Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Haylee Boyens, Medical Student, University of Auckland, New Zealand; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, December 2014. Latest update by Dr Jannet Gomez, Postgraduate student in Clinical Dermatology, Queen Mary University London, United Kingdom, July 2016.
Introduction
Causes
Demographics
Clinical features
Investigations
Treatment
Prognosis
Gangrene is the localised death of body tissue. Wet gangrene is gangrene due to necrotising bacterial infections, including necrotising fasciitis. Wet gangrene should be distinguished from 'dry' gangrene, which is due to ischaemia.
Necrotising bacterial infections can occur via any break in the skin or internal organ. They are caused by 3 main bacterial subgroups:
Polymicrobial necrotising infections often involve a mix of:
Polymicrobial necrotising infections tend to affect the trunk and perineum.
Patients with these infections usually have a history of other medical problems, especially diabetes, and are likely to be older adults. The initial injury to the skin may have been unnoticed.
Gas gangrene is particularly severe and is most often due to Clostridium perfringens, which can rapidly proliferate in injured muscles. This organism is ubiquitous in soil and dust. Gas gangrene was very prevalent in World War 1, complicating 6% of open fractures and 1% of all open wounds. Clostridia release alpha, beta and other toxins, which induce blood clotting at the site of the infection and result in myonecrosis (death of muscle tissue). Reduced blood flow, localised ischaemia and lowered pH result in a favourable environment for other bacteria to grow. The gas is composed of nitrogen, oxygen, hydrogen, hydrogen sulfide and carbon dioxide. It spreads within the muscle fibres allowing rapid spread of infection.
Group A β-hemolytic streptococci (GAS), either alone or associated with staphylococcal species, tend to be locally aggressive and can lead to serious blood infections such as toxic shock syndrome.
Patients with streptococcal and staphylococcal infections are likely to be younger and in better general health than those with polymicrobial infections. The route of entry usually follows trauma, including surgery and intravenous drug (ab)use. M proteins produced by GAS allow the bacteria to adhere to tissue and evade the immune system. M protein can also activate T lymphocytes, which can lead to an inflammatory shock response.
Marine organisms such as Vibrio vulnificus are rare causes of gangrene and have mostly been reported in warm coastal regions. Route of infection can be through an open wound exposed to water, or via ingestion of infected oysters. Systemic toxicity tends to occur early.
Risk factors for necrotising infections include:
The clinical features of necrotising infections depend upon the location and cause.
Necrotising infections frequently resemble cellulitis or an abscess initially, but progress to discolouration (blue to black), foul-smelling discharge, and/or numbness. If the affected area is internal, symptoms may include confusion, fever, gas in the tissues under the skin, low blood pressure and persistent or severe pain.
The early signs of gangrene that should result in an urgent investigation are:
Less specific signs that should increase clinical suspicion of necrotising infection include:
Necrotising skin infections may progress rapidly to wet gangrene, unlike cellulitis or abscess.
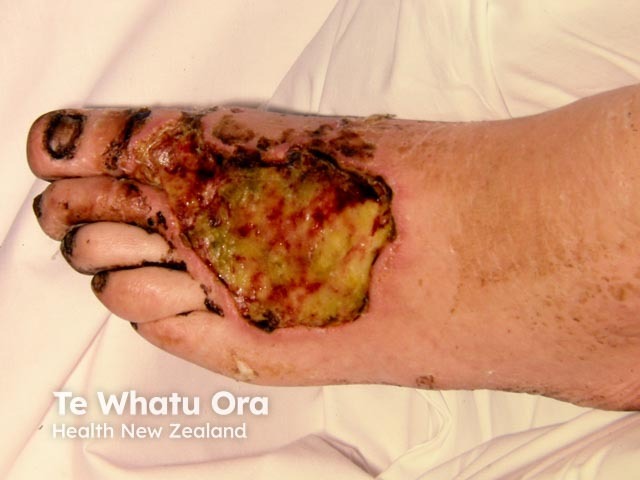
Necrotising skin infection
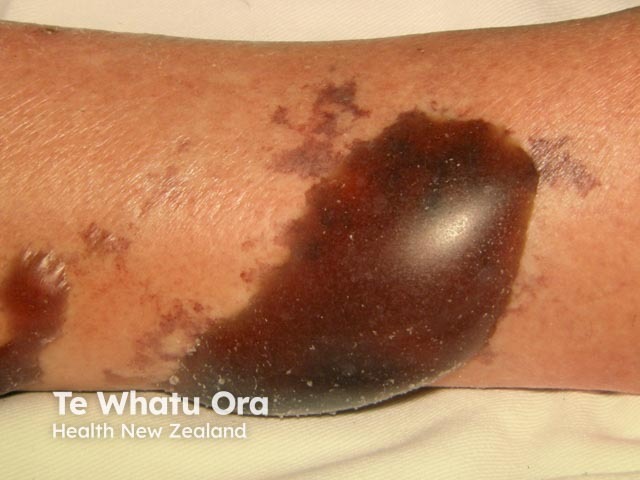
Necrotising skin infection
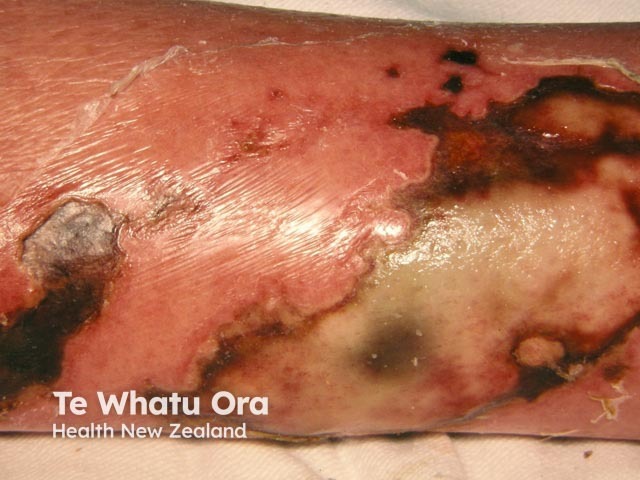
Necrotising skin infection
Blood cultures should be undertaken to identify specific organisms involved in the infection.
The table below was developed as a risk indicator for necrotising fasciitis by Wong et al. in 2004. Scores ≥6 were found to have a 92% positive predictive value and a 96% negative predictive value.
Elements of the laboratory risk indicator for necrotizing fasciitis (LRINEC) score |
|
|---|---|
Laboratory marker |
Scoring evaluation |
CRP (mg/dL) |
150 = 0 points |
WBC (per mm3) |
15 = 0 points |
Hb (g/dL) |
> 13.5 = 0 points |
Serum sodium |
> 135 = 0 points |
Serum creatinine |
≤ 1.6 = 0 points |
Serum glucose |
180 = 0 points |
CRP: C-reactive protein; Hb: haemoglobin.
Imaging has a limited role in the diagnosis of infectious gangrene.
Treatment of gangrene depends on location and cause, but is centred around:
Management may also include:
The incidence of wartime gas gangrene has markedly reduced with identification and isolation of cases, and early debridement, amputation and supportive treatment.
Prognosis in wet gangrene depends on the extent of disease, the underlying cause and the timing of appropriate treatment.
Anaya et.al have constructed a clinical score to predict patient outcomes for infective gangrene based on several clinical criteria:
Patients with few of these findings had a 6% risk of death in this study, while patients with several findings had up to an 88% risk of death. Prognosis can vary widely due to the aggressive nature of gangrene if treatment is not accessed early.