Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Based on Dr Amy Stanway's article on Cutaneous Vasculitis, 2003; minor update by Dr Ian Coulson, Dermatologist, Sept 2024.
Previous authors: A/Prof Amanda Oakley, Dermatologist (2016).
Introduction - vasculitis
Introduction - small vessel vasculitis
Demographics
Causes
Clinical features
Diagnosis
Treatment
Prevention
Outlook
Vasculitis is a disorder in which there are inflamed blood vessels. These may include capillaries, arterioles, venules and lymphatics.
Small vessel vasculitis is the most common form of vasculitis affecting arterioles and venules.
Small vessel vasculitis is also called immune complex small vessel vasculitis. The term hypersensitivity vasculitis is used for cutaneous small vessel vasculitis due to known drug or infection.
There are particular types of small vessel vasculitis that present with similar cutaneous signs and should be considered in the differential diagnosis.
Cutaneous small vessel vasculitis mainly affects adults of all races over the age of 16. Children are more likely to have Henoch-Schönlein purpura, a distinctive vasculitic syndrome associated with deposits of IgA in the skin and kidneys.
Secondary cutaneous small vessel vasculitis often affects older people, because they are more likely to have diseases and medications (alone or in combination) that are potential causes of vasculitis.
Many different insults may cause an identical inflammatory response within the blood vessel wall. Three main mechanisms are proposed.
Vasculitis can be triggered by one or more factors. In the past, it was frequently seen with administration of antisera (serum sickness) but is now more often due to drugs, infections and disease. In most cases, an underlying cause is not found.
A large series of 440 patients over a 14-year period presenting with leukocytoclastic vasculitis of the skin 82% had disease limited only to the skin, 12% had HSP, and a small number of cases had an underlying systemic connective tissue disease. Of those with cutaneous disease only, most cases were of unknown cause, 27% were drug-induced, 18% due to bacterial infection, 5% virally induced, and 1% had an underlying malignancy.
Bacterial endocarditis due to Bartonella (often culture negative endocarditis) has been highlighted as an important cause not to overlook.
Drugs are frequently responsible for cutaneous small vessel vasculitis, particularly in association with infection, malignancy or autoimmune disorders. The onset of vasculitis is often 7–10 days after the introduction of new medicine, such as:
Foods and food additives, for example, tartrazine, are rare causes of vasculitis.
Examples of infections associated with cutaneous small vessel vasculitis include:
Cancer is found in fewer than 5% of patients with cutaneous small vessel vasculitis. It is thought that malignancy leads to more circulating antibodies and viscous proteins that may sludge within small blood vessels.
Autoimmune disorders such as systemic lupus erythematosus (SLE), dermatomyositis, and rheumatoid arthritis are characterised by circulating antibodies that target the individual's tissues. Some of these antibodies can target blood vessels, resulting in vasculitis.
The main reason that vasculitis affects the lower leg is reduced blood flow because this leads to the deposition of mediators of inflammation on the blood vessel wall. Contributing factors include:
The clinical features of hypersensitivity vasculitis include:
The initial acute rash of small vessel vasculitis usually subsides within 2–3 weeks, but crops of lesions may recur over weeks to several months, and hypersensitivity vasculitis may rarely become relapsing or chronic.
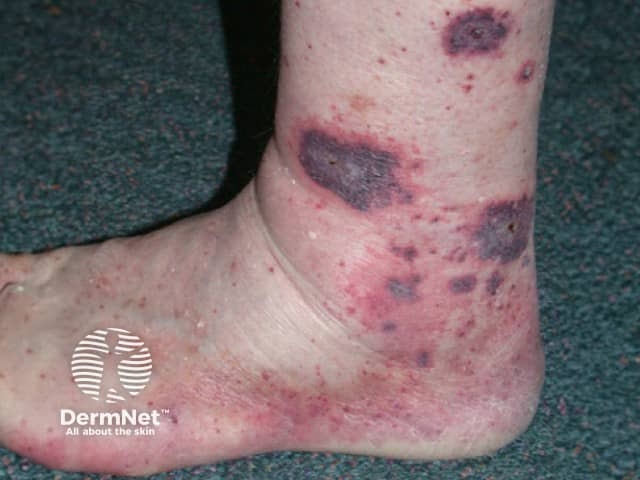
Cutaneous vasculitis
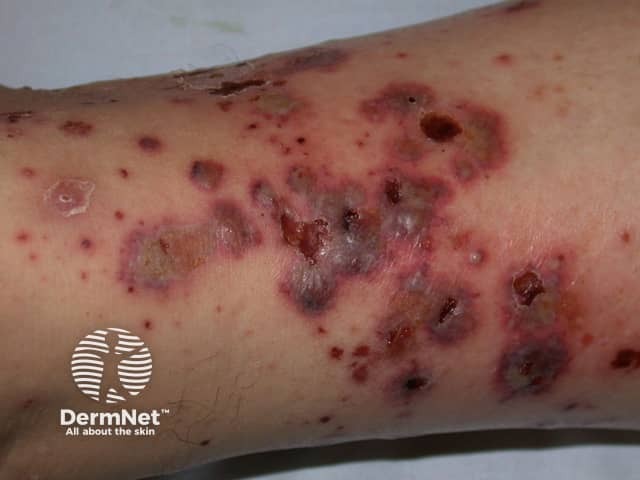
Cutaneous vasculitis

Hypersensitivity vasculitis
The most severe complications of small vessel vasculitis are seen with its systemic forms, such as kidney disease associated with Henoch-Schönlein purpura.
Local ulceration from cutaneous small vessel vasculitis can lead to:
The clinical diagnosis of an acute cutaneous small vessel vasculitis is generally straightforward.
Thorough history and examination are essential to determine if symptoms and signs are confined to the skin, or if there may be systemic involvement, and to establish a cause.
Cutaneous small vessel vasculitis is confirmed by 4-mm punch biopsy of an early purpuric papule, ideally present for 24–48 hours. Histopathology reveals neutrophils around arterioles and venules, and fibrinoid necrosis (fibrin within or inside the vessel wall). There may be extravasated red cells, leukocytoclasis (broken-up neutrophils within the vessel wall) and signs of an underlying disease.
Direct immunofluorescence (DIF) of a lesion less than 24 hours old often reveals immunoglobulins and complement.
Screening tests are requested to identify any underlying cause and to determine the extent of involvement of internal organs. The history and symptoms may suggest these. Patients should have:
Additional tests may include:
If an initial screen indicates an abnormality or there is clinical suspicion of a more widespread vasculitic process, further investigations will be requested. The majority of patients presenting with palpable purpura have primary cutaneous small vessel vasculitis, and no underlying cause is found in spite of extensive investigations.
In most patients presenting with the first episode of acute cutaneous small vessel vasculitis, general measures are all that is required to keep the patient comfortable until the rash spontaneously resolves.
Medications used to control cutaneous vasculitis have not been subjected to randomised trials. They are recommended in acute vasculitis when ulcerated and in symptomatic relapsing or chronic disease. They include:
Other treatments reported to be helpful in at least some cases include:
If cutaneous vasculitis is a manifestation of systemic vasculitis, treatment of the systemic disorder is required.
Flares of cutaneous small vessel vasculitis can be minimised by rest, compression and elevation of lower legs.
Once a drug is identified as the cause of small vessel vasculitis, the patient should avoid it lifelong. It is not usually possible to prevent other forms of vasculitis.
Idiopathic/primary cutaneous small vessel vasculitis is self-limiting. Most cases resolve within a period of weeks to months. When the cause is an underlying disease, the vasculitis may recur at variable intervals after the initial episode.
It is common for an orange-brown discolouration of the skin due to haemosiderin deposition to persist for weeks or months after the inflammatory disease has settled.
The prognosis of systemic vasculitis is dependent upon the severity of involvement of other organs. If vasculitis affects the kidneys, lungs or brain, it can be life-threatening.