Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2006. Updated by Dr Arun Gangakhedkar, Paediatrician, Waitakere Hospital, Auckland, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. October 2018.
Introduction Demographics Causes Clinical features Cutaneous features Physiological manifestations Chronic skin manifestations Diagnosis General management Outcome
Down syndrome is a common genetic disorder resulting from the chromosomal abnormality, trisomy 21. Individuals with Down syndrome have a cognitive delay and characteristic appearances associated with certain medical conditions [1–8].
The incidence of Down syndrome rises with advancing maternal age, but most individuals with Down syndrome are born to younger mothers under 30 years owing to a greater number of pregnancies in this age group. Due to an increase in the terminations of pregnancies with Down syndrome, the live birth prevalence has decreased from one in 700 to about one in 1000 in New Zealand.
Studies suggest marginally higher rates of Down syndrome in boys than girls.
A cell division error during early conception results in three copies of chromosome 21 instead of the usual two. The chromosomal abnormality results from nondisjunction (a lack of normal separation) during cell division as the pair of chromosomes in either the sperm or egg fail to separate. This results in a gain of an additional chromosome 21 and the occurrence of Down syndrome [1–8].
The clinical phenotype in all types of Down syndrome is similar, with the subtle differences in mosaic Down syndrome depending on the extent of an individual's trisomy 21 cell population.
The diagnosis is suspected or confirmed in the neonatal period in most infants with Down syndrome. Characteristic physical features of Down syndrome include [1–8]:
Cognitive delay is present in all individuals with Down syndrome. Children are reported to have higher rates of a seizure disorder (8%), coeliac disease, and diabetes (1%).
Red cell macrocytosis and polycythaemia may affect up to two-thirds of infants with Down syndrome. Transient myeloproliferative disorder (TMD), a type of leukaemia resulting from trisomy 21, may be present in up to 10% of newborns. Acute leukaemias are reported in 1 in 300 individuals with Down syndrome.
A single transverse palmar crease is the main cutaneous phenotype and is easily detectable. However, a single transverse palmar crease may also occur as a normal variant that is unilateral in 4% and bilateral in 1% of the general population [9–18].
Other cutaneous features include dry skin and a large tongue (macroglossia) with a fissured appearance.
A variety of dermatological disorders are more common in Down syndrome due to a combination of immune and genetic dysregulation and inefficient physiological processes.
Defective regulation of genes located on chromosome 21 may play a role in keratosis pilaris, alopecia areata, and vitiligo. Immune dysregulation leads to increased susceptibility to bacterial and fungal skin infections.
Transient physiological cutaneous manifestations are common during infancy, and chronic skin conditions appear with age.
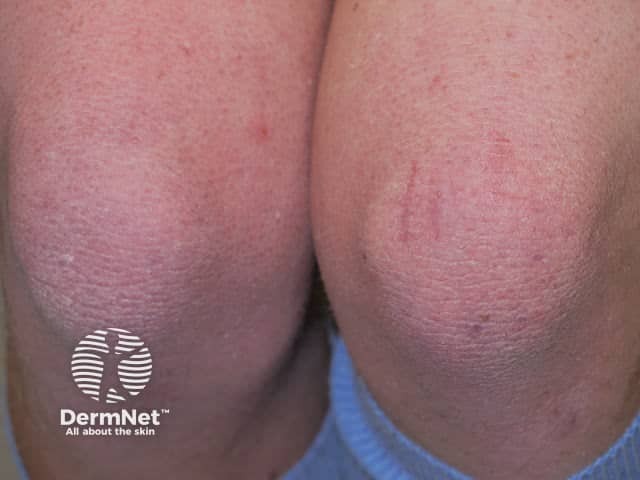
Xerosis
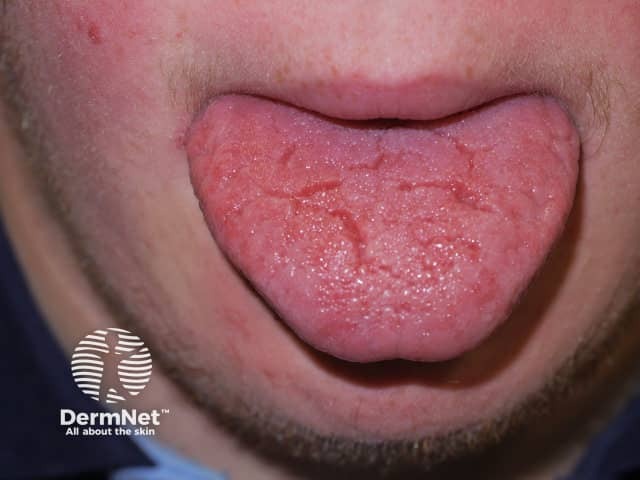
Fissured tongue
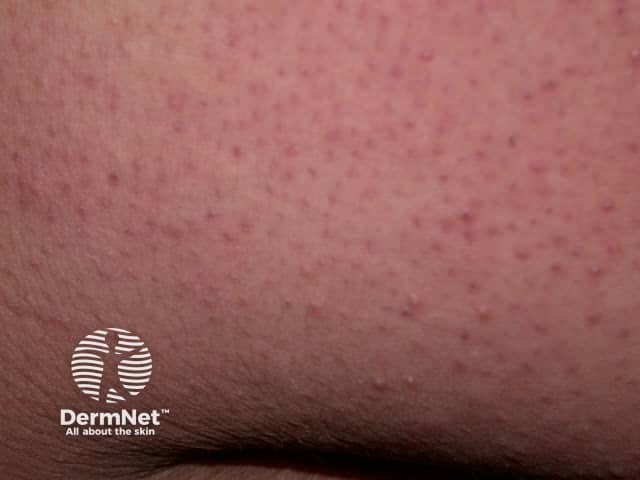
Keratosis pilaris
Acrocyanosis is due to poor peripheral circulation and is more pronounced in Down syndrome. It is commonly observed in newborns.
Cutis marmorata is a lacy, mottled skin discolouration common during early infancy due to altered blood flow in the small blood vessels of the skin. The discolouration is most marked in skin exposed to cooler environmental temperatures.
The skin change due to livedo reticularis is similar but less marked than cutis marmorata. Livedo reticularis mostly affects the lower limbs but may also be present on the arms and trunk. It becomes more pronounced in cold weather.
The signs of premature ageing reported in Down syndrome include greying or thinning of the hair, skin atrophy, early development of rhytids (wrinkles), and lentigines. The overexpression of the SOD gene, which regulates free radical metabolism, is located on chromosome 21, and is overexpressed as a result of trisomy 21; this leads to excess production of hydrogen peroxide, causing the release of cytotoxic hydroxyl radicals. This, in turn, causes cell-membrane lipid oxidation, altering the structure and function of the skin and involved tissues.
The skin texture is soft and velvety in newborn infants with Down syndrome in comparison to unaffected infants. The skin becomes rough with an altered texture during the school years, with most adolescents and adults showing chronic skin changes [9–18].
Chronic skin conditions associated with Down syndrome may be related to immune insufficiency, autoimmune processes, infections and infestation-related complications, and defects of keratinisation or connective tissue.
The skin in Down syndrome becomes increasingly dry, rough, and inelastic, and there is patchy lichenification with increasing age.
Recent studies report a prevalence of atopic eczema of up to 5%, which is similar to the general population. The patches of eczema are red, scaly, and itchy. They generally involve the cheeks, behind the ears, knees, and elbow flexures. Malar erythema is more commonly seen in Down syndrome than in unaffected individuals. Dry skin predisposes individuals to irritant contact dermatitis and allergic contact dermatitis.
Seborrhoeic dermatitis occurs in about a third of individuals with Down syndrome, often associated with Malassezia folliculitis. It presents as an erythematous rash with yellow-brown scales involving the scalp, midfacial ‘T’ region, behind the ears, upper chest, and back.
Palmoplantar keratoderma is thickened skin on the palms and soles and affects up to 40% of those with Down syndrome. Although uncommon in infants under 5 months, the prevalence of palmoplantar keratoderma is up to 75% for children over 5 years with Down syndrome.
Keratosis pilaris describes rough pinpoint spots (which may contain twisted hair) with varying red–brown pigmentation. The papules affect the upper outer arms, and sometimes the thighs, outer cheeks, trunk, and buttocks, and occasionally the forearms and lower legs. Keratosis pilaris usually appears in adolescence for those with Down syndrome.
Pityriasis rubra pilaris (PRP) is a rare chronic papulosquamous disorder of unknown cause. It is characterised by well-defined areas of hyperkeratotic follicular papules that may evolve into erythroderma. PRP causes thick, smooth, yellow palms and soles, and abnormal nails. Immunodeficient states may trigger severe forms of PRP.
The incidence of psoriasis in the general population is 1–3%; the range is 0.5–8% in people with Down syndrome. Immunocompromised patients may develop severe psoriasis.
Syringomas are benign tumours of the eccrine appendages. They are reported in 18–39% of individuals with Down syndrome (up to 30 times more common than in the general population). They are more commonly found in girls and women. Syringomas often develop during adolescence. They are small (0.5–3 mm) flesh-coloured or yellow–brown dermal papules and are typically distributed in the periorbital area.
Cutaneous calcinosis may present as asymptomatic discreet, firm, small, chalky-white milia-like papules. These mostly arise on the hands and feet. Their pathogenesis is unclear. Increased sweat calcium and calcification of eccrine ducts may contribute, as there is no preceding injury or calcium metabolism abnormality. The calcinosis heals without scarring. The differential diagnosis includes molluscum contagiosum, viral warts, milia, and inclusion cysts.
Elastosis perforans serpiginosa (EPS) is rare, affecting about 1% of patients with Down syndrome. It presents as asymptomatic, erythematous, and coalescent 2–5 mm keratotic papules arranged in linear, arcuate, or serpiginous patterns. The papules may have umbilicated centres. EPS most commonly appear on the neck but also affects the chin, cheeks, arms, and knees with asymmetrical distribution. The lesions develop slowly during adolescence and spontaneously resolve over 6 months to several years, leaving atrophic linear or retiform scars. Generalised EPS is associated with Down syndrome while the idiopathic form is usually localised. EPS may represent a connective tissue dysplasia with transepidermal elimination of thickened elastic fibres. It is also associated with other connective tissues disorders such as Ehlers–Danlos syndrome, Marfan syndrome, cutis laxa, pseudoxanthoma elasticum and osteogenesis imperfecta; and it may also be induced by D-penicillamine. The differential diagnosis of EPS includes granuloma annulare, tinea corporis, annular sarcoidosis, cutaneous calcinosis, and porokeratosis of Mibelli.
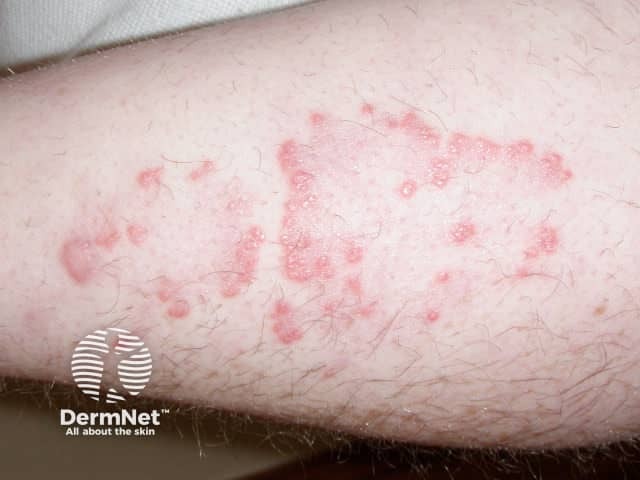
Elastosis perforans in Down syndrome
Anetoderma is a circumscribed area of flaccid skin, often with fat herniation and a ‘button-hole’ sign on palpation. It most often affects the chest, back, necks, and arms. It is usually secondary to elastolysis, which is induced by leukocytes or bacteria associated with chronic folliculitis. The congenital malformation of elastic fibres in Down syndrome may predispose patients to anetoderma.
Oral lesions are common in individuals with Down syndrome.
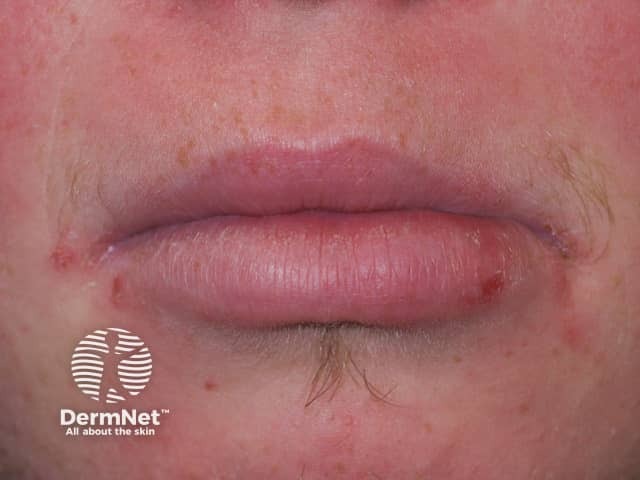
Angular cheilitis in Down syndrome
Vitiligo presents at any age, with the loss of skin pigmentation anywhere on the body. There is a 3% prevalence of vitiligo in Down syndrome, which is marginally above the 2% prevalence in the general population.
Other pigmentation abnormalities are common in individuals with Down syndrome.
Alopecia areata affects 6–10% of those with Down syndrome compared to the >2% prevalence in the general population.
Dermatitis herpetiformis is rare. It causes a symmetrical, pruritic, 1–3 mm papulovesicular and erosive rash on the extensor aspects of limbs, buttocks, and the midline of the back. Purpuric lesions may be seen on the fingers and toes in children. A coeliac screen should be completed if dermatitis herpetiformis is suspected. Subepidermal bullae with microabscesses in the dermal papillae, with immunoglobulin A deposits on direct immunofluorescence, are confirmatory on skin biopsy.
Hidradenitis suppurativa causes pustules, nodules, and abscesses in the armpits and groins. The response to treatment with standard antibiotics is often poor.
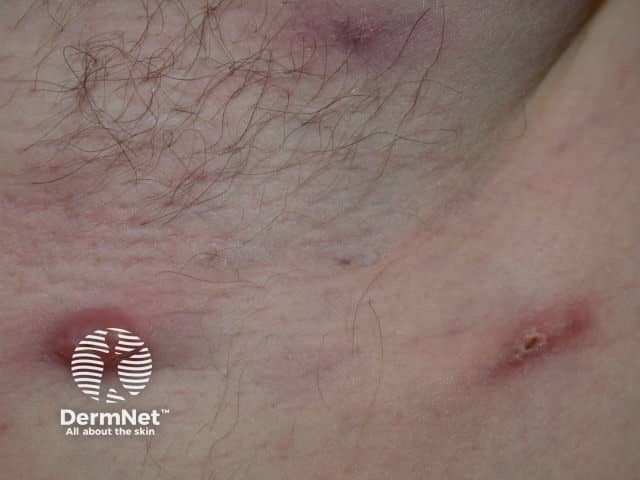
Hidradenitis suppurativa in Down syndrome
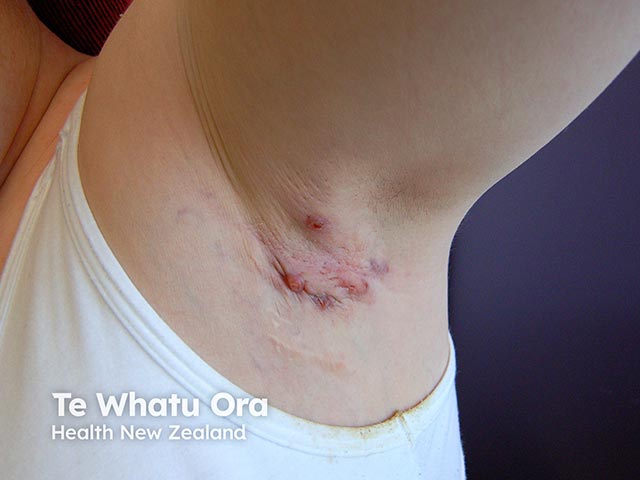
Folliculitis in Down syndrome
A variety of bacterial skin infections affect patients with Down syndrome.
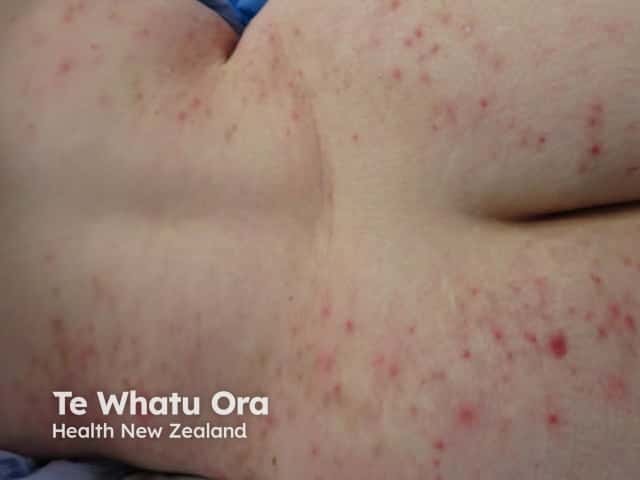
Folliculitis in Down syndrome
Tinea pedis and onychomycosis are common in Down syndrome.
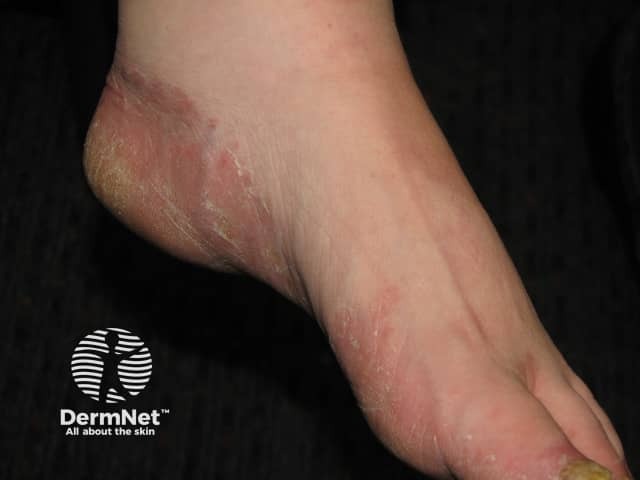
Tinea pedis
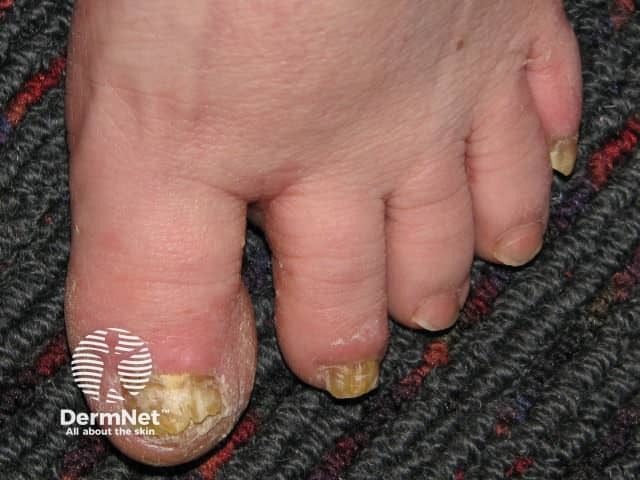
Tinea unguium
People with Down syndrome are predisposed to scabies infestations. Crusted scabies may occur in Down syndrome and can be asymptomatic and thus diagnosed late, leading to a risk of widespread infestation in the community.
Lichen nitidus causes asymptomatic, flesh-coloured shiny papules (1–2 mm) distributed in crops over the genitalia, abdomen, trunk, and/or upper limbs in children. The histopathology of lichen nitidus reveals focal papillary dermal lymphohistiocytic infiltrates resembling a ‘claw’ or ‘baseball glove and ball’. The strength of the association with Down syndrome is unknown, but several case reports are cited in the medical literature [19].
Acanthosis nigricans is a marker of insulin resistance and is associated with obesity. It affects the flexures of the neck, the axilla, and groin. Rarely, it may also affect the flexor aspect of the elbow and knee and the dorsal interphalangeal and metacarpal joints.
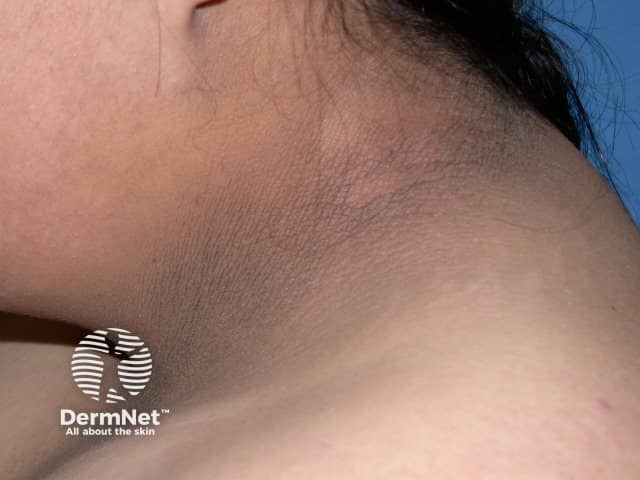
Acanthosis nigricans
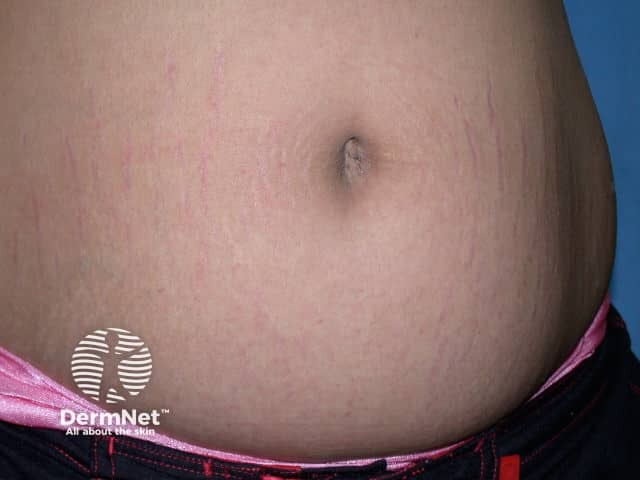
Striae atrophicae
Carotenoderma is a benign yellow–orange hue of the skin involving the nasolabial folds, outer ears, palms, and soles, but sparing the mucous membranes and sclera. It is due to eating excessive carotenoid-rich fruits and vegetables, such as carrots and pumpkin, and has been reported in children on exclusion diets due to food allergy [20]. Hypothyroidism associated with Down syndrome may accentuate carotenoderma.
Rarely, blood disorders such as a transient myeloproliferative disorder or congenital leukaemia are reported in infants with Down syndrome.
Leukaemia cutis presents as characteristic blue, firm, infiltrated papules or nodular skin lesions.
A clinical diagnosis of Down syndrome is always confirmed by cytogenetic analysis. A standard or conventional karyotype should be requested. A rapid fluorescent in-situ hybridisation (FISH) analysis for trisomy 21 should be specified on the laboratory request form when an urgent result is required.
Post-term, a diagnosis of Down syndrome can be made from the identification of characteristic phenotypic features, but the clinical diagnosis is not always possible in patients with mosaic Down syndrome.
Genetic disorders such as Smith–Magenis syndrome, Zellweger syndrome, and Beckwith–Weidemann syndrome, may be confused for Down syndrome as these syndromes present with similar phenotypic features in early infancy.
A careful skin examination is required as dermatological problems are reported in up to 87% of individuals with Down syndrome [9–18].
Managing skin and associated medical conditions is important in providing optimal medical care for individuals with Down syndrome.
Other related support services should include:
Most skin conditions may be managed with optimal care and supervision.
Longevity in individuals with Down syndrome is influenced by the severity of their congenital abnormalities and associated medical problems. Substantial improvements in the lifespan are observed with better health surveillance and management compared to a few decades ago.