Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu, MD candidate, Keck School of Medicine, Los Angeles, USA. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy editor: Maria McGivern. June 2017.
Introduction
Causes
Demographics
Clinical features
Diagnosis
Differential diagnoses
Treatment
Outcome
Drug-induced nail disease is diagnosed when a medication affects nail growth or structure. Drugs may cause:
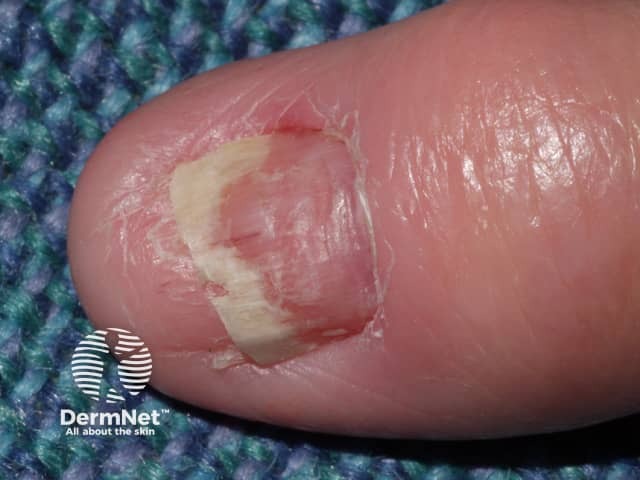
Nail plate deformity induced by acitretin
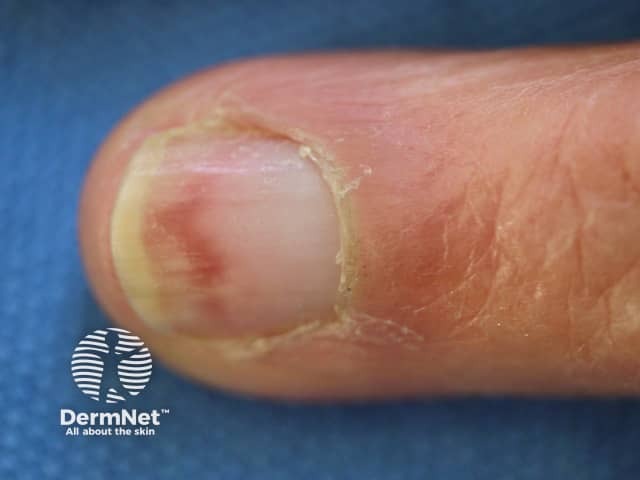
Nail dystrophy induced by hydroxyurea
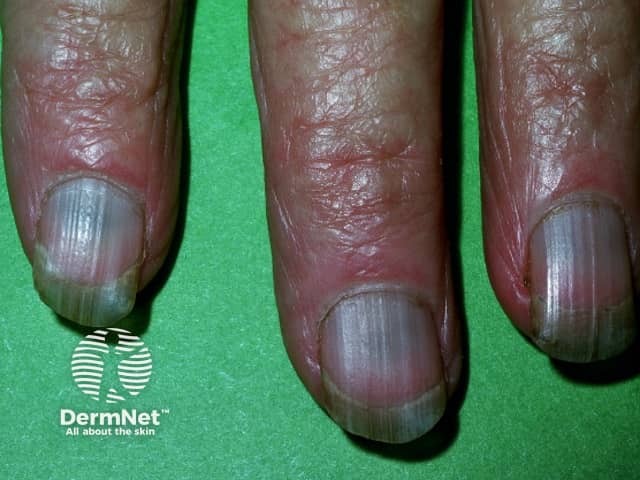
Discolouration induced by minocycline
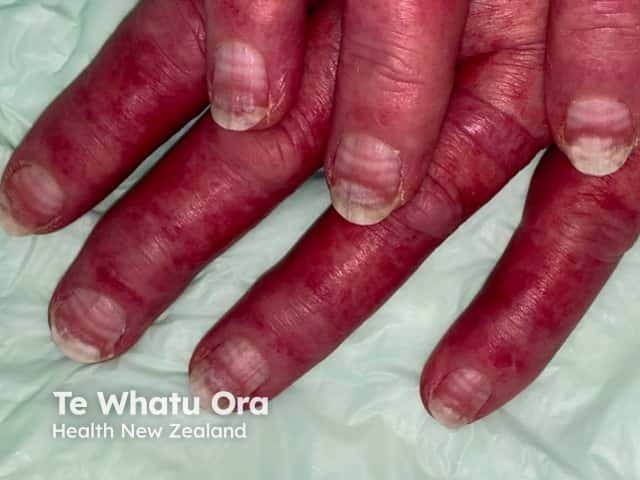
Muercke nails due to chemotherapy
Drugs can damage the nail matrix (the hidden part of the nail unit under the cuticle), the nail bed (the skin beneath the nail plate [the visible part of the nail]), periungual tissue (tissue situated around the nail), or blood vessels feeding the nail or nails.
In general, the higher the dose of the drug, the more likely it is to cause nail disease. A wide variety of medications have been reported to cause nail disease, but with a few exceptions (chemotherapy agents), it is generally rare.
Drug-induced nail disease is more common overall in older persons and those exposed to multiple medicines.
The signs and symptoms of drug-induced nail disease depend on the specific drug. They are often noticed some weeks or months after the drug has been commenced and may affect a single nail or, more often, all the fingernails (and sometimes the toenails). Symptoms include:
The temporary interruption of nail growth due to toxicity from a drug to the nail matrix results in:
The transverse lines move distally as the nail plate grows out normally.
Blanchable white bands that do not move distally are due to damage to the nail bed and are associated with chemotherapy. These are also called apparent leukonychia and Muehrcke lines.
Drugs that temporarily interrupt nail growth include:
Nail thinning, fragility and brittleness are due to diffuse damage to the nail matrix and nail plate. These signs are most often caused by long-term use of chemotherapy agents and retinoids. Damage to the distal nail plate causes:
Drugs can also cause nails to grow more quickly or more slowly.
Toxicity to the nail bed results in onycholysis (the lifting of the nail plate from the nail bed causing nails to appear white, yellow or brown — due to subungual haemorrhage). It is often painful. Photo-onycholysis is onycholysis following exposure to ultraviolet radiation and generally does not affect thumbnails.
Drugs that can cause onycholysis and photo-onycholysis include:
Damage to the nail folds (the skin folds that frame and support the nail on three sides) results in:
Damage to the nail folds is associated with the use of:
Splinter haemorrhage is a short longitudinal line within the nail due to capillary bleeding and grows out with the nail.
Drugs that cause splinter haemorrhage, and subungual haemorrhage, include:
Nail pigmentation can also be drug-induced. This includes:
The diagnosis of drug-induced nail disease is made by taking a careful history and by a thorough clinical examination.
Infections and spontaneous nail dystrophies may appear similar to drug-induced nail disease. Conditions that appear similar to drug-induced nail disease include:
There is no specific treatment for drug-induced nail disease.
Where possible, the causative drug is stopped; however, it may be continued if the nail symptoms are tolerable, especially, if there is no suitable alternative medication.
If nails are brittle:
In the case of onycholysis, protect the nail bed from ultraviolet exposure by applying nail enamel.
Paronychia and nail fold pyogenic granulomas are treated with topical steroids, antibiotics and cautery.
Nail diseases caused by drugs may sometimes resolve without discontinuing the causative medication; this is particularly true of onycholysis. Most nail abnormalities improve when the causative drug is discontinued, but in some cases the nail abnormalities are permanent. It may take months or, in the case of toenails, years for the nails to return to their normal appearance due to their slow growth.