Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amy Stanway, Department of Dermatology, Waikato Hospital, Hamilton, New Zealand, February 2004.
Introduction
Atopy
The inherited barrier defect
The immune system
The microbiome
Skin dryness
Irritants
Infection
Allergens and eczema
Stress
Climate
There is no known single cause for atopic dermatitis (eczema) and it probably represents more than one condition. There are many theories regarding the underlying mechanisms. Current research is investigating the roles of the immune system, skin structural gene mutations, defects in the skin cells (keratinocytes), the skin surface microbiome (bacteria, viruses and yeasts), and many other factors.
Current theories identify that atopic dermatitis is primarily a disease of the immune system, with cytokines being critical components to the disease. These cytokines, particularly IL-4 and IL-13 (Th2 pathway cytokines) and IL-22 (the Th22 axis cytokine) cause barrier defects and inflammation that result in the clinical features of eczema.
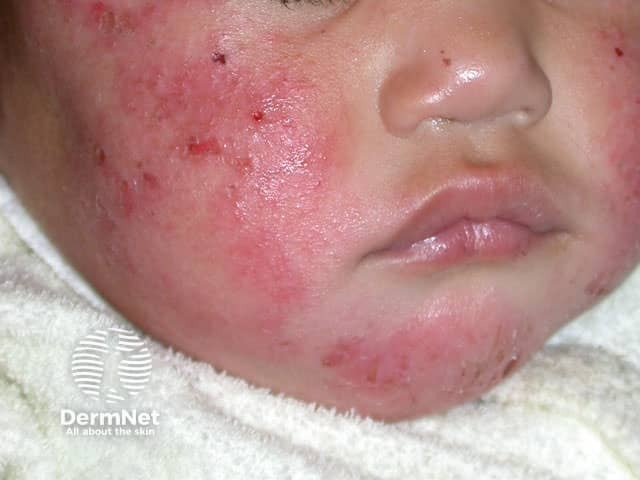
Atopic eczema
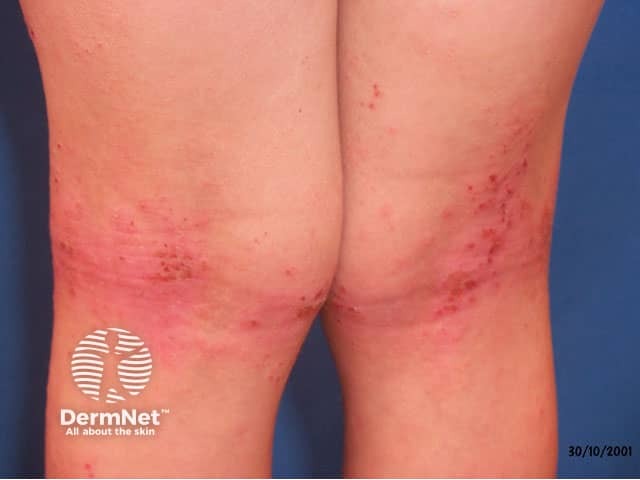
Atopic eczema
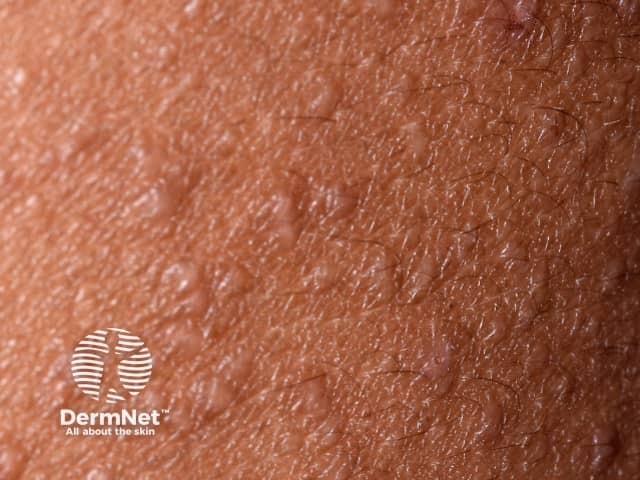
Close-up of follicular atopic dermatitis
Atopy refers to the tendency to asthma, eczema and hay fever. Atopy is mostly inherited (genetic). It is characterised by an overactive immune response to environmental factors. The same factors have no effect on the skin of a non-atopic. Yet, despite their genetic background, some children from an atopic family never develop atopic dermatitis and children with no family history can suffer from it. For more information, see the webpage on atopy.
Atopic dermatitis is a disease of the whole body that manifests in the skin. Events that upset the body in other ways (such as viral infection, teething, eating certain foods) may have an effect on dermatitis. Flares may also occur without obvious provocation and can be very frustrating.
There is emerging evidence that inflammation in atopic dermatitis is associated with immune-mediated and inherited abnormalities in the skin barrier. This barrier failure causes increased permeability of the skin and reduces its antimicrobial function.
The main inherited abnormality causing disordered barrier function is filaggrin expression. Filaggrins are filament-associated proteins which bind to keratin fibres in the epidermal cells. The gene for filaggrin (FLG) resides on chromosome 1 (1q21.3). This gene was first identified as the gene involved in ichthyosis vulgaris. Abnormal filaggrin is associated with early-onset, severe and persistent atopic dermatitis.
It is postulated that the loss of filaggrin results in:
Proteins under investigation in atopic eczema include structural compounds, such as hornerin, cornulin, claudin 1/23 and ceramides, enzymes, such as kallikrein (a protease) and serine peptidases.
The immune system develops in the first six months of life. There is a generally an equilibrium of the two main types of T Helper lymphocytes (small white blood cells), Th-1 and Th-2. In atopic dermatitis, there is often an imbalance, with far more Th-2 cells and their associated chemical messengers (cytokines). In some children, there are also high levels of the antibody immunoglobulin E (IgE) antibodies and eosinophils (the white blood cells associated with allergy).
The Th2 associated cytokines contribute to the loss of skin barrier function:
The specialised immune cells of the epidermis (Langerhans cells) have an increased response to these antigens in atopic dermatitis and interact with dermal T cells to produce an even greater Th2 response further exacerbating the barrier defect.
So both the genetic make-up of the individual and external environmental factors contribute to the likelihood of developing eczema, its severity and its response to treatment.
Very rarely, atopic dermatitis may be due to an underlying inherited immune deficiency such as Job syndrome. In this disease, dermatitis appears very soon after birth and is complicated by severe infections.
The functions of microbial components of the skin flora have only recently become of interest to atopic dermatitis researchers. It is postulated that different organisms in different body sites might account for the characteristic distribution of active lesions of atopic dermatitis — for example in the moist elbow and knee creases.
The microbiome likely contributes to normal and abnormal inflammatory responses in the skin. Flares of atopic dermatitis are accompanied by a proliferation of Staphylococcus aureus on lesional skin and a reduction in the biodiversity of the cutaneous microbiome (dysbiosis), with fewer malassezia yeasts and cutibacteria than are present on normal skin. Researchers report that emollients can increase biodiversity in eczema skin.
A study suggests there may be an increased risk of AD in children exposed to antibiotics in-utero, depending on the mother's AD history (20-40%). And an increased risk in children who are exposed to antibiotics early-in-life, depending on the antibiotic (40-80%). Penicillin had the strongest association.
Another focus of research is the role of the intestinal microbiome.
Dry skin is a sign of the loss of barrier function. Factors that make the skin even drier may make eczema harder to control:
A brief shower or bath once a day is enough if you have dry skin. However, your doctor may specifically recommend bathing for longer or more often during the acute blistered phase of eczema. Use a non-soap cleanser.
Regular use of an emollient helps skin retain moisture and combat dryness.
Most people with eczema will notice that certain things seem to irritate their skin with immediate stinging or itching and may also cause a flare of eczema (irritant contact dermatitis). These are not allergies.
It is common sense to avoid the substances that irritate.
Antigen stimulation
Infective organisms play an important role in triggering and aggravating atopic dermatitis. Bacteria (particularly staphylococci) and in some patients yeasts (malassezia and candida) contribute to chronic inflammation.
Bacterial infection
People who have atopic dermatitis are particularly prone to skin infections with Staphylococcus aureus.
As a result, people with atopic dermatitis frequently suffer from boils, folliculitis and infected eczema.
The infection causes eczema to worsen and become more resistant to the usual treatment with emollients and topical steroids. S. aureus produces enterotoxin. This induces the production of enterotoxin-specific IgE, resulting in proliferation and recruitment of more T cells and aggravating dermatitis.
Antibiotics are often required to eliminate the infection and control eczema. However, antibiotics may reduce the biodiversity of the microbiome.
Viral infections
Fungal infections
Dermatophyte infections (tinea) do not appear to be more prevalent in atopic dermatitis.
Food allergies
Food allergies affect about a third of children with eczema. They are most commonly to egg, cows milk, soy, wheat, peanuts and fish. The reaction may be acute urticaria (hives) sometimes accompanied by swelling of the face and tongue (angioedema) or abdominal pain shortly after ingesting the offending food. Severe allergy causes anaphylaxis and the patient may collapse and even die. Any tiny amount of food allergen can cause this response. These reactions are not eczema.
However, eczema can be aggravated by certain foods in other ways (food intolerance).
Environmental allergies
Environmental allergens may sometimes be related to atopic dermatitis. Many children with atopic dermatitis are allergic to grass, dust mites and cat dander. Usually, this manifests as an immediate reaction with a runny nose, sneezing and swollen eyes, and improves after removal from the allergy source. It is uncommon for this type of allergy to cause persistent worsening of eczema.
Allergic contact dermatitis is equally common in those without atopic dermatitis.
Environmental particulate exposure during gestation and in the first 30 weeks of life may be associated with an increased risk of developing eczema.