Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: July, 2023
Author(s): Dr Hyun Kyoung Lee, Medical Registrar; and Dr Louise Reiche, Dermatologist, Palmerston North, New Zealand (2023); Minor update Jan 2025.
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Prevention
Outcome
Topical corticosteroid withdrawal is a rare rebound reaction in patients with topical steroid overuse that occurs after discontinuation.
This is usually caused by prolonged use of moderate to high strength topical corticosteroids. Withdrawal may present with skin burning, itching, redness, scaling, swelling, papules, or pustules.
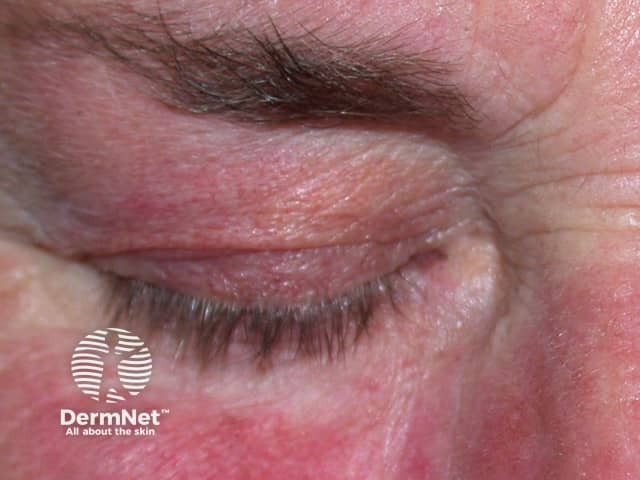
Redness and swelling of the lids - steroid withdrawal after prolonged potent steroid use on the face.

Redness and swelling of the forearm after abrupt discontinuation of prolonged potent topical steroid use. Palms are not affected (red sleeve sign).
The prevalence of topical corticosteroid withdrawal reactions is unknown.
Major risk factors for topical steroid withdrawal include:
The following mechanisms may explain the pathogenesis of topical steroid withdrawal:
Prior to stopping the steroid, the skin often appears normal or near-normal, although patients with atopic dermatitis may have itching or prurigo-like nodules. The onset of withdrawal from the time of discontinuation ranges from 48 hours to over 3 months.
Withdrawal typically occurs in four stages.
Symptoms:
Cutaneous features:
Darker or grey skin changes, rather than redness, may feature in more pigmented skin types.
There is a lack of consensus on diagnostic criteria for topical corticosteroid withdrawal however, in recent literature, the key features are:
One of the challenges is determining whether the skin reaction observed is due to the stopping of topical corticosteroids, or a worsening of the underlying skin disease for which the steroids were prescribed.
Patch testing can be useful in excluding contact dermatitis to the topical corticosteroid or cream excipients, or other topical agents (eg, emollients), although this may be difficult if there are insufficient areas of normal skin.
Histology is not useful in the diagnosis of topical corticosteroid withdrawal due to its non-specific histological features of epidermal atrophy, spongiosis, and parakeratosis.
Many different treatments are available, however they are not associated with a reduced time to resolution.
Concerns about the risk of topical corticosteroid withdrawal should not prevent adequate treatment of atopic dermatitis and other skin conditions, as far more people respond to appropriate topical steroid use than develop withdrawal.
There are currently no specific treatments that clearly reduce the time to resolution, which can range from 72 hours to months, with the majority (77%) recovering after 3 months.
Topical corticosteroid withdrawal can have a prolonged course of up to 5 years after cessation in a small minority of patients.