What is atopic dermatitis and how is it treated?
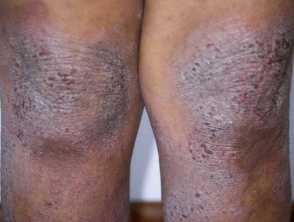
Atopic dermatitis (atopic eczema), the most common inflammatory skin disease worldwide, involves genetic and environmental factors. It is not yet possible to modify genetic factors and it can be difficult to effectively manipulate all relevant environmental factors. There is therefore no known cure for atopic dermatitis, however, treatment can control inflammatory dermatitis and help the skin feel healthy:
- General measures
- Topical treatments
- Systemic treatments.
Atopic dermatitis
What general measures help atopic dermatitis?
- Education: Understanding the disorder and being fully informed by healthcare providers is important. Effective education facilitates effective treatment.
- Skin irritants: Where possible, avoid triggers that can directly inflame the skin. These may include fabrics, chemicals, humidity, and dryness. See: Barrier function in atopic dermatitis.
- Food: The relationship between atopic dermatitis and food is complex. Food allergies may exacerbate atopic dermatitis, but avoidance diets do not cure the problem. Avoidance may exacerbate atopic dermatitis. Food allergy testing is needed if there is concern of an immediate life-threatening reaction (anaphylaxis). See: Causes of atopic dermatitis for more information.
- Psychological support: The psychological effects of atopic dermatitis are considerable, for both the sufferer and the carer. Counselling and cognitive behavioural therapy can be beneficial.
What topical treatments help atopic dermatitis?
Topical treatments can come in many forms. It is important that the correct formulation is used for the different patterns and distributions of atopic dermatitis.
- Lotion: Smooth liquid. These are not greasy and cosmetically leave little or no residue. When applied to broken skin they can be very painful.
- Gel: Semi-liquid and often clear.
- Foam: Bubbles within a liquid.
- Cream: Oil-in-water mix. Smooth and easy to spread especially on moist skin.
- Ointment: Water-in-oil mix. Greasy and more difficult to spread but better for dry skin than creams.
Treatments
Over-the-counter topical treatments for atopic dermatitis
Emollients and moisturisers
- Emollients and moisturisers are an essential aspect of care for all types of dermatitis.
- They need to be continued long-term in atopic dermatitis even if the skin looks and feels comfortable. They should be applied regularly (2-3 times/day is recommended) and liberally.
- Dry skin (xerosis), a common feature of eczema, is highly responsive to treatment with moisturisers; and moisturiser use has been associated with reduced frequency of flares and reduced use of topical corticosteroids.
- Adults with extensive atopic eczema may need as much as 500g of an emollient cream weekly.
- There are different formulations of moisturisers, including leave-on products (best applied directly after bathing), soap substitutes, and bath additives.
- High oil/low water mixtures are generally recommended for skin hydration and barrier repair; generally, the greasier the better, but patient preference is important.
- Greasy leave-on moisturisers can be uncomfortable under clothing, whereas lighter moisturisers (lotions, for example) stain less and are more comfortable, but may require more frequent application.
- Potential adverse effects and risks of moisturiser use:
- Application can be time-consuming and leave residue on clothes or furniture.
- If paraffin-based moisturisers soak into clothing, this can cause a fire hazard.
- Moisturisers make the skin slippery so take care with emollients in the bath, shower, and when holding babies.
- If contact dermatitis develops in reaction to a particular product, its use should be discontinued.
- Sodium lauryl sulphate (SLS) is a surfactant used to mix the oil and water in moisturisers. It irritates dermatitis when left on for prolonged periods. Products to be left on the skin should be SLS-free, contain only a few ingredients, and ideally avoid other irritants or allergens such as fragrances.
- Wet wraps may be used over moisturisers on areas of red, hot, weepy dermatitis.
Antiseptics
- It is common for patients with atopic dermatitis to have bacteria such as Staphylococcus aureus colonising the skin. Sometimes the skin can become infected by these organisms. Antiseptics can be used during an infection and to try to prevent infection, but with care as they can irritate the skin.
- Common antiseptics used to treat atopic dermatitis include:
- Bleach bath: Add half a cup of household bleach to a full bath.
- Potassium permanganate: Use in a weak concentration (1 in 10,000 dilution) as a wet soak or in a bath. It is useful short-term to help dry weepy, exudative eczema; stop as soon as the exudation is controlled to prevent excessive drying. It can cause permanent staining of ceramic baths and temporary brown staining of nails and skin.
Prescription topical treatments for atopic dermatitis
Coal tar
- Coal tar is a distillate from coal used in a variety of topical preparations including shampoos, lotions, and creams, sometimes mixed with a topical steroid to treat scaly atopic dermatitis. The smell can be off-putting.
Topical steroids
- Topical steroids are the mainstay treatment for mild-to-moderate atopic dermatitis. They are safe and effective when used correctly.
- The strength of a topical steroid is determined by the structure of the molecule. The weakest steroid used for the shortest time to be effective is usually prescribed. The strength of the steroid selected is determined by the skin site and dermatitis severity.
- The fingertip unit is a useful guide to how much cream or ointment to apply.
- Wet wraps can be applied over a topical steroid for acutely inflamed atopic dermatitis.
- Paste bandages can be applied over excoriated or lichenified dermatitis to reduce scratching and enhance the effect of the steroid.
- Steroid impregnated tape has also been used.
- Weekend treatment: When the dermatitis is under control, apply the steroid two days per week to any new or old areas of dermatitis, and then take a break for five days.
- Fear of topical steroids resulting in their inadequate use is a common reason why they do not work.
- A rebound flare may occur if too strong a steroid is used on the incorrect site for the incorrect reason.
Topical calcineurin inhibitors
- Topical calcineurin inhibitors are topical immunomodulators and work in a different way from corticosteroids.
- Pimecrolimus and tacrolimus are suitable for treating atopic dermatitis in sensitive sites such as the eyelids, skin folds, and genital areas.
Crisaborole ointment
- Crisaborole was approved by the FDA in 2016 as a topical treatment for mild-to-moderate atopic dermatitis in patients 2 years of age and older. It works by inhibiting phosphodiesterase 4 (PDE4). See also: Key clinical-trial evidence for crisaborole.
Phototherapy
- Narrowband UVB phototherapy can be used to treat severe atopic dermatitis.
- Treatment involves standing in the cabinet two to five times weekly, so may not be suitable for young children or the infirm who cannot stand unaided.
- Phototherapy is usually combined with the usual topical treatments.
UVB treatment
What systemic treatments help atopic dermatitis?
Antihistamines
- Antihistamines are useful to control dermographism and other forms of urticaria in some patients with atopic dermatitis.
- There is no role for the routine use of non-sedating antihistamines for dermatitis-induced itch; sedating agents may help sleep disturbance that is common in eczema.
Systemic steroids
- A short course of systemic corticosteroids can be very useful to quickly control a flare and to provide temporary respite, especially for important occasions such as a wedding.
Immunosuppressive and anti-inflammatory agents
- Long-term control of severe disease may require an immunosuppressive or anti-inflammatory agent such as:
- These medications take weeks to work and careful monitoring is required.
Biological agents
- Biological agents block specific steps in the inflammatory pathway.
- Dupilumab is the first biological agent approved to treat atopic dermatitis. See also: Key clinical-trial evidence about dupilumab.
Janus kinase inhibitors and other novel small molecules
What new and emerging treatments are there for atopic dermatitis?
Topical agents
- Janus kinase inhibitors eg, ruxolitinib. Ruxolitinib was approved by the United States Food and Drug Administration (FDA) in September 2021 for select use in patients aged 12 and older with mild to moderate atopic dermatitis.
- Phosphodiesterase 4 inhibitors.
Systemic agents
- Biological agents at various stages of research, development, and approval eg, tralokinumab, lebrikizumab, nemolizumab, rituximab, rocatinlimab and amlitelimab.
- Small molecule antagonists.
Treatment of atopic dermatitis in skin of colour
- There is little published data on the treatment of atopic dermatitis in skin of colour, in part due to under-representation in clinical trials.
- Treatments should take into account genetics, skin phototype, and cultural practices.
- The efficacy of systemic treatments may be influenced by gene polymorphisms and enzyme deficiencies affecting drug pharmacokinetics in some ethnic groups.
Treatment for infective complications of atopic dermatitis
- For secondary bacterial infection, skin swabs should be taken to determine the responsible bacteria and their antibiotic sensitivity. Topical antibiotics should not be used as this increases bacterial resistance, a topical antiseptic should be considered instead. Overt superadded Staphylococcal infection (impetiginisation) often merits a short course of an oral antibiotic.
- Superinfection with herpes simplex (eczema herpeticum) can cause rapid and painful deterioration and the development of small blisters followed by crusting over existing dermatitis, requiring antiviral tablets or injections.
- Molluscum contagiosum, and coxsackievirus (eczema coxsackium) may also infect dermatitis, requiring specific treatments.
See also: Complications of atopic dermatitis.
We suggest you refer to your national drug approval agency such as the Australian Therapeutic Goods Administration (TGA), US Food and Drug Administration (FDA), UK Medicines and Healthcare products regulatory agency (MHRA) / emc, and NZ Medsafe, or a national or state-approved formulary eg, the New Zealand Formulary (NZF) and New Zealand Formulary for Children (NZFC) and the British National Formulary (BNF) and British National Formulary for Children (BNFC).