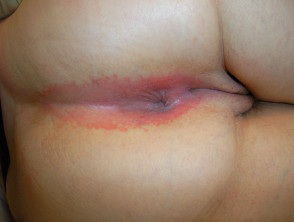
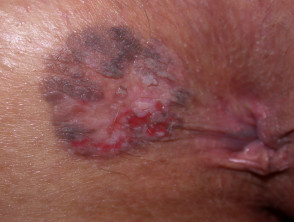
What is a perianal dermatosis?
A perianal dermatosis is a rash or skin change around the anus, between the buttocks.
Who gets perianal dermatoses?
Patients with a pre-existing inflammatory dermatosis may have anogenital involvement as commonly occurs with psoriasis, or the dermatosis predominantly involves the anogenital area (eg, lichen sclerosus).
Patients are often embarrassed, and it may be difficult for them to visualise and examine the area. Their quality of life can be markedly affected yet do not mention it at medical appointments.
What are the causes and clinical features of perianal dermatoses?
A compromised skin barrier may predispose to a perianal dermatosis. Advanced age, faecal incontinence, immobility, hyperhidrosis, obesity, occlusion from clothing, and poor anal hygiene all contribute to skin barrier dysfunction.
Because of the effects of occlusion and maceration, scaling may not be apparent, and the skin signs may be non-specific, although there are usually clinical clues to make the diagnosis. It is important to ask about and look for skin problems elsewhere.
Perianal dermatoses often present with itch (see Itchy anus). Pruritus ani means itch around the anus with no visible skin change when used in the strict sense.
Intertrigo is an inflammatory rash in a skin fold, often due to sweat and friction, an inflammatory dermatosis, or infection.
Contact dermatitis of the perianal skin
Irritant contact dermatitis
Perianal irritant contact dermatitis can be due to:
- Faecal soiling resulting from an incompetent anal sphincter
- Skin irritants in skin cleansers and alkaline soaps
- Moisture from gastrointestinal contents after consumption of spicy food or cathartics
- Sweating.
Allergic contact dermatitis
Topical allergens that can cause perianal allergic contact dermatitis include:
- Ingredients of topical haemorrhoid preparations, such as local anaesthetics benzocaine and lignocaine
- Fragrances and preservatives, especially in wet wipes
- Lanolin
- Ingredients of body washes
- Medicaments including neomycin
- Nail varnish.
Inflammatory dermatoses involving perianal skin
Psoriasis
Flexural psoriasis often involves the anogenital skin and natal cleft, presenting with well-demarcated symmetrical, non-scaly erythema. There will be signs of psoriasis elsewhere such as in other skin folds, scalp, or nails.
Seborrhoeic dermatitis
Seborrhoeic dermatitis typically affects the scalp, eyebrows, and nasolabial folds, but can involve the perineum and intergluteal fold.
Atopic dermatitis
Although the cubital and popliteal fossae are more commonly involved, the intergluteal fold can also be affected in atopic dermatitis.
Lichen planus
Perianal lichen planus may be seen as an extension of vulval disease and has been reported to transform to anal squamous cell carcinoma.
Lichen sclerosus
Perianal lichen sclerosus shows a female predominance usually associated with vulval disease. There is an associated risk of perianal squamous cell carcinoma.
Lichen simplex
Lichen simplex commonly complicates perianal itch of various causes.
Hidradenitis suppurativa (acne inversa)
Clinical features of hidradenitis suppurativa include comedones, papules, nodules, draining sinuses, and abscesses in apocrine gland-rich skin. Fistula formation may occur in the perianal region. Genital Crohn disease can also result in perianal fistulae but lacks the other features of hidradenitis suppurativa.
Infections of the perianal skin
Erythrasma
Erythrasma is an infection caused by Corynebacterium minutissimum. It is often asymptomatic and causes an erythematous brown patch with maceration and slight scaling in a skin fold. Characteristic coral red fluorescence is seen with a Wood lamp.
Streptococcal and staphylococcal infections
Perianal streptococcal dermatitis is seen in children as a sharply demarcated, beefy erythematous ring around the anus with possible fissuring and exudate.
Candidiasis
Perianal candidal intertrigo presents as soreness and irritation with bright red erythema and satellite lesions extending into the natal cleft.
Tinea
Tinea cruris is usually due to T. rubrum and presents as an asymmetrical erythematous patch with a scaly, annular border in the groin. Perianal tinea is uncommon.
Other perianal infections
Pinworm infestation typically causes perianal itch at night and perianal redness or dermatitis.
Viral warts and herpes simplex virus can infect the perianal skin.
Blistering skin disorders of the perianal area
Pemphigus vulgaris often begins in the oral mucosa or the anogenital area. Benign familial pemphigus (Hailey-Hailey disease) typically involves skin folds including the skin around the anus.
Perianal malignancies
Malignancies of the perianal skin may resemble a rash.
Extramammary Paget disease
Extramammary Paget disease is an intraepithelial adenocarcinoma which can involve the perianal skin particularly in males. Lesions may appear as itchy, unilateral or asymmetric, erythematous or pigmented plaques with scaling, ulceration, or crusting.
Anal intraepithelial neoplasia
Anal intraepithelial neoplasia (AIN) is a superficial squamous-cell carcinoma usually associated with human papillomavirus (HPV) 16 and 18, often seen in HIV/AIDS. The clinical features are non-specific, presenting as a bleeding, well-defined red, scaly erythematous rash-like plaque on the perianal skin.
Perianal dermatoses
see also perianal lichen sclerosus images, genital psoriasis images, mammary and extramammary Paget disease of the skin images, anal cancer images
How is a perianal dermatosis diagnosed?
Perianal dermatoses are diagnosed by taking a comprehensive history, including hygiene practices, use of tight-fitting clothing, bowel habits, use of topical preparations, systemic symptoms, associated medical conditions, personal and family history of skin conditions, and response to treatment.
Following clinical examination of the perianal area and skin generally, investigations may include:
- Swabs for bacterial culture, especially in children
- Skin scrapings for fungal culture, if indicated
- Skin biopsy may be needed, in particular to diagnose extramammary Paget disease and AIN.
If allergic contact dermatitis is suspected, patch testing is required to identify the allergen.
Anal manometry can be performed to identify abnormalities of the anal sphincter, which may contribute to faecal incontinence and/or constipation.
What is the treatment for perianal dermatoses?
Following diagnosis, it is important to relieve symptoms, restore the skin barrier, prevent recurrence, and treat the specific condition.
General measures
- Hygiene — thorough cleansing of the area with tepid water and avoidance of excessive rubbing when wiping away faecal matter should be encouraged. Irritating skin cleansers, alkaline soaps, and wet wipes should be avoided. Soft, wet washcloths, or drying with a hair dryer, may be less irritating than toilet paper.
- Moisturising cream — maintenance of the skin barrier with a lotion or cream (see Emollients and moisturisers).
- Zinc oxide-based topicals — soothe and augment the skin barrier, reducing irritation, and promote healing (see Barrier cream).
- Avoid topical irritants.
- Minimise the ingestion of spicy foods and foods that cause acidic, loose, or frequent stools. Foods that promote regular bowel movements, such as those high in fibre, are advisable.
- Limit wearing clothing that is nonporous and tight-fitting, which may trap sweat and bacteria.
- Avoid scratching — pruritus can be addressed by avoiding heat and applying cold compresses. If available, a sitz bath may be helpful.
- Biofeedback and exercises of the muscles of the anal sphincter and pelvic floor may have a role in some cases.
- Avoid topical allergens identified on patch testing.
Specific treatments
Specific treatments for perianal dermatoses depend on the diagnosis, but may include the following.
- Topical corticosteroids
- Creams are preferred over ointments for this area.
- Avoid potent topical steroids except for lichen sclerosus and lichen planus.
- Topical calcineurin inhibitors
- Calcineurin inhibitors may be used longer treatment than topical steroids and are less likely to cause skin atrophy.
- Topical local anaesthetics
- Topical local anaesthetics should be used with caution because of the risk of allergic contact dermatitis.
- Other
- Weak coal tar preparations for psoriasis.
- Topical antifungal medications for tinea cruris and candidiasis.
- Antibiotics for bacterial infections.
- Surgery may be appropriate for malignant perianal conditions. Other options such as imiquimod or radiotherapy may be considered.