What are amputation stump dermatoses?
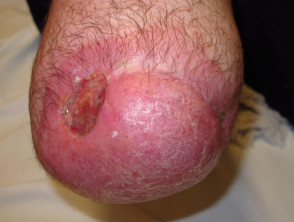
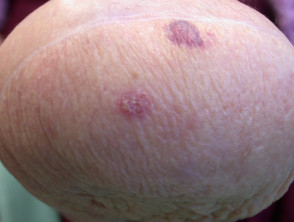
Amputation stump dermatoses are skin diseases affecting the stump, following the amputation of a limb. They can occur immediately after surgery, or not until many years later. They are also called amputation-related dermatoses.
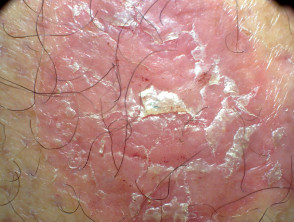
Amputation stump dermatoses
How common are amputation stump dermatoses?
Stump dermatoses are reported to affect between 34–74% of amputees [1]. Figures vary according to the design, population samples and methods used in the studies.
Skin problems tend to persist long term, as described in war veterans 38 years after amputation [1].
Why do skin problems occur on the stump after amputation?
Factors that make the stump vulnerable to skin disease include:
- Underlying conditions that gave rise to the amputation eg, occlusion of small blood vessels in vascular disease such as diabetes or thromboembolic disease
- Variable swelling due to operation, bandaging, venous congestion
- Scarring at the site of the surgical operation
- Poorly fitting prosthesis
- Lack of physiological adaptation to pressures applied by the limb prosthesis
- Trapping of perspiration in the closely-fitted socket of the prosthesis
- Proliferation of commensal (normal) and pathogenic bacteria
- Close contact of materials of the limb prosthesis, which may irritate the skin or rarely, cause an allergic reaction [2].
Although dermatoses may arise before a prosthesis is fitted and used, the main contributing factors are the degree of activity and the use of a prosthesis [2]. Severity also depends on:
- Age of patient
- Reason for amputation
- Pre-existing skin diseases such as atopic dermatitis or psoriasis
- Level of amputation (below or above knee)
- Type of gait
- Materials used to make, clean or repair the prosthesis including resins, adhesives, rubber
- Products applied to the skin such as cleansers, emollients, antiperspirants
- Walking aids.
Which skin conditions affect the amputation stump?
Skin problems affecting an amputation stump are listed below.
Vascular occlusion
- Purpura, necrosis (death of tissue), ulceration
- Verrucous hyperplasia due to venous congestion and/or lymphoedema
Mechanically induced problems
- Pressure ulcers, erosions and abrasions
- Epidermoid cysts and sinues from repetitive rubbing and friction
- Corns and calluses
Koebner phenomenon (dermatosis arising in injured skin)
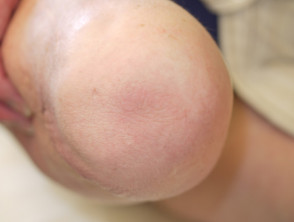
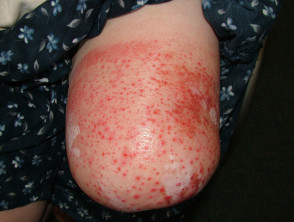
Skin problems affecting an amputation stump
Dermatitis
- Irritant contact dermatitis
- Sweat rash in skin folds and creases (intertrigo)
- Allergic contact dermatitis to cleanser, skin product or prosthetic material (should be confirmed by patch tests)
- Venous stasis / gravitational dermatitis
Infection
- Bacterial infections such as cellulitis, boils and folliculitis
- Yeast (candidiasis) and dermatophyte (tinea) fungal infections
- Viral infections such as molluscum contagiosum
Physical factors
- Cold skin and excessive perspiration (localised hyperhidrosis) [3]
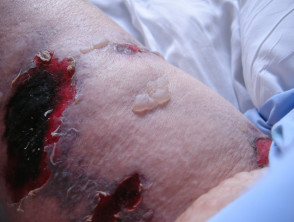
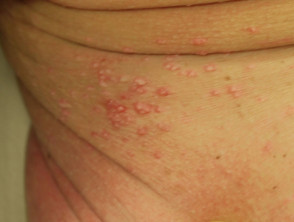
Skin problems affecting an amputation stump
Of these, pressure ulcers and skin breakdown (39%) and infection (25%) are most common [1][2][5], with up to one quarter of amputees being affected more than 50% of the time.[1] In some cases, rashes are unexplained.
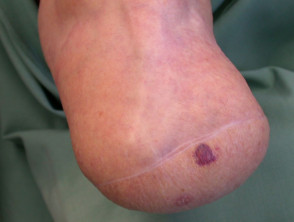
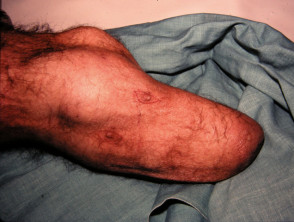
Common skin lesions such as warts, moles and skin cancer can also arise on the stump.
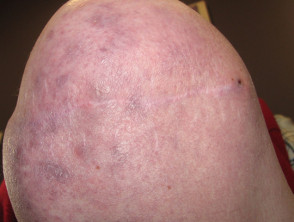
Skin cancer arising on limb of amputee
The impact of stump dermatoses on the amputee
Adverse physical, mental, and emotional effects of stump dermatoses may affect wellbeing and quality of life, including:
- Reduced use of the limb prosthesis, reported in up to 53% of amputees [5]
- Reduction in walking distance because of pain or irritation of the stump site
- Repeated alterations and replacements of the prosthetic limbs
- Prosthesis abandonment.
Skin care for amputees
To prevent complications due to poor skin care, check the amputation stump daily, keep the skin dry by changing damp socks promptly, and protect bony prominences and pressure-sensitive areas from injury.
- Wear compression garment or bandages to reduce swelling and scarring.
- Cleanse daily with hypoallergenic non-soap cleanser, completely remove the cleanser by rinsing, and dry gently and thoroughly with a soft clean towel.
- Moisturise dry skin at night using a bland, non-perfumed emollient.
- Ensure socks are soft and non-irritating and change them as soon as they are damp and at least daily.
- Clean liner and socket daily.
- Remove appliance and rest if sores occur.
- Seek help from limb-fitting centre and from your doctor promptly.
Diabetics need to be vigilant to monitor and control blood sugar levels, and to inspect numb areas of skin frequently.
Treatment of amputation stump dermatoses
Treatment of stump dermatoses depends on careful evaluation to establish contributing factors.
- Powders and unperfumed antiperspirants can be used to reduce sweating.
- Bacterial infections are treated with antiseptic washes, antibiotics.
- Calluses are treated with keratolytic agents such as urea cream.
- Cysts may require surgical removal and refitting the appliance.
- Ingrown hairs and folliculitis are treated by not shaving, antibiotics and if necessary permanent hair removal.
- Yeast and fungal infections are treated with topical or oral antifungal agents.
- Dermatitis is treated with emollients and topical steroids.
- Surgery to excise areas of wound breakdown or to revise the amputation.
Unfortunately the skin may fail to adapt to mechanical pressures, materials, and closed environment associated with the use of a prosthesis [1].