Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Marie Hartley, Staff Writer, 2009. Updated by Vanessa Ngan, Staff writer, 1 February 2014.
Introduction
Clinical features
Early skin manifestations
Late skin manifestations
Diagnosis
Treatment
Prevention
Ticks are blood-sucking parasites. When they take a blood meal, they can cause dermatologic disease directly by their bite, or indirectly as vectors of other diseases. Tick-borne diseases include:
This page will focus on skin diseases that occur as a direct result of tick bites. Risk factors for tick exposure include outdoor activities such as camping, hiking, walking in long grass, or contact with animals. In endemic areas, infections can also be acquired during routine activities. Many cases of the tick-borne disease occur in the summer months when ticks are most active.



While tick bites can be painful, in many cases they can go unnoticed. Once the tick is full from its blood meal it falls off the skin.
Ticks can be categorised as either hard or soft ticks and this distinction determines some of the clinical features of the tick bite. Hard ticks feed for a few days to several weeks, while soft ticks feed quickly and leave their host rapidly.
Ticks cause acute and chronic skin diseases through physical trauma, salivary secretions, toxins, excretions, body parts, or by causing a host to scratch. Skin disease may occur away from the site of the bite, and tick bites can also cause disease in other parts of the body such as 'flu-like symptoms, vomiting, paralysis and even anaphylaxis.

Tick bite
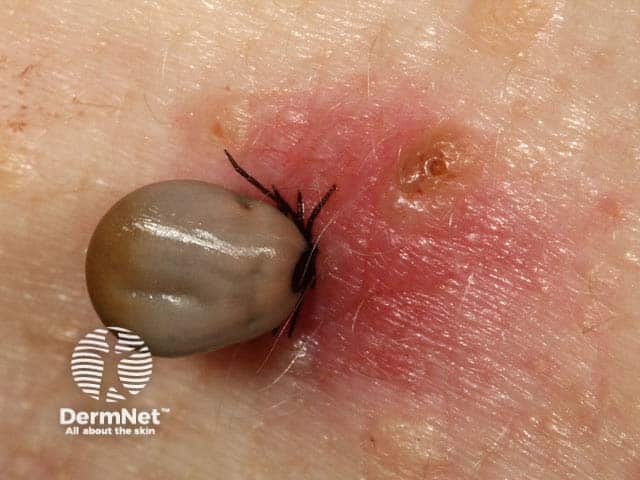
Tick bite

Tick bite
For both hard and soft tick bites, 0.5–2 cm red areas, papules (small bumps), or thin plaques may form at the site of attachment within 1 to 3 days. The lesion may feel hard and may be surrounded by redness. Mild swelling or blister formation can occur. The bite can be mild to severely itchy.
Necrotic (dead tissue) ulcers can form in severe cases; usually due to bites from soft ticks. Bites from soft ticks may be painful.
Specific tick species can also cause characteristic lesions such as bruising (purpura), urticaria, and ulceration.
Acute skin lesions can persist and become papules, nodules (larger solid lumps), or plaques. Over days to months, these lesions can form a tick bite granuloma; a 0.5 to 2 cm nodule made up of mixed inflammatory cells.
Tick bites can also rarely result in hair loss (alopecia), which may resolve within 1 to 3 months, or be permanent.
Tick bites can develop wound infection due to secondary infection by bacteria such as Staphylococcus aureus and Group A Streptococcus. Retained tick material and host scratching may increase the likelihood of this complication.
Diagnosis can be difficult, especially if the bite has gone unnoticed. Microscopic examination of skin biopsy specimens may assist diagnosis. Sometimes if a tick is still attached, it can be removed and identified. Additional tests may be done according to the tick identified and whether or not it is a vector for certain diseases.
Itch resulting from a tick bite may be relieved with topical steroids and oral antihistamines. Tick bite granulomas can be surgically removed.
Ticks still attached to the skin should be physically removed. Equipment necessary for tick removal includes gloves, isopropyl alcohol or other skin disinfectant, and fine-toothed forceps. The patient should be comfortably positioned so that the doctor can easily access the tick.
While wearing protective gloves, gently grasp the tick with tweezers as close as possible to the skin and slowly, gently pull it upwards and away. Do not twist or jerk the tick as this may cause the tick mouthparts to break off and remain in the skin. Also, do not squeeze or puncture the body of the tick as this may contain infectious organisms that cause disease.