Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Marianne Kim, Medical Student, University of Auckland, New Zealand, 2012.
Facial psoriasis is a chronic skin condition in which there are one or more, persistent, thickened, red and dry patches on the face.
Psoriasis is a common chronic inflammatory skin disease that may affect any skin site. Facial involvement occurs at some time in about half those affected by psoriasis. Although it is usually mild, facial psoriasis is occasionally very extensive involving the hairline, forehead, neck, ears and facial skin.
It is extremely rare to have psoriasis occurring solely on the face. Most patients also have scalp psoriasis and they may also have moderate to severe psoriasis at other sites.
Patients with facial psoriasis often suffer from psychosocial problems due to the presence of unsightly red, scaly plaques on highly visible areas.
Facial involvement presents as a therapeutic challenge because facial skin is thin, sensitive and more complicated to treat.
Facial psoriasis has various clinical presentations. There are three main subtypes:
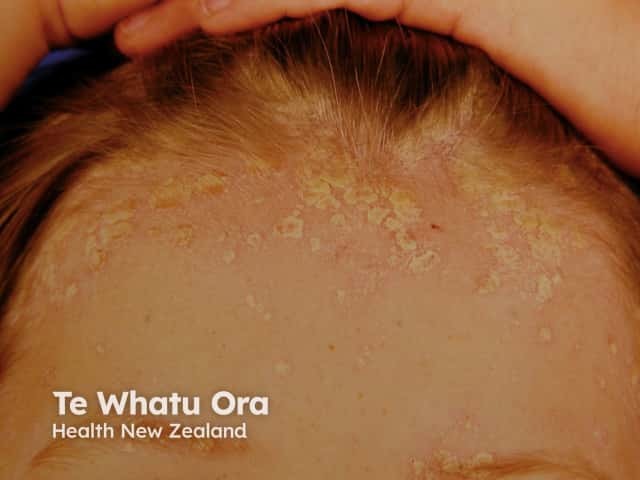
Facial psoriasis
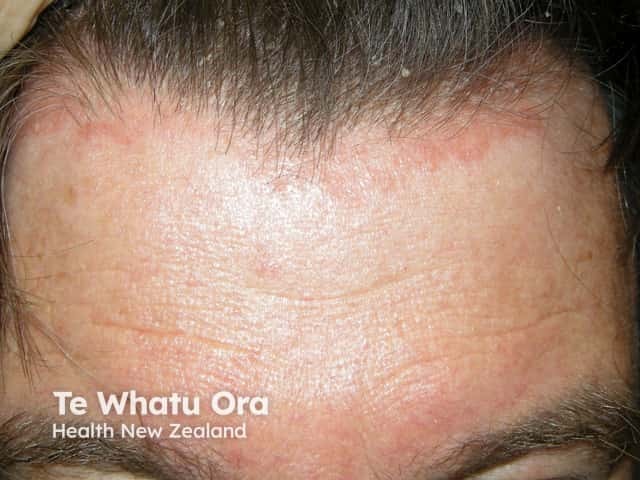
Facial psoriasis
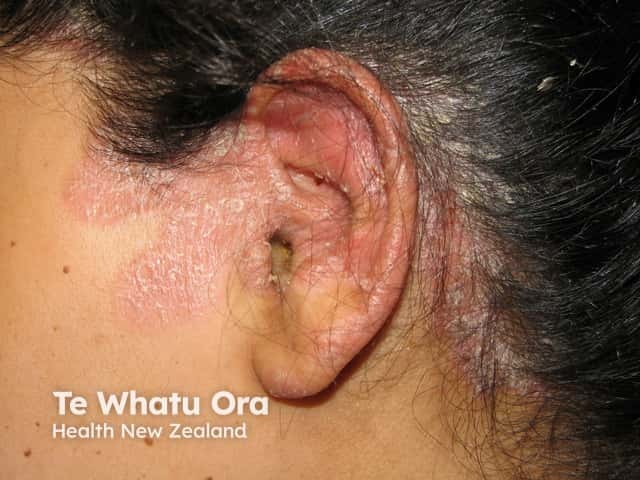
Facial psoriasis
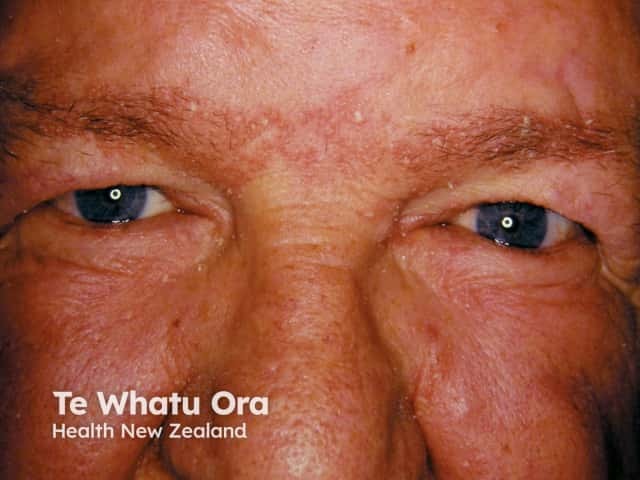
Facial psoriasis
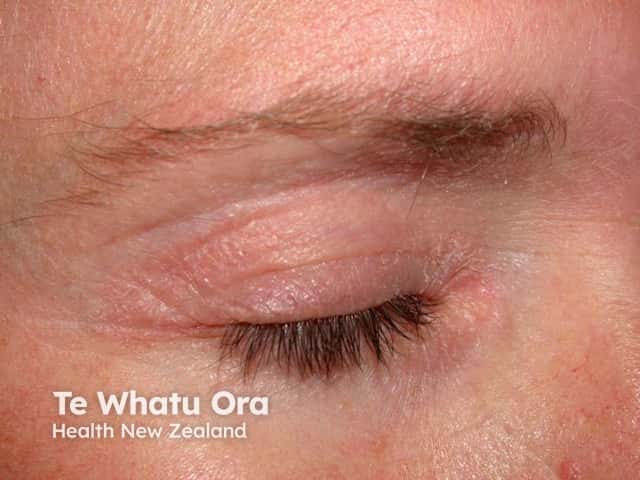
Eyelid psoriasis
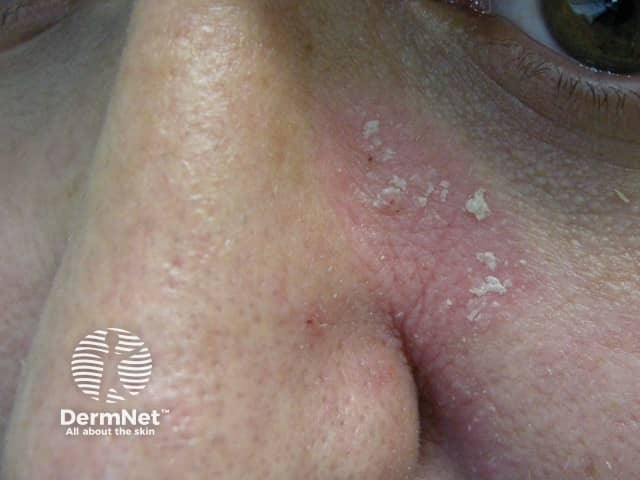
Facial psoriasis
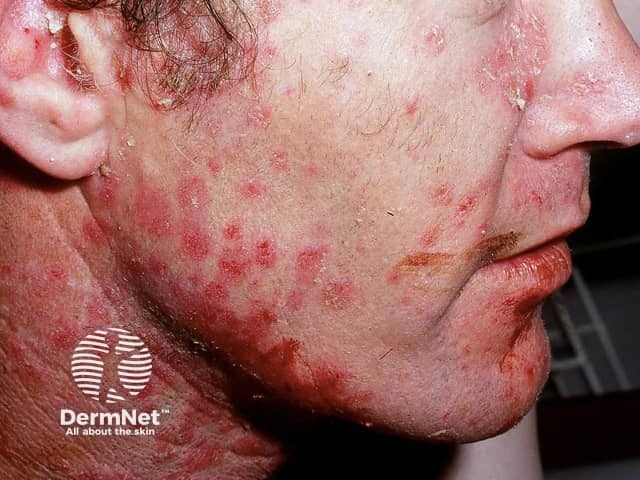
Facial psoriasis
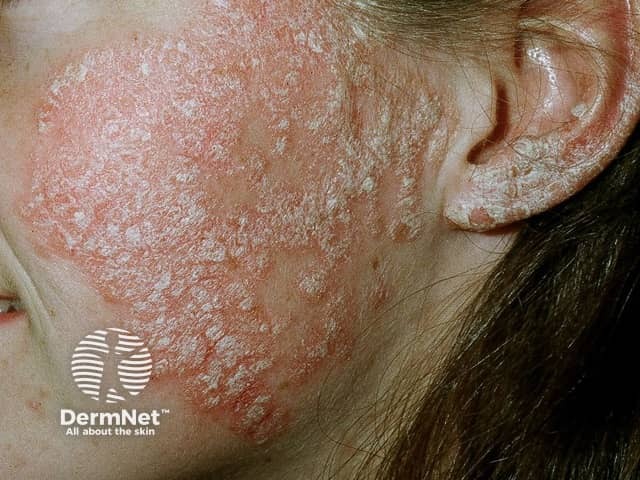
Facial psoriasis
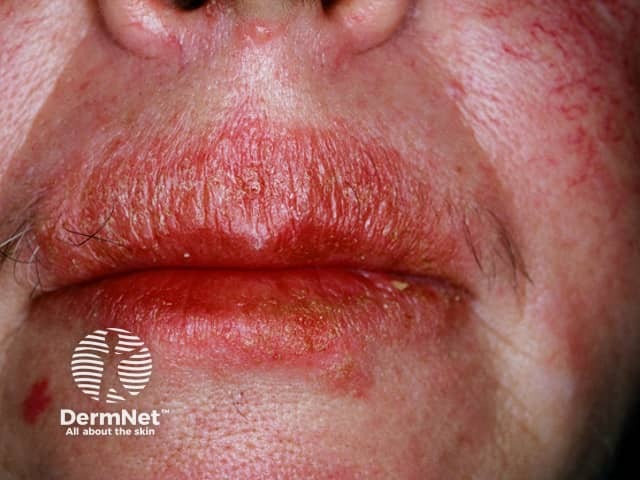
Facial psoriasis
See more images of facial psoriasis.
The causes of facial psoriasis are the same as for psoriasis in general. Psoriasis is associated with inappropriate activation of the immune system resulting in inflammation and increased proliferation of skin cells. There is a genetic predisposition, but environmental influences are important, including stress, infection, injuries and certain medications.
Facial psoriasis may also be aggravated by:
There is no cure for facial psoriasis, but satisfactory control of the disease is possible for most patients using topical therapy. General skin care may include:
Mild or moderate strength topical steroids reduce inflammation and relieve itching. Side effects of corticosteroids restrict the potency and duration of use on the face. These include:
Hydrocortisone is generally safe. More potent topical steroids are best used on the face for only a few days each month.
The topical calcineurin inhibitors pimecrolimus cream and tacrolimus ointment may be prescribed off-label for facial psoriasis and can be very effective. They are particularly useful on eyelid skin. In New Zealand, these preparations are not currently subsidised by PHARMAC (February 2019).
Sun exposure or prescribed phototherapy is often helpful for facial psoriasis.
It is unwise if there is photosensitivity or significant sun damage, such as solar/actinic keratoses or skin cancer.
Severe facial psoriasis sometimes warrants treatment with tablets or injections such as methotrexate, ciclosporin, acitretin or biologic agents. Patients should be under the care of an experienced dermatologist and should be carefully monitored.
Facial psoriasis tends to persist, although its severity may vary with season, stress and other factors. It may be a marker of more severe disease with early-onset, long duration and more extensive plaques.