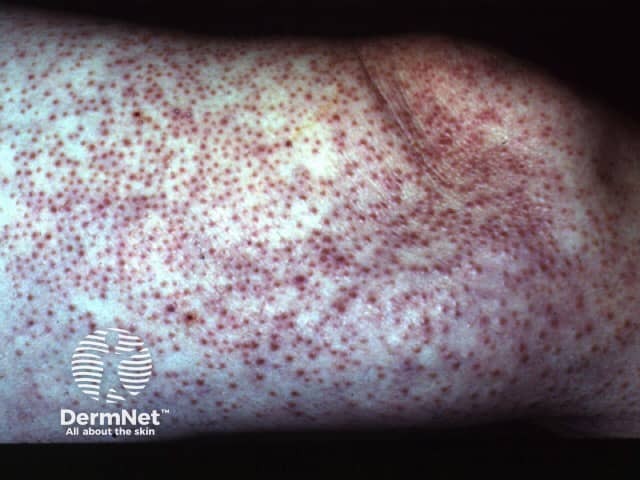
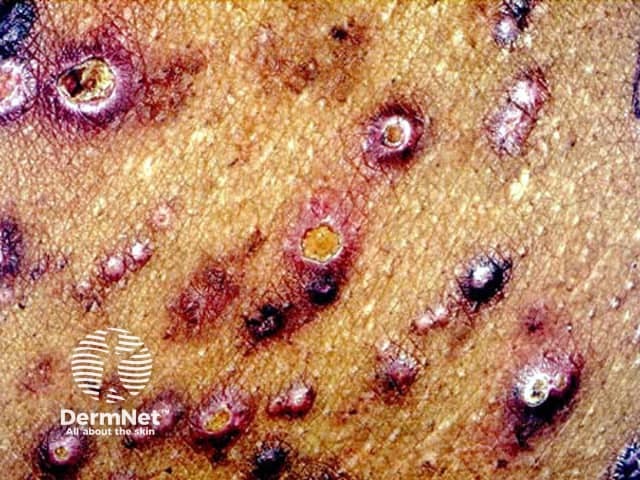
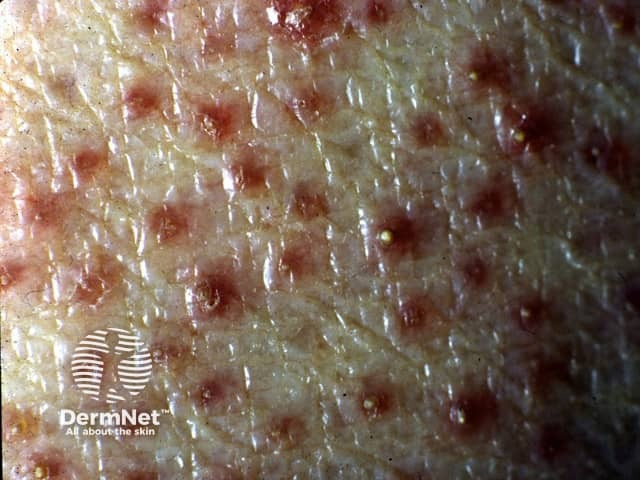
The pathogenesis of Kyrle disease (KD) is unclear.
Kyrle disease is a papulonodular mucocutaneous disorder.
Kyrle disease can usually be diagnosed on its distinct clinical features, associated conditions, and confirmed on skin biopsy with histopathology showing incomplete keratinisation and a hyperkeratotic, parakeratotic plug.
The main aim of treatment is to control itch and avoid superficial trauma. Rapid improvement and resolution of lesions are often seen once any associated underlying disease is managed.
Lesions are self-healing but often recur. Individuals can develop larger and more lesions with age.