Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: May, 2022
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Discoid lupus erythematosus (DLE) is a chronic scarring skin condition. It is the most common form of cutaneous lupus.
DLE is a sub-type of chronic cutaneous lupus erythematosus. It is characterised by persistent scaly plaques on the scalp, face, and ears which subsequently can progress to scarring, atrophy, dyspigmentation, and permanent hair loss in affected hair-bearing areas.
DLE can affect males and females of any age but occurs more frequently in women in their 20s, 30s, and 40s. Children are rarely affected. The estimated prevalence is around 20–40 people in every 100,000.
DLE is more common in skin of colour. For example, in New Zealand, Māori, and Pacific people have a significantly higher relative risk of discoid lupus erythematosus compared to the European population. This ethnic disparity has also been observed in the USA with those with skin of colour having an increased incidence of DLE.
The causes of DLE are endogenous and exogenous.
Endogenous factors include:
Exogenous factors include:
DLE may be localised (above the neck in 80%) or generalised (above and below the neck in 20%). Often the rash is asymptomatic but it can be itchy and sore. Most patients with DLE only have skin involvement but some have or subsequently develop signs of SLE. Typically, the lesions evolve over time.
Typical signs of localised DLE include:
Signs of generalised DLE include:
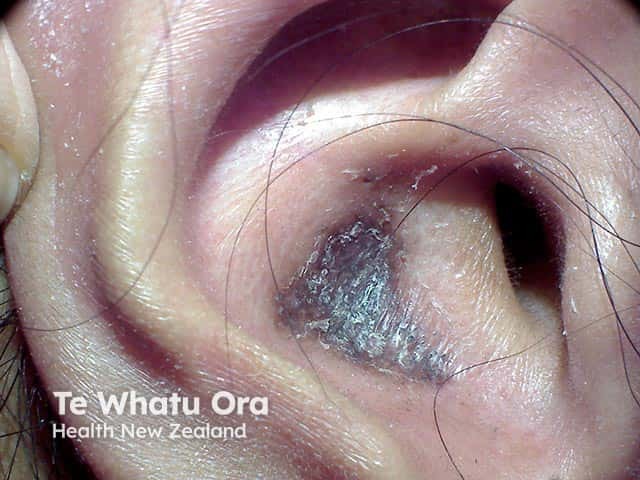
Conchal bowl discoid lupus erythematosus (Shuster sign) (DLE-patient4)
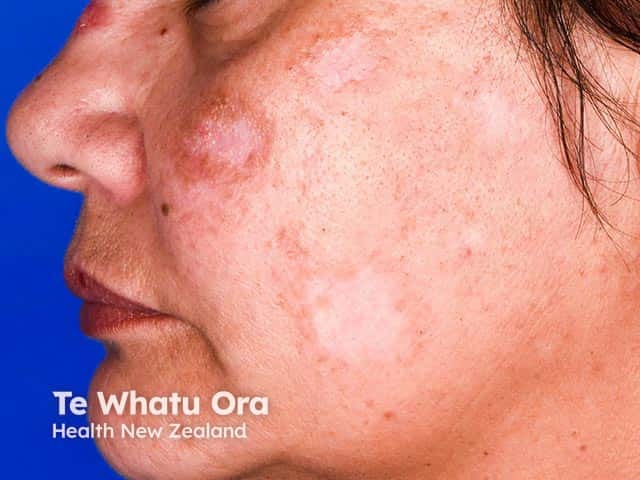
Active inflammatory discoid lupus erythematosus with hypopigmented scarred areas on the cheek (DLE-patient8)
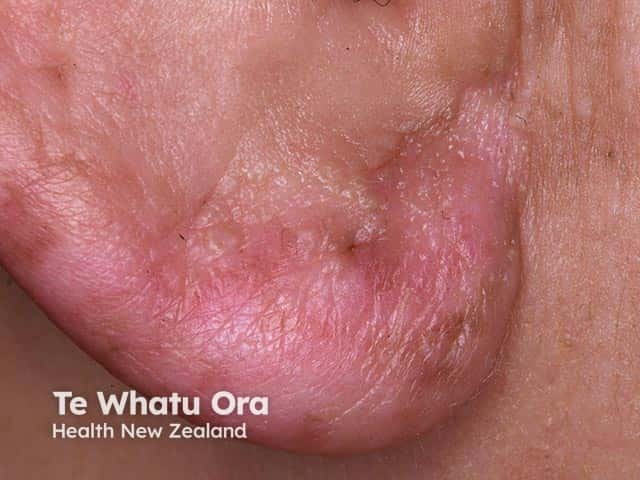
Well circumscribed scarred ear lobe due to discoid lupus erythematosus (DLE-patient8)
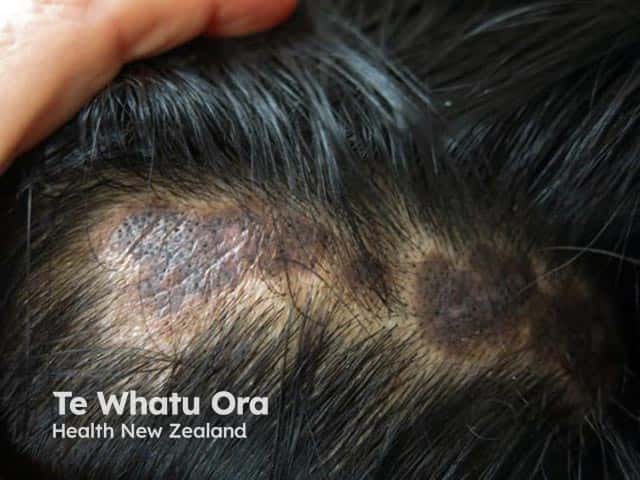
Scarring alopecia due to discoid lupus erythematosus (DLE-patient4)

erythematosus Discoid lupus erythematosus Scarring alopecia with follicular plugging in discoid lupus erythematosus (DLE-patient4)
DLE is more common in skin of colour. Hypo- and hyper-pigmentary change in those with skin of colour is especially noticeable and distressing.
Discoid lupus erythematosus is diagnosed from its distribution and the clinical appearance of the plaques. A patient with DLE should undergo a complete examination for other manifestations of lupus.