Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Susan Simpkin, Dermatology Registrar, Green Lane Clinical Centre, Auckland, New Zealand, 2012.
Introduction
Clinical features
Diagnosis - interstitial granulomatous dermatitis
Introduction - Palisading neutrophilic granulomatous dermatitis
Diagnosis - palisading neutrophilic granulomatous dermatitis
Clinical associations
Treatment
Interstitial granulomatous drug reaction
Granulomatous dermatitis describes several disorders characterised by their histological appearance.
Interstitial granulomatous dermatitis is a rare skin disorder in which there is a particular pattern of granulomatous inflammation.
The classic original clinical description of interstitial granulomatous dermatitis was of linear erythematous palpable cords on the lateral aspects of the trunk, called 'the rope sign'. However, several different types of rash have since been described with the same histological appearance.
The features of interstitial granulomatous dermatitis are variable.
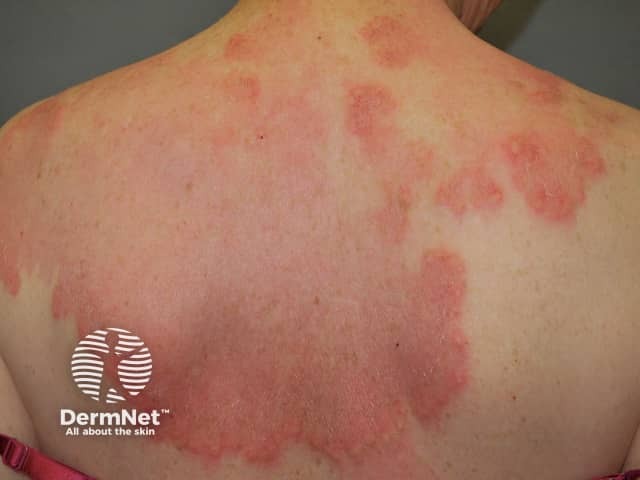
Interstitial granulomatous dermatitis
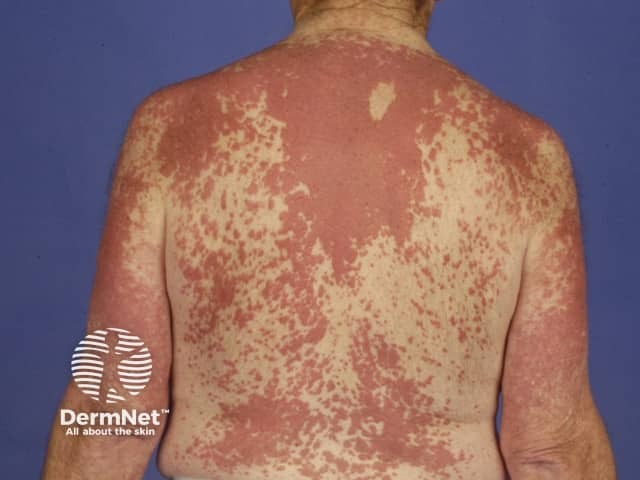
Interstitial granulomatous dermatitis
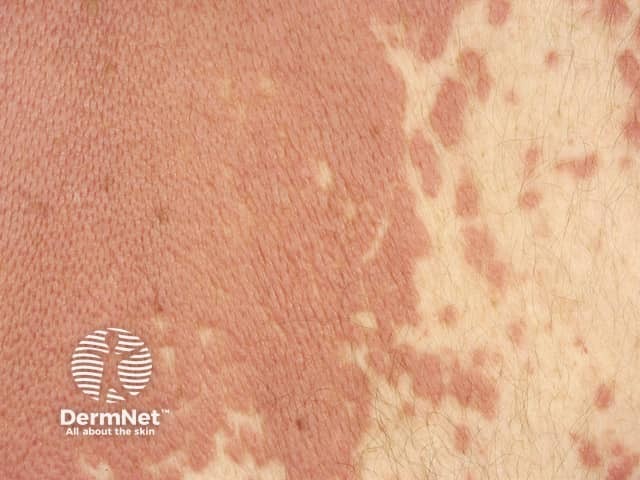
Interstitial granulomatous dermatitis
Interstitial granulomatous dermatitis is diagnosed by a pathologist on examining a skin biopsy. The characteristic histological features of interstitial granulomatous dermatitis are:
Granuloma annulare and interstitial granulomatous dermatitis may appear similar clinically and histologically. Granuloma annulare also presents with papules and plaques, but these are typically on the back of the hands or feet, whereas the trunk is a more common site for interstitial granulomatous dermatitis. Granuloma annulare is less often associated with autoimmune diseases.
The characteristic histological features of granuloma annulare are:
Palisading neutrophilic granulomatous dermatitis was first described as crusted umbilicated papules on the elbows arising in patients with rheumatoid arthritis (Winkelmann granuloma) and eosinophilic granulomatosis with polyangiitis (Churg-Strauss syndrome).
Several different types of rash have been described with the same histological appearance including annular plaques on the trunk. Lesions are often tender and may ulcerate.
Palisading neutrophilic granulomatous dermatitis is diagnosed on skin biopsy. The characteristic histological features of palisading neutrophilic granulomatous dermatitis are:
Palisading granulomas seen have also been described as miniature ‘Churg-Strauss granulomas’ or flame figures, with degenerated collagen enveloped by eosinophils resembling a flame. Flame figures are also seen in the pathology of Wells syndrome.
Several conditions have been noted to arise in association with interstitial granulomatous dermatitis. There is less information about associations with palisading neutrophilic granulomatous dermatitis.
Both forms of granulomatous dermatitis have often arisen in people with other conditions considered autoimmune in origin, implying an immune-complex mechanism may be involved in the pathogenesis [2]. These have included the following conditions.
In a literature review of 15 patients with interstitial granulomatous dermatitis, autoantibodies identified on blood testing included rheumatoid factor (RhF), antinuclear factor (ANA), thyroglobulin, SS-A Histone, DNA histone and ANCA [4].
There are some reports of association of malignancy with interstitial granulomatous dermatitis. In one case, the lesions cleared after lung cancer was treated [5]. Rare associations of granulomatous dermatitis with leukaemia [6], lymphoma, breast cancer, hypopharyngeal squamous cell carcinoma and endometrial neoplasia have been reported.
Granulomatous dermatitis typically flares and remits. Successful treatments have included:
One case associated with SLE responded well to systemic steroids after 15 days [2].
Although tumour necrosis factor (TNF)-alpha inhibitors have been recently described as inducing interstitial granulomatous dermatitis [7], etanercept has been used in interstitial granulomatous dermatitis associated with rheumatoid arthritis with complete skin clearance and improvement in arthritis [8].
Interstitial granulomatous dermatitis induced by medications is known as an interstitial granulomatous drug reaction. It is thought to be a distinct clinical and pathological entity. It presents as annular plaques, and nodules on the trunk, arms, medial thighs and skin folds. The rash resolves when the responsible drug is withdrawn.
Interstitial granulomatous drug reaction is diagnosed by skin biopsy. The characteristic histological features of interstitial granulomatous drug reaction are:
Medications that have been reported to be implicated in interstitial granulomatous drug eruption include: